This review will demonstrate the imaging manifestations of nodal and extranodal Non-Hodgkin lymphoma in the ER setting at the time of acute presentation with a systemic approach.
In general, lymphomas demonstrate similar imaging features independent of their location. Lesions are typically homogenous and hypoechoic on ultrasound. CT frequently demonstrates hypodense lesions with homogenous contrast enhancement. Rarely, lesions may demonstrate heterogeneous enhancement with necrosis. On MRI, the lesions are usually iso/ hypointense on T1-weighted imaging (T1WI), hyperintense on T2-weighted images (T2WI) with a similar enhancement pattern to that seen on CT. Lesions demonstrate restricted diffusion on diffusion-weighted images (DWI) images, which reflects the high cellularity of lymphomas. Lymphomas are typically hypermetabolic on 18F-FDG PET/CT, which is the imaging modality of choice for staging and assessing treatment response. Bony destruction is uncommon in lymphomatous masses, and they routinely insinuate between adjacent anatomical structures. They encase and displace the adjacent vessels and luminal structures rather than invasion, but they may rarely cause obstruction by external compression.
Nervous system lymphoma
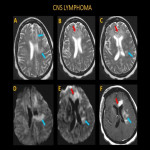
Central nervous system (CNS) lymphoma patients may present to ER with headache, neural deficits, seizure, and altered mental status. Primary CNS lymphoma typically manifests as a CT hyperdense, T1 hypointense, T2 iso-hypointense supratentorial mass with homogeneous enhancement and restricted diffusion. In comparison with glioblastoma multiforme, primary CNS lymphoma less commonly demonstrates central necrosis and hemorrhage, except immunocompromised patients.
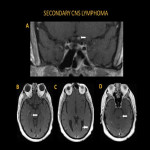
On the other hand,
secondary CNS lymphoma typically involves the dural and leptomeningeal tissues.
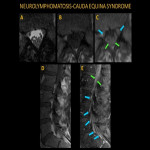
Neurolymphomatosis is characterized by the direct lymphomatous involvement of the cranial or peripheral nerves secondary to systemic lymphoma, which may cause cranial nerve palsies and cauda equina syndrome.
Orbital lymphoma
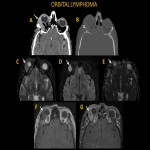
Orbital lymphomas comprise 5-15% of extranodal lymphomas and almost half of the primary malignant tumors of orbits [2]. Patients may present to the ER with a palpable mass, proptosis, diplopia, and blurry vision. Orbital lymphoma manifests as a smooth, homogenously enhancing mass commonly at the superolateral quadrant without bone erosion. The mass may push and mold the adjacent bone and globe.
Head and neck Lymphoma
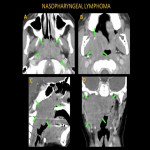
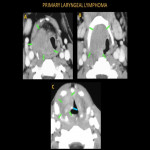
Head and neck Lymphoma may present as cervical lymphadenopathy or as soft tissue mass involving the nasopharynx, oropharynx, or larynx. Lymphoma can cause stridor due to compromised airflow at the supraglottis, glottis, or trachea level. This can be secondary to direct involvement of the Waldeyer's ring, larynx, and trachea or by external compression of the enlarged lymph nodes around the airway.
Thoracic Lymphoma
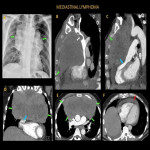
Mediastinal lymphoma is a common anterior mediastinal lesion that may manifest with rapidly progressing chest pain, dyspnea, or cough.
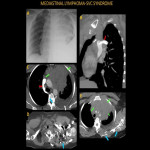
Superior vena cava syndrome (SVCS) is a well-known complication of mediastinal lymphoma secondary to extrinsic vascular compression in the superior mediastinum. Patients with SCVS present with face, neck, and upper extremity swelling, flushing, headache, and neurological symptoms. CT demonstrates large mediastinal soft tissue mass encasing vascular structures, especially SVC causing obliteration. CT is the primary imaging modality to assess the site and severity of the obstruction, thrombosis, and collateralization.
Gastrointestinal lymphoma
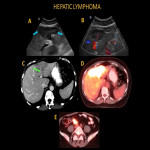
Hepatic lymphoma patients may present to ER with acute right upper quadrant pain, fever, nausea, and vomiting. Hepatic lymphoma may manifest as a focal liver mass or masses, diffuse infiltrating disease, or an ill-defined mass in the portal hilum. The lesions are usually seen as hypoechoic on US, which may have central hyperechoic components (target sign).
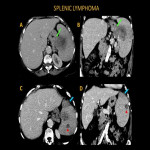
Lymphoma is the most common hematologic malignancy that affects the spleen. Thirty percent of lymphoma patients have spleen involvement at the presentation. ER presentation may include left upper quadrant pain, fever, and a palpable mass. Splenomegaly is the most common imaging finding. Lymphomatous deposits may appear as discrete hypoechoic lesions on US and hypodense masses on CT. Invasion of surrounding structures, including the stomach and pancreas, may be seen.
