Trauma is the leading cause of death in patients under 45 years and the third leading cause of death. Up to 1% of all trauma injuries have a vascular component, involving mainly the extremities.
CT angiography (CTA) of the extremities is a rapid, cost-effective, and noninvasive technique that has widely replaced digital subtraction angiography DSA. It allows rapid characterization of traumatic arterial lesions. Meta-analysis studies have shown very high sensitivity and specificity of 96,2% and 99,2%, respectively, for detecting clinically significant arterial injury.
Other techniques such as color Doppler ultrasound and MR angiography allow the evaluation of suspected vascular injuries, but they have a substantial limitation that is, both require a considerable amount of time. Also, color Doppler sonography is highly dependent on operator skill, and MR angiography is more susceptible to motion artifacts than CT angiography, so they are not practical to perform in the setting of trauma.
CLINICAL SIGNS
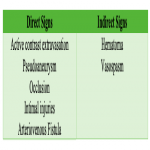
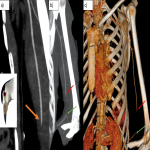
Clinical signs of vascular injury can be categorized in (Fig 1):
- Hard signs: loss of pulses, enlarging hematoma, thrill or bruit, and evidence of limb ischemia.
- Soft signs: asymmetric pulses, nonexpanding hematoma, cool limb, or color change.
Hard signs are associated with a significant vascular injury in almost 100% and require surgical exploration. However, the majority of patients with trauma of the extremities present with soft signs of vascular injury. The prevalence of arterial injury is lower when only soft clinical signs are present.
Patients with hard signs could potentially proceed directly to surgical exploration. However, it is preferable to perform CT in all patients if they are hemodynamically stable because it decreases diagnostic ambiguity, the number of unnecessary catheter-based procedures and provides valuable information to the vascular surgeon or interventionalist.
CT IMAGING TECHNIQUE
- Scanning parameters typically include 120 kVp, 200-300 mAs, a detector thickness of 0.6 mm, a section thickness of 0.75 mm, a reconstruction interval of 0.5 mm.
- Between 100 and 120 mL of contrast material is injected at a rate of 4 to 5 mL/second followed by a saline flush (in cases of upper-extremity trauma, intravenous contrast material should be injected in the contralateral arm).
- Contrast bolus tracking and a trigger threshold of 100 HU.
- Remove metal objects before scanning if possible.
- Positioning the area of interest as close as possible to the isocenter of the CT:
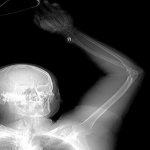
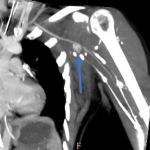
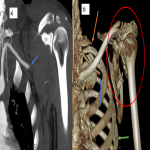
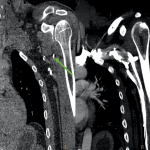
- In cases of upper extremity trauma, the patient should raise the extremities above the head if possible to limit the body's streak artifact (Fig 2).
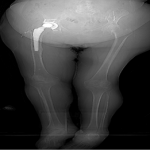
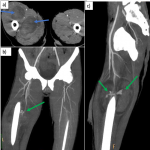
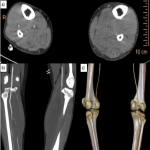
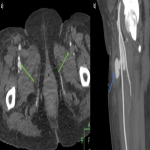
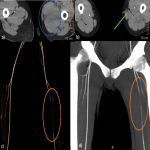
- In lower extremity trauma cases, both lower extremities should be imaged in synchrony in a supine position (Fig 3).
- The presence of the contralateral extremity can be a useful reference.
- Radiation exposure should be minimized by limiting the anatomical coverage to the region of interest when there is not clinically suspected injury in other anatomical regions.
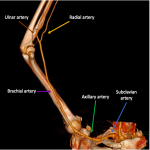
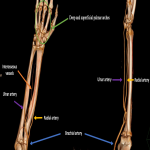
ANATOMY OF THE UPPER EXTREMITY (Fig 4 and 5)
- The arterial supply to the upper limb begins as the subclavian artery. On the right, the subclavian artery arises from the brachiocephalic trunk, and on the left, it arises directly from the aortic arch.
- The subclavian artery travels laterally towards the axilla and extends laterally to the first rib's lateral border, where it enters the axilla and is renamed the axillary artery.
- The axillary artery lies deep to the pectoralis minor and extends from the lateral border of the first rib to the lower border of the teres major muscle.
- The brachial artery is a continuation of the axillary artery and extends from the inferior border of the teres major tendon to 1 cm inferior to the elbow joint line.
