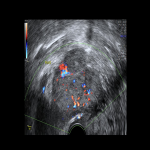
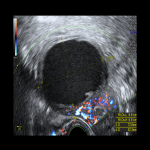
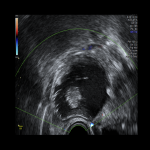
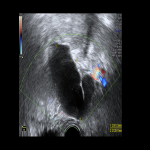
Ovarian cancer is low in prevalence but potentially fatal.
O-RADS provides a classification system previously unavailable using ultrasound, based on a common lexicon, which allows categorizing the risk of malignancy through guidelines.
GENERAL INFORMATION
- Based on retrospective analysis of IOTA phase 1-3 data (the largest multicenter prospective study);
- US features of adnexal lesions placed in prespecified risk categories based on IOTA data;
- Clinical management scheme based on expert opinion of gynecologysts, gynecologic oncologists, and radiologists;
- Based on average risk, asymptomatic patient, without increased risk factors for ovarian cancer (it increases sensitivity, not specificity);
- It is based on more conservative treatment for apparently benign lesions and referral to an oncology gynecologist when the lesion is suspicious;
KEY DESCRIPTORS
- CLINICAL HISTORY: Menopausal status should be included in clinical information.
- LOCATION:
Situs: right, left, other;
Relative to ovary: intraovarian, adnexal (if ovarian tissue is not seen), extraovarian or separate from the ovary;
- MAJOR CATEGORIES
A) Physiologic: need no additional descriptors if criteria are met.
- Follicle
- Corpus Luteum
B) Classic benign lesion:
- Hemorrhagic Cyst
- Dermoid Cyst
- Endometrioma
- Paraovarian Cyst
- Peritoneal Inclusion Cyst
- Hydrosalpinx
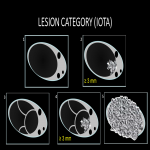
C) Lesion (IOTA Classification):
- Unilocular cyst without a solid component; Incomplete septa, an irregular wall with focal thickening <3 mm in height or internal echoes may be present;
- Unilocular cyst with a solid component (> 3 mm in height);
- Multilocular cyst without a solid component; May include an irregular focal thickening <3 mm in height or internal echoes
- Multilocular cyst with a solid component (>3 mm in height);
- Solid (> 80%);
D) General and extra-ovarian findings:
- Fluid descriptors;
- Peritoneal thickening, nodules;
- Adenopathy;
DESCRIPTORS:
- Size: Maximum diameter is required in any plane;
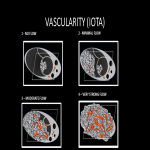
- Vasculary: Color score 1-4 (IOTA classification)
- Color score 1 = No flow;
- Color score 2 = Minimal flow;
- Color score 3 = Moderate flow;
- Color score 4 = Very strong flow;
- Cystic Lesion:
- Inner margin or internal walls (smooth, irregular, papilar projection (<3 mm) or nodule)
- Internal content (solid component if > 3 mm, cystic component like septations or fluid content)
- Solid Lesion:
- Internal content (hypoechoic, isoechoic, hyperechoic, acoustic shadowing, calcifications)
- External contour (smooth, irregular)
In general, the impression should include a brief summary of each finding with the corresponding assessment category and management recommendation and should be listed from most to least concerning.
The assessment category may be provided as the numeric value (0-5) with associated terminology or using terminology alone. The numeric value may be used alone as long as a legend is included within the report.
O-RADS US
O-RADS 0 - INCOMPLETE EVALUATION
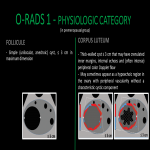
O-RADS 1 - PHYSIOLOGIC CATEGORY (in premenopausal group)
FOLLICULE
- Simple (unilocular, anechoic) cyst, ≤ 3cm in maximum dimension
CORPUS LUTEUM
- Thick-walled cyst ≤ 3 cm that may have crenulated inner margins, internal echoes and (often intense) peripheral color Doppler flow
- May sometimes appear as a hypoechoic region in the ovary with peripheral vascularity without a characteristic cystic component
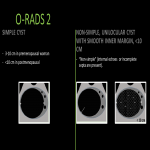
O-RADS 2
SIMPLE CYST
- 3-10 cm in premenopausal woman
- <10 cm in postmenopausal woman
NON-SIMPLE, UNILOCULAR CYST WITH SMOOTH INNER MARGIN, <10 CM
- “Non-simple” (internal echoes or incomplete septa are present).
