A. THE IMPORTANCE OF USING THE OPTIMAL TECHNIQUE FOR ACQUIRING AND READING THE IMAGES:
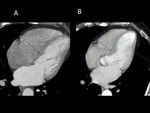
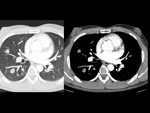
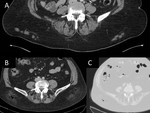
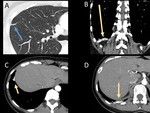
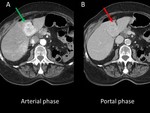
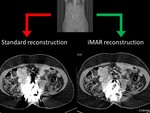
1-Dedicated CT protocol: Hypervascular metastases are more conspicuous in the arterial phase. In typically hypervascular tumors such as GIST, renal cell carcinoma, melanoma, neuroendocrine... consider acquiring also the arterial phase (Figure 1).
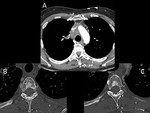
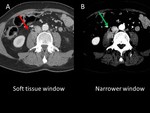
2-Optimized image review: choose the right window display. Review the soft tissues with a narrower window, which helps detect some lesions less conspicuous because of their density, especially in atypical locations that tend to go unnoticed: intramuscular metastases, bowel implants, spinal canal lesions... (Fig 2).
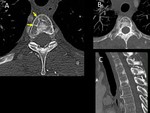
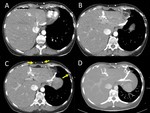
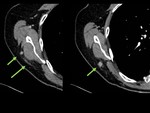
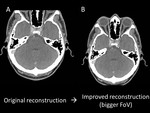
3-If necessary, reconstruct again the acquired data. For example, use software that reduces the metal artifact (Figure 3) or expand the field of view if any area of interest is missing (often in the neck, shoulders and peripheral soft tissue) (Figure 4).
B. RELEVANT ANATOMY IN ONCOLOGIC IMAGING:
1-Ectopic tissue foci of different glands can simulate nodules or adenopathies. The keys tips to not confuse these findings with tumor lesions are:
- remember the embryogenesis of these organs
- these foci of ectopic tissue have a typical location
- its CT density and its MR signal are the same as those of the normal gland.
The two most characteristic cases of ectopic tissue mimicking malignancy are:
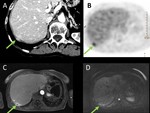
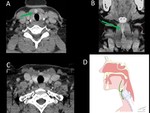
- hyperdense nodules of ectopic thyroid tissue in the neck or upper mediastinum along the migration route of the gland during embryonic development (Figure 5), and
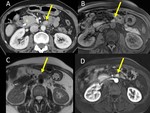
- foci of heterotopic pancreatic tissue in the wall of the digestive tract (Figure 6).
2-Pseudo-lesions and lesions whose characteristic anatomical location should prevent us from confusing them with tumor-related lesions:
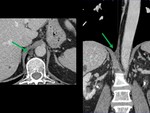
- An enlarged cisterna chyli should not be mistaken with an enlarged retrocrural lymph node. Take into account its typical location and density, and its elongated morphology best seen in coronal reconstruction (Figure 7).
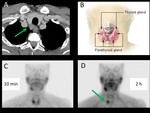
- Lesions in the parathyroid glands should not be mistaken with cervical or mediastinal lyphadenopathies. Look at the typical location of the glands and to remember the specific nodal territories (Figure 8).
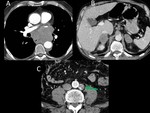
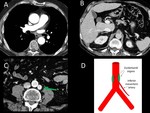
- A very caracteristic location of extra-adrenal paraganglioma is the Zuckerkandl body and it can mimic paraaortic lymhadenopathy (Figure 9 and Figure 10). Paragangliomas can be hypermetabolic in 18FDG-PET / CT. They are usually benign lesions, They usually have a typical location along the sympathetic chains and a characteristic radiological aspect, with intense relapse after the administration of contrast and, sometimes, an area hypodense central secondary to hemorrhage.
The case presented in Figures 9 and 10 illustrates a bonus tip: we should suspect that a lesion is not related to the patient's known cancer when:
- It is in a very atypical location for that tumor
- Its morphological features are clearly different from those of the primary tumor and the rest of the metastases
- Its response to treatment diverges from the rest of the lesions
3-Enlarged lymph nodes distant form the primary tumor but in typical locations. Virchow´s node is an enlarged left supraclavicular node in digestive tumors with lymphatic drainage through the thoracic duct, which ends next to the left subclavian vein (Figure 11).
C. SYSTEMIC MANIFESTATIONS OF CANCER AND THEIR IMAGING FEATURES. NOT EVERYTHING IS A SPACE-OCCUPYING LESION!
Although radiologists tend to thinking of cancer as space-occupying lesions, cancer is a heterogeneous group of diseases with systemic manifestations. Many times we can be the first to detect these systemic phenomena if we are aware of their imaging features. The two most obvious examples are the predisposition to thrombosis and infections. We present some others:
1-Carcinoid heart disease: Carcinoid heart disease is part of the carcinoid syndrome. Fibrous tissue deposits in the right heart valves and endocardium causing valvular dysfunction and, potentially, right heart failure. The growth of the right heart chambers can be observed incidentally on the CT scans and/or MRI of these patients, whose heart disease is often asymptomatic and underdiagnosed (Figure 12).
