Keywords:
Performed at one institution, Observational, Prospective, Prostheses, Neoplasia, Artifacts, Diagnostic procedure, MR, Breast
Authors:
M. P. F. Ananias1, A. M. Munhoz1, L. F. Chala1, G. G. N. Mello1, A. G. T. D. S. FILHO1, H. F. B. D. CASTRO2, A. D. A. M. Filho1, T. C. D. M. Tucunduva1, R. Gemperli1; 1São Paulo/BR, 2SAO PAULO/BR
DOI:
10.26044/ecr2020/C-14673
Results
None of the patients reported local heat or discomfort during the MRI examination. There were no signs of intra or extracapsular ruptures, contractures or relevant fluid collections.
The implants' volumes ranged from 375 to 540 cm³ (average, 415 cm³) and 185 to 295 cm³ (average, 215 cm³) on the reconstructed and contralateral breast respectively.
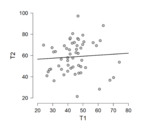
All implants showed an RFID-M related artifact with a mean estimated volume in T1 of 45.1 cm³ and in T2 of 55.6 cm³ as shown in Table 1. The mean ratio between estimated artifact volume and implant volume was 14.75% (95% CI, 13.14-16.36) in T1 and 18.25% (95% CI, 15.87-20.63) in T2. The artifact volume in T1 is statistically significantly smaller than in T2 (P <0.001) (Fig. 5). The Pearson’s correlation coefficient (r = 0.075) indicates that there is no linear relationship between T1 and T2 EVAs as shown in Table 2.
MRI results were divided by surgical indication groups: group A (41/56) included mastectomies, therapeutic or risk-reducing adenomastectomies, and quadrantectomies; group B (15/56) included only breast symmetrizations.
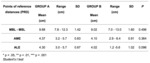
The average artifact volume in group A was 46.34 cm³ (95% CI, 43.01-49.67) and in group B was 42.04 cm³ (95% CI, 36.93-47.15) in the T1 sequence. The average of artifact volume in group A was 57.39 cm³ (95% CI, 52.25-62.53) and in group B was 48.68 cm³ (95% CI, 37.80-59.56) in the T2 sequence. There were no statistically significant differences in artifact volume between groups A and B as shown in Table 3.
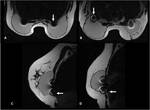
All cases showed thoracic wall involvement and only two (2/56; 3.5%) extended to the breast parenchyma due to the small volume (180 mL) and the minimum lower displacement of the implant. There were 5/56 (8.9%) cases of implant rotation (3/5 in group A and 2/5 in group B). In all cases, the angle of rotation was less than 45° (1 medial, 2 lateral and 2 inferior) (Fig. 6).
A total of 4/5 displacements occurred in implants with a volume below 250 mL and 1/5 in implants above 350 mL. The implants with a volume of fewer than 250 ml presented a statistically significant association with displacement/rotation (Table 4 and Table 5).
The distance from the reference points was measured in the T2 sequences and is summarized in Table 6. The paired analysis of reference point distances and rotation/displacement showed no significant differences between groups A and B.