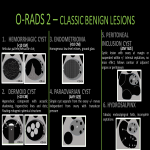
CLASSIC BENIGN LESIONS
- HEMORRHAGIC CYST (<10 CM) - Reticular pattern/Retractile clot;
- DERMOID CYST (<10 CM) - Hyperechoic component with acoustic shadowing, hyperechoic lines and dots; Floating echogenic spherical structures
- ENDOMETRIOMA (<10 CM)- Homogenous low-level echoes, ground glass
- PARAOVARIAN CYST (ANY SIZE) - Simple cyst separate from the ovary +/- moves independent from ovary with transducer pressure
- PERITONEAL INCLUSION CYST (ANY SIZE) - Cystic lesion with ovary at margin or suspended within +/- internal septations, no mass effect, follows contour of adjacent organs or peritoneum
- HYDROSALPINX - Tubular, endosalpingeal folds, incomplete septations
O-RADS 3
- Unilocular cyst, ≥ 10 cm.
- Typical hemorrhagic cyst, dermoid, endometrioma (≥10 cm)
- Unilocular cyst with irregular inner wall, any size
- Multilocular cyst with smooth inner wall, <10 cm, color score 1-3
- Solid or solid-appearing (>80%) with smooth contour, any size, color score 1
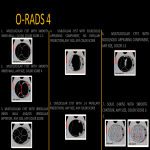
O-RADS 4
- Multilocular cyst with smooth inner wall, ≥10 cm, color score 1-3
- Multilocular cyst with smooth inner wall, any size, color score 4
- Multilocular cyst with irregular inner wall and/or irregular septation, any size, any color score
- Unilocular cyst with solid/solid appearing component, no papillary projections, any size, any color score
- Unilocular cyst with 1-3 papillary projections, any size, any color score
- Multilocular cyst with solid/solid appearing component, any size, color 1-2
- Solid (>80%) with smooth contour, any size, color score 2-3
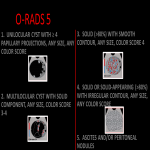
O-RADS 5
- Unilocular cyst with ≥4 papillary projections, any size, any color score
- Multilocular cyst with solid component, any size, color score 3-4
- Solid (>80%) with smooth contour, any size, color score 4
- Solid or solid-appearing (>80%) with irregular contour, any size, any color score
- Ascites and/or peritoneal nodules
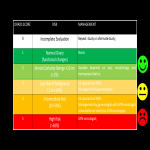
CLINICAL MANAGEMENT SCHEME
0 - Incomplete Evaluation - Repeat study or alternate study;
1 - Normal Ovary (functional changes) - None;
2 - Almost Certainly Benign <10 cm (<1% risk of malignancy) - Variable depends on size, morphology and menopausal status;
3 - Low Risk of Malignancy (1 to <10% risk of malignancy) - US specialist or MRI; Management by gynecologist;
4 - Intermediate Risk (10-50% risk of malignancy) - US specialist of MRI; Management by gynecologist with GYN-oncologist consultation or solely by GYN-oncologyst;
5 - High Risk (>50% risk of malignancy) - GYN-oncologist;
Test your ORADS!
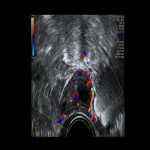
CASE 1 (Premenopausal)
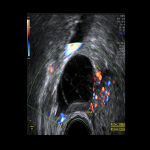
CASE 2 (Premenopausal)
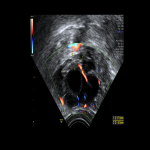
CASE 3 (Postmenopausal)
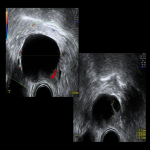
CASE 4 (Postmenopausal)
CASE 5 (Postmenopausal)
CASE 6 (Premenopausal)
CASE 7 (Premenopausal)
CASE 8 (Premenopausal)
CASE 9 (Premenopausal)
CASE 10 (Premenopausal)
CASE 11 (Postmenopausal)