Learning objectives
To implement new hands-on training exercises in 3D printing technology within the course: “Computer Assisted Surgery and Rapid Prototyping for Radiographers”
To understand commonly used 3D printing technologies in medicine
To evaluate learning outcome by means of a self-assessment questionnaire
Background
3D printing applications in medicine are steadily increasing. One major application of 3D printing technology is the production of replicas of patient’s anatomy. The production of these models is based mainly on cross-sectional images of CT, CBCT or MRI Scans. These accurate models are produced by means of Rapid Prototyping technologies such as 3D printers. Due to the high depiction accuracy of these models, they have been used for operation planning and simulation of complex maxillofacial surgeries. Through this application it is possible e.g. prior...
Findings and procedure details
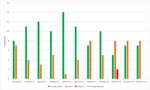
Stereolithography 3D printer apparatus was acquired from our department in order that students perform the whole 3D printing process. Small groups (2-3 students) were formed. Besides the main steps of image segmentation and 3D visualization and surgery simulation additional practical exercises were introduced and accomplished (Figure 1) in small groups.
Original base hands on training at PC
CT image segmentation,
3D visualization and surgery simulation,
New implemented items in Rapid Prototyping technologies section
·Generation and export of STL files,
·Object placing
·Support generation & slicing...
Conclusion
Further practical training on 3D printers is necessary to achieve a comprehensive understanding of 3D printing workflow in medicine. With the new implemented contents, students are able to perform all steps in of the process until the finished 3D printed medical models by themselves and to differentiate which Rapid Prototyping technologies are commonly used for medical applications.
Personal information and conflict of interest
G. Guevara Rojas; Vienna/AT - nothing to disclose M. Ali; Vienna/AT - nothing to disclose G. Schwarzmüller-Erber; Vienna/AT - nothing to disclose C. Schneckenleitner; Vienna/AT - nothing to disclose G. Unterhumer; Vienna, AUSTRIA/AT - nothing to disclose
References
(1) Hanasono MM, Goel N, DeMonte F. Calvarial reconstruction with polyetheretherketone implants. Ann Plast Surg. 2009; 62:653-5.
(2) Guevara-Rojas G, Figl M, Schicho K, Seemann R, Traxler H, Vacariu A, Carbon C, Ewers R, Watzinger F. Patient-specific polyetheretherketone facial implants in a computer-aided planning workflow. Journal of Oral and Maxillofacial Surgery 2014; 72:1801.
(3) Guevara Rojas G, Unterhumer G, Schwarzmüller-Erber G, Schicho K. Computer Assisted Surgery and Rapid Prototyping for Radiographers. Implementation of a new lecture; ECR 2018 / C-1119 Vienna/AT
https://posterng.netkey.at/esr/viewing/index.php?module=viewing_poster&doi=10.1594/ecr2018/C-1119