2-Pseudolesions mimicking metastases in superior vena cava syndrome:
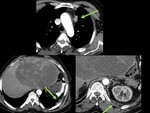
- “Vanishing bone metastases“: Vertebral venous congestion caused by superior vena cava syndrome can simulate sclerotic vertebral metastases. When in doubt, repeating the CT scan without contrast will show the disappearance of the lesions (Figure 13 and Figure 14).
- "Hot liver sign": Superior vena cava obstruction can cause areas of focally increased blood flow in the collateral veins of the left hepatic lobe (Figure 15).
3-Gynecomastia as unusual presentation of choriocarcinoma, due to the secretion of Beta-hCG)-by the tumor (Figure 16).
D. EFFECTS OF SYSTEMIC THERAPY CAN SIMULATE TUMOR SPREAD
To read cancer patients´ studies it is essential to know what treatment the patient is receiving and since when to assess response and toxicity. Moreover some side effects of the drugs can be confused with tumor progression They are drug-specific and were not present in the baseline study.
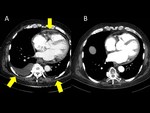
1-Fluid Retention Associated with Imatinib: Imatinib is used mainly for GIST and chronic myeloid leukemia and typically causes fluid retention. The appearance of ascites without implants in patients with GIST should make us suspect this phenomenon before considering disease progression. Since GIST does not spread to the pleura or pericardium, effusions in these cavities are almost always related to treatment. (Figure 17).
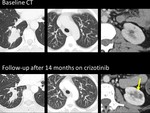
2-Crizotinib-induced complex renal cysts: Crizotinib is a c-kit tyrosin-kinase inhibitor used in ALK-mutant lung adenocarcinoma. Renal cysts grow or appear de novo during treatment in up to 16% of patients treated with crizotinib, and around a quarter of them are complex. They should be recognized, do not mistake with renal metastases or renal tumors (Figure 18). They lack clinical relevance and usually regress at the end of the treatment.
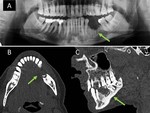
3-Bisphosphonate-related osteonecrosis of the jaw: Bisphosphonates are used to treat bone metastases. Osteonecrosis of the jaw is a well-known side effect of prolonged treatment with these drugs that should not be confused with a lytic metastasis (Figure 19). Also characteristic of bisphosphonates is the osteonecrosis of the external auditory canal, although this complication is less frequent and less known.
4-Granulomata secondary to subcutaneous injection of somatostatin analog: the differential diagnosis is between injection site reactions and metastases. Typical imaging features, symmetry and awareness of this treatment are key to avoid this pitfall (Figure 20).
E. REVIEWING THE MEDICAL RECORD AND OLD FILMS WILL SAVE YOU FROM MISTAKES. SEQUELAE OF REMOTE DISEASES AND TREATMENTS MAY SIMULATE METASTASES.
The following cases were initially mistaken with metastatic disease at our institution and a careful review of the medical record was key to avoid definitive misdiagnosis.
1-Tick-borne lymphadenopathy (TIBOLA) mimicking nodal recurrence: TIBOLA was first described in 1997: rickettsial inoculation after a tick bite results in subcutaneous inflammation and enlarged regional lymph nodes in the absence of a rash. In this case, the extremely unusual location of the lesions should make us consider alternative diagnoses to the relapse of a gynecological tumor (Figure 21).
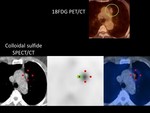
2-Thoracic esplenosis mimicking pleural implants. The definitive diagnosis of thoracic splenosis can be performed by nuclear medicine, and biopsy is unnecessary (Figure 22 and Figure 23). But it is important to suspect this entity by the typical findings and associate them with the history of splenic and diaphragmatic rupture.
3-Talc pleurodesis sequelae mimicking pleural implants:(Figure 24). Sequelae of pleurodesis have characteristic radiological features, but it is necessary to know the medical history to relate it to the findings. They can be hypermetabolic on PET/CT.
4-Dropped gallstones mimicking peritoneal implants: Dropped gallstones are a well-known pitfall in cancer patients, especially when they are not calcified (Figure 25). Surgical history of cholecystectomy with bile and gallstones spillage to the peritoneal cavity is key. PET/CT and MRI features can further confuse the diagnosis, as in this case.


![Fig. 11: Staging CT scan for locally advanced gastric neoplasm. Left supraclavicular mass (Virchow´s node) corresponds to a stage IV. The drawing (Henry Vandyke Carter [Public domain] https://commons.wikimedia.org/wiki/File:Gray599.png) shows the anatomy of the thoracic duct draining at the origin of the left brachiocephalic vein, into the systemic (blood) circulation at the junction of the left subclavian and internal jugular veins.
References: (Henry Vandyke Carter [Public domain] https://commons.wikimedia.org/wiki/File:Gray599.png](https://epos.myesr.org/posterimage/esr/ecr2020/155949/media/893914?maxheight=150&maxwidth=150)