- The brachial artery at the cubital fossa typically bifurcates into three major branches: the arteria profunda brachii (first branch), the radial artery, and the ulnar artery.
- The ulnar artery gives rise to the interosseous vessels.
ANATOMY OF THE LOWER EXTREMITY
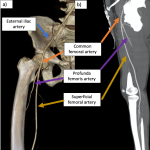
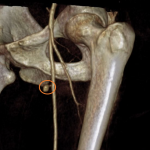
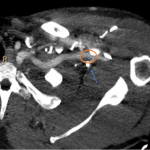
- The common femoral artery (Fig 6) is a continuation of the external iliac artery after passing the inguinal ligament.
- After originating the profunda femoris artery (Fig 6), it is also commonly known as the superficial femoral artery.
- The superficial femoral artery (Fig 6) continues down within the thigh's anterior compartment until it enters the posterior compartment through the abductors canal, proximal to the knee, where is now known as the popliteal artery.
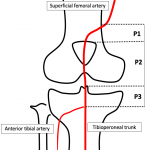
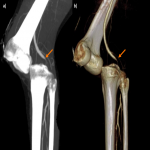
- The popliteal artery is usually divided into three segments (Fig 7):
- P1: from the abductors canal to the proximal edge of the patella.
- P2: from the proximal edge of the patella to femorotibial joint space.
- P3: from femorotibial joint space to the origin of the tibial artery.
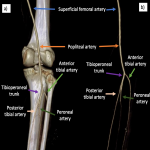
- Below the knee, the popliteal artery bifurcates into the anterior tibial artery and the tibioperoneal trunk (Fig 8), which ends bifurcating into the posterior tibial artery and peroneal artery.
- At the ankle, the anterior tibial artery becomes the dorsalis pedis, which supplies the foot's dorsum, and the posterior tibial artery gives rise to the plantar arch.
CT SIGNS OF ARTERIAL INJURIES
The CT signs of arterial injuries are (Fig 9):
- Direct signs: active contrast extravasation, pseudoaneurysm, occlusion, intimal injuries, and arteriovenous fistula.
- Indirect signs: hematoma and vasospasm.
Active contrast extravasation: usually manifests as an irregular blush of extraluminal contrast material into adjacent soft tissues (Fig 10) and does not wash out on venous or more delayed phases. It indicates ongoing hemorrhage.
Pseudoaneurysm: a well-circumscribed round extravascular contrast-filled sac connected to a vessel through a neck at a site of focal arterial wall discontinuity (Fig 11). It shows the same behavior as arteries with washout on venous and delayed phases (Fig 12).
Occlusion: It is seen as an abrupt interruption of the contrast-enhanced blood with or without distal reconstitution (Fig 13 and 14). It may represent in situ thrombosis of a vessel at the site of arterial wall injury, transection, or intimal flap. It is difficult to distinguish between these entities, but sometimes some signs can help, like the "beak sign”. The “beak sign” is defined as wedge-shaped hypodensity at the ends of the occluded segment (Fig 15), indicating thrombosis. In cases of transection (Fig 16), malalignment in proximal and distal segments on CTA can be seen.
Intimal injuries: damage of the innermost layer of the artery can result in flaps, disruptions, or subintimal/intramural hematomas (Fig 17). Dissection can appear as a linear or curvilinear nonenhancing filling defect representing intimal flap or an intraluminal complete filling defect.
Arteriovenous fistula: the communication between the artery and vein can be seen on CTA as asymmetric early venous enhancement on the arterial phase (Fig 18).
Hematoma is a focal collection of blood without contrast opacification outside the vessel lumen (Fig 10 and 14).
Vasospasm: It can be shown as a diffuse narrowing artery or gradual tapering vessel before losing opacification (Fig 19).
PITFALLS OF COMPUTED TOMOGRAPHY ANGIOGRAPHY
- Poor arterial lumen opacification can be caused by the discrepancy in timing between the angiographic boluses' transit and the incorrect timing of the image acquisition.
- Motion artifacts due to patient movement during scanning can degrade the quality of CT angiograms.
- Remember that in cases of upper-extremity trauma, intravenous contrast material should be injected into the contralateral arm. The streak artifacts due to contrast material in the adjacent venous can difficult the correct visualization of the arteries (Fig 20).
- Beam-hardening artifacts due to metallic implants and foreign bodies can lead to an uninterpretable angiogram (Fig 17). Streak artifacts can potentially create pseudo-lesions or hide subtle lesions.