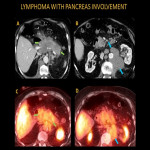
The pancreas may be involved in diffuse non-Hodgkin’s lymphoma and occasionally may cause acute pancreatitis, which may be the initial presentation.
The most common extranodal site of lymphoma is the gastrointestinal (GI) tract, and the stomach is the most frequently affected location in GI tract, followed by the small bowel. GI lymphomas may complicate with gastrointestinal bleeding, perforation, and rarely obstruction.
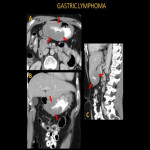
Gastric lymphoma manifests as marked gastric wall thickening. Gastric lymphomas are generally indolent without acute symptoms but may present to the ER with abdominal pain, GI bleed, or rarely obstruction.
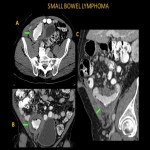
Small bowel lymphomas (SBL) usually occur in the terminal ileum (60-65%), which has rich lymphoid tissue. SBL on imaging demonstrates circumferential bowel wall thickening with extension into the mesentery and regional lymph nodes. Aneurysmal dilatation without obstruction is a characteristic appearance due to the destruction of the myenteric nerve plexus and may help differentiate lymphoma from adenocarcinoma.
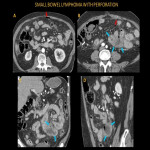
The small bowel perforation can occur in 9% of SBL cases, more commonly with aggressive B-cell and T-cell lymphomas [3]. Although it is more often seen after chemotherapy initiation, patients can present with perforation as an initial presentation.
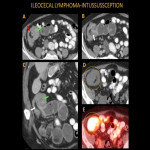
Obstruction is rare with SBL due to the absence of desmoplastic reaction, but it can occur with very large lesions or polypoid lesions causing intussusception.
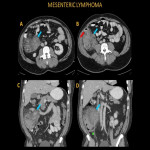
Mesenteric lymphoma is the most common malignant neoplasm of the mesentery. Approximately 30-50% of patients with non-Hodgkin lymphoma have the mesenteric nodal disease. Mesenteric lymphoma occasionally invades the adjacent organ serosa, which results in ER presentations with abdominal pain. The CT appearance of mesenteric lymphoma includes mildly enhancing homogenous bulky mesenteric lymphadenopathy, ill-defined infiltration of the mesenteric fat, and/or large lobulated heterogeneous mass with hypodense areas of necrosis.
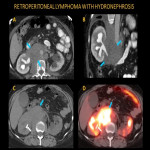
Rarely, lymphoma can cause hydronephrosis and post obstructive acute kidney failure with external obstruction of the ureters.
Genitourinary Lymphoma
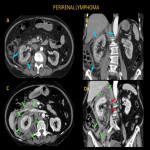
Patients with renal lymphoma may present to ER with flank pain and hematuria. CT images may demonstrate multiple hypodense renal masses, single mass, or diffuse renal infiltration. Less commonly, the perirenal subtype of renal lymphoma may appear as perirenal soft tissue stranding, homogenous soft tissue mass, or plaques and nodules in perirenal space.
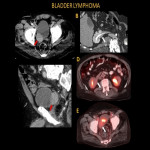
Primary lymphoma of the bladder is rare due to a lack of lymphoid tissue in the bladder. The patients may present to ER mimicking cystitis with hematuria, dysuria, increased urinary frequency, and suprapubic pain. On imaging, bladder lymphoma has a variable appearance ranging from a solitary submucosal mass to diffuse bladder wall thickening and is in the differential for urothelial cell carcinoma. Involvement of the entire bladder wall is uncommon in primary bladder lymphoma, as is hydronephrosis, whereas the opposite is true for transitional cell cancer [4].
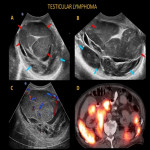
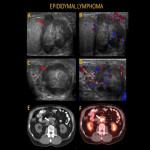
Testicular lymphoma usually occurs in adults older than 60 years of age who may present to ER with rapidly enlarging, firm, non-tender scrotal mass. Testicular lymphoma is the most common bilateral intratesticular tumor. Testicular lymphoma may appear as large hypoechoic infiltrative, focal single, or multiple hypoechoic lesions. Secondary lymphomatous involvement of the epididymis in patients with testicular lymphoma is more common than primary epididymal lymphomas.
Epididymal lymphoma appears as heterogeneous enlargement with increased blood follow on color Doppler. Imaging findings can mimic epididymitis; hence clinical findings like lack of tenderness might be helpful for diagnosis.