12 cases of tuberculous sacro-iliitis (34,3 %), from 35 infectious sacro-iliitis, were identified in adults, including 8 (67%) women and 4 (33%) men (Figure 1).
The average age of diagnosis was 53 ± 17 years.
The sacro-iliitis was unilateral in 11 (91,7 %) cases, the right joint was effected in 5 cases and the left joint in 6 cases. It was bilateral in one case (8,3 %).
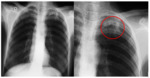
One patient was treated for lymph nodes tuberculosis, another was treated for pericardial tuberculosis.
Low back pain, fever and night sweats were presented in all cases.
Physical examination revealed pain by pressure on the iliac wings ans sacroiliac joints.
Blood test showed inflammation in 11 cases (in 91,7 %, ESR was positive).
Tuberculosis skin test was performed in 7 cases. It was positif in 6 cases (85 %).
Quantiferon-TB-Gold test was performed in 2 cases. It was positif (100%).
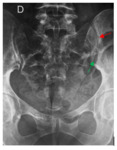
Plain antero posterior radiograph was performed in 7 cases. It was abnormal in all cases. It showed :
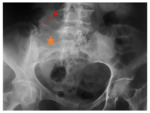
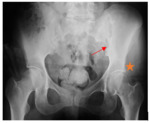
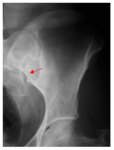
· Widening of the joint space (n=3) (figure 2,3,4).
· Narrowing of the joint space (n=3).
· Erosions along the joint margins (n=4) (Figure 2).
· Sclerosis (n=5).
· Destructive lesion of the sacro-iliac joint (n=3) (Figure 3,4,5).
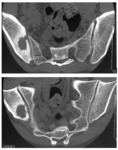
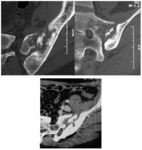
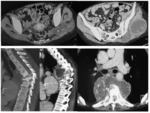
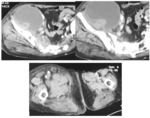
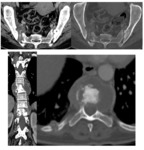
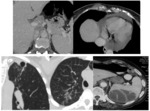
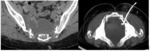
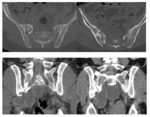
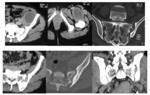
Computed tomography (CT) of the pelvis was performed in all cases, it was abnormal in all cases and it showed (figures 7,8,9,10,11) :
· Arthritis in 12 cases.
· Bone sequesters in 7 cases.
· Soft tissues involvement in 9 cases.
· Other associated localisation was diagnosed.
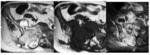
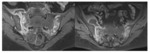
The MRI directed towards the diagnosis in 4 cases. It shows (figures 13,14) :
· Bone marrow oedema.
· Soft tissue involvement : soft tissue swelling and/or abscess.
Closed biopsy of sacro-iliac joint were performed in 5 patients. Histology revealed granuloma and caseation in 3 cases (figure 15).
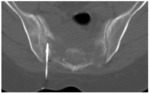
The puncture of abses (figure 16) was performed in 4 cases, Acid-Fast bassili were isolated and PCR was positif in two patients.
In the other cases, the diagnosis was retained on suggestive clinical and biological arguments.
The delay between the onset of symptoms and the final diagnosis ranged between 100 and 712 days.
The follow up ranged from 1 to 5 years. CT scan was performed in 6 cases and MRI in one case.
Radiological improvement was seen in 3 cases (Figures 17,18).