Type:
Educational Exhibit
Keywords:
Performed at one institution, Not applicable, Inflammation, Infection, Abscess, Diagnostic procedure, Ultrasound-Power Doppler, Ultrasound-Colour Doppler, Ultrasound, Liver, Emergency, Abdomen, Abdominal Viscera
Authors:
A. A. Ramos Muñoz, I. Tamayo-González, J. L.ABRALDES, A. Perez Lara, M. M. MOLINERO-CASARES, J. Vicente-Romo; Málaga/ES
DOI:
10.26044/ecr2020/C-09352
Background
The clinical status of the patient and certain abnormalities in blood test results such as leukocytosis and acute phase proteins increase can guide to AC diagnosis; however, these findings are nonspecific and oftenly are not present. Ultrasound imaging (US) is the fist-line imaging modality to be performed due to its advantages such as its low cost and high disponibility allowing to be performed even at the patient’s bedside. In addition, this imaging technique does not use ionizing radiation so it can be repetead if necessary without the additional radiation cost, and it is an optimal imaging technique to assess the gallbladder due to its excellent capacity to evaluate cystic structures.
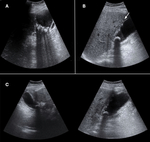
During the US examination gallstones can be identified as hyperechogenic rounded images producing associated posterior shadow. Sonographic Murphy's sign can be evaluated by pressing the visualized gallbladder with the transducer, considering this sign as positive if it leads to an increase in tenderness. The presence of both main findings (confirmed gallstones and sonographic Murphy's sign) provides a 95% and 92% PPV and PPN respectively. Other US signs suggestive of AC are gallbladder wall thickening (over 3 mm), gallbladder distention -wider than 4 cm and longer than 10 cm- or spherical shape of the gallbladder. Adjacent free fluid and fat hyperechogenicity can be present, while lithiasis or biliary sludge are detected withing the gallbladder (Figure 1).
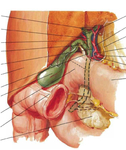
However, these signs may be occasionally challenging to detect AC. Wall thickening and pericholecystic free fluid are nonspecific signs present as well in other entities such as acute pancreatitis, chronic kidney disease, congestive heart failure, hepatitis, cirrhosis/portal hypertension, portal thrombosis or hypoproteinemia. Murphy’s sign can be masquerade in patients receiving high analgesic dose or in patients with history of cognitive decline. In addition, US examination is occasionally limited by certain factors -increase of abdominal fat thickness, excessive intestinal gas content or lack of patient collaboration during the exam- and the inexperience of the radiologist. These factors can lead to false positives and false negatives that occasionally may difficult the AC diagnosis. Moreover, there are other entities involving other anatomical structures in the vicinity of the gallbladder that clinically can simulate AC, constituting a diagnostic challenge (Figure 2).
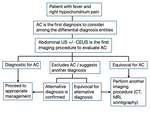
Considering all these factors, a decision-making imaging algorithm is proposed to achieve an accurate diagnosis (Figure 3).