Keywords:
Interventional Radiology, Interventional non-vascular, CT, Biopsy, Cancer, Retrospective, Observational, Performed at one institution
Authors:
E. RONCONI1, M. A. Tipaldi2, T. Polidori1, F. Laurino3, A. Pisano1, A. Zolovkins2, G. Orgera2, A. Laghi2, M. Rossi2; 1roma/IT, 2Rome/IT, 3EBOLI/IT
DOI:
10.26044/ecr2020/C-15370
Methods and materials
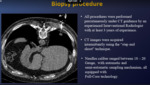
Data Collection: Prior to the biopsy, all patient had undergone a diagnostic CT chest scan. Based on these images, a retrospective analysis was performed. Lesion size, localization, morphology and distance from the pleural surface were recorded. The latter was evaluated by an expert interventional radiologist considering the optimal needle trajectory to avoid major vessels, interlobular fissures, visible bronchi and overlapping of bone structures.
SUV (Standardized Uptake Value) were taken from the PET report and a maximum value equal or less then 2.5 was considered the cut-off to mark a nodule as negative. A few cases not reporting the SUV were re-evaluated with the help of a nuclear medicine specialist in order to obtain a numerical value.
Data about each procedure have been extracted from the header DICOM retrieved from our hospital PACS: duration of total session, procedural time for biopsy and Dose-Length-Product (DLP) for each patient were collected.Histopatological reports were examined and results classified in 3 categories: positive for a specific malignant disease, positive for a specific benign disease and not adequate sample. The latter were deemed those which resulted in necrosis, clots, normal parenchima tissue, or those with not enough material for diagnosis.Complications were investigated with peri-procedural CT, 3 hours post-procedural X-ray control or other radiological exams until patient discharge. Complications were classified as minor or major according to the Society of Interventional Radiology (SIR) Guidelines [36]. Minor complications consisted of pneumothorax not requiring intervention, limited parenchymal hemorrage and transient hemoptysis. Major complications consisted of pneumothorax or iatrogenic bleeding requiring chest tube placement or embolization.
Statistical Analysis: All calculations were made using IBM SPSS Statistics for Windows, Version 14.1. Continuous variables were reported as mean +- SD, discrete variables as absolute number and relative frequency. Distribution was checked for normality using the Shapiro-Wilk test. Univariate analysis was performed in order to assess wich features correlates with unsuccessful procedures, with a p value cut-off of < 0.1 for statistical significance. When normally distributed, a two-tailed T-test was used; when not normally distributed, the Mann-Whitney test was used. Pearson chi-square was was performed to test for dichotomous variables. A multivariate logistic regression model was constructed choosing as indipendent predictors those features wich resulted significant at the univariate analysis, adjusted for the other factors included in the study. Continuous factors included in the model were dichotomized around an optimal cut-off for sensitivity and specificity, by applying Youden’s index on ROC curves. Specifically, we used a cut-off of 18 mm for maximum lesion diameter, and 20 mm for distance from the pleural surface. A Bootstrap internal validation setted at 500 ripetition was used to correct for overfitting. Prediction accuracy of our model was estimated using the C-index, and goodness of fit via Hosmer-Lemeshow test. Results are reported in odds ratios (OR) with a 95% CI, and a point-based score model for the risk of unsuccessfull procedures was developed using variables resulting statistically significant at p < 0.05. A normogram was then constructed to help allocating points to each patients, and predicted probability of unsuccess is express as percentages.