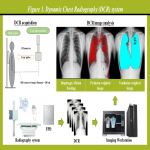
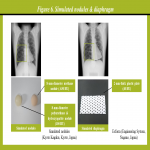
We used our original rotation phantom (a 20-cm-diameter acrylic disc) and a commercially available lung phantom (Lungman phantom; Kyoto Kagaku, Kyoto, Japan) (Figure 5) with simulated nodules and diaphragm (Figure 6) to perform the following three experiments with standard acquisition parameters used in clinical settings and all the pulse widths available with the DCR system: 1) quantitative evaluation of blurring and ghost artifact, 2) qualitative evaluation of nodule visibility, and 3) quantitative evaluation of diaphragmatic movement. The system specifications and acquisition parameters used in this study are summarized in Table 1.
Quantitative evaluation of blurring and ghost artifact
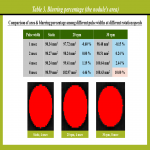
The rotation phantom where a simulated nodule, a 10-mm-diameter lead disc of CT value of 15000 HU, was attached was placed on the lung phantom (Figure 6) and rotated at speeds of 20 and 30 rotations per minutes (rpm) in the counter-clockwise direction (Figure 7, Figure 8). Frontal DCR at pulse widths of 1, 2, 4, and 8 msec as well as static radiography of the phantoms was acquired. On both DCR and static radiography, using an image analysis software (ImageJ; National Institutes of Health, Version 1.53e, Bethesda, MD), profile curves were drawn for the nodule located at the top or zero degree to measure full width at half maximum (FWHM) of its diameter (Figure 9); and a region of interest (ROI) was placed including the nodule located at the same location to determine the threshold of its signal value and to measure its area of signal value greater than the threshold (Figure 9). Blurring percentages based on both the FWHM and area on DCR (a) and static radiography (b) were calculated to quantitatively evaluate blurring at different pulse widths using the following equation: (a-b)/b x 100%.
Using the software, a circular ROI of the maximum area was placed within the nodule located at the zero degree as a reference to measure the mean signal values in both the nodule’s ghost artifact (a) at the following 10 frames (the first to tenth frame following the reference) and background (b) at the 20th frame on DCR (Figure 10); and ghost artifact percentages at the first to tenth frame were calculated to quantitatively evaluate ghost artifact at different pulse widths using the following equation: (b-a)/b x 100%.
Qualitative evaluation of nodule visibility
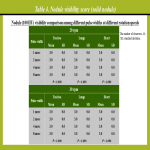
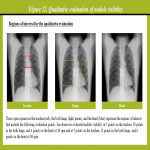
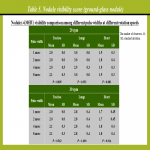
The rotation phantom where a simulated solid nodule made of polyurethane and hydroxyapatite (the diameter, 8 mm; CT value, 100 HU) and a simulated ground-glass nodule made of urethane (the diameter, 8 mm; CT value, -630 HU) were attached was placed on the lung phantom (Figure 6) and rotated at speeds of 20 and 30 rpm in the clockwise direction (Figure 11). Frontal DCR of the phantoms was acquired at pulse widths of 1, 2, 4, and 8 msec. Independent ten observers qualitatively evaluated visibility of these nodules in both the lungs (18 different evaluation points at 20 rpm, 32 points at 30 rpm) and on the trachea (3 different evaluation points at 20 rpm, 5 points at 30 rpm) and the heart (4 different evaluation points at 20 rpm, 6 points at 30 rpm) on DCR (Figure 12) using the following scoring system: 1, always invisible; 2, sometimes visible; and 3, always visible. The nodule visibility scores by the ten observers were averaged.
Quantitative evaluation of diaphragmatic movement
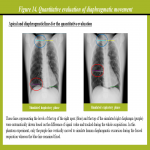
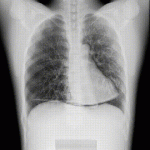
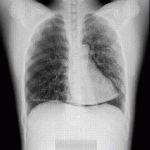
The simulated diaphragm, a 2-mm-thick plastic plate of 40 HU, was horizontally placed on the lung phantom on the right side (Figure 6) and vertically moved at a constant speed to simulate human diaphragmatic excursion during the forced respiration (Figure 13, Figure 14). Specifically, two medical syringes filled with air were connected via an extension tube, the plate was attached to a piston end of one syringe, and that of the other syringe was manually pushed and pulled back with the same stroke volume. Frontal DCR of the phantom was acquired during a single cycle at pulse widths of 1, 2, 4, and 8 msec. The maximum diaphragmatic movement from the inspiration level to the expiration level was automatically measured three times using the dedicated workstation and the measurements were averaged.
Statistical analysis
All the continuous variables were expressed as mean ± standard deviation (SD). Statistical analysis was performed using commercially available software (IBM SPSS Statistics, version 27 IBM SPSS, Armonk, NY). The blurring and ghost artifact percentages at 20 and 30 rpm, nodule visibility scores at 20 and 30 rpm, and averaged maximum diaphragmatic movements were compared among the different pulse widths. The nodule visibility scores in/on each anatomy were compared using Kruskal-Wallis test. P-values less than 0.05 were considered significant.