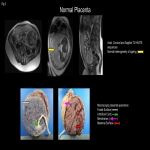
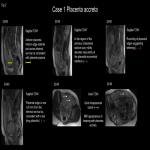
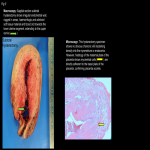
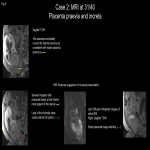
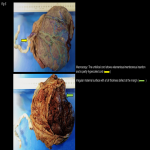
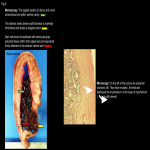
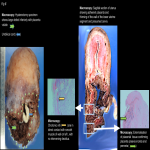
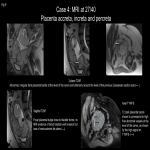
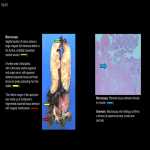
Normal placental attachment is to the decidua basalis layer. Placental adhesive disease occurs when there is abnormal attachment to the myometrium. Abnormal placentation is a spectrum disorder ranging from abnormally adherent to deeply invasive placental tissue:
- Placenta accreta/ Placenta accreta vera (75-80%): attachment of placenta to myometrium without muscular invasion.
- Placenta increta (15%): Chorionic villi invade the myometrium.
- Placenta percreta (5%): Penetration of chorionic villi through the serosa which may invade the bladder, rectum, and parametrium.[2]
Absence of histopathological confirmation causes diagnostic difficulties and partly explains why there is a wide variation in the reported prevalence of placenta accreta, ranging between 1 in 300 and 1 in 2000 pregnancies[3]. This highlights the need for a standardised approach to imaging, clinical and histopathological descriptions.
Risk factors for developing placental adhesive disease:
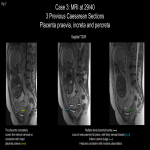
- History of accreta in a previous pregnancy
- Placenta praevia
- Previous caesarean delivery
- Previous uterine surgery
- Advanced maternal age (35 years or more)
- Assisted reproductive technology (ART), in particular in vitro fertilisation.[4]
The incidence of placental adhesive disease (PAD) is increasing and will continue to do so as a result of rising rates of Caesarean deliveries, increased maternal age and use of assisted reproductive technology (ART). It is associated with a high maternal and neonatal morbidity and mortality risk, which is usually related to massive haemorrhage.[5] The highest rates of complication for both mother and newborn are observed when these conditions are only diagnosed at delivery.[6]
Antenatal diagnosis of placenta accreta spectrum is crucial in planning its management and reduces maternal peripartum haemorrhage and morbidity.[7]
Although ultrasound is the initial imaging modality of choice for placental assessment, and the diagnostic value of MRI and ultrasound imaging in detecting placenta accreta spectrum is similar when performed by experts; no ultrasound sign or combination of signs have so far been found to be specific in assessing depth of placenta accreta spectrum in order to distinguish between adherent and invasive placentation.
Determining the depth and lateral extension of placental invasion is helpful for planning the individual care of women diagnosed with placenta accreta spectrum. Therefore, MRI is of added diagnostic value when this further characterisation is required and may be used to complement ultrasound imaging, especially with posterior placentation and/or in women with ultrasound signs suggesting parametrial invasion and its use has significantly increased in recent years.[8]
The diagnostic sensitivity of deciphering between accreta/ increta vs percreta can be challenging, but in clinical practice if MRI is able to establish the severity of PAD, it can be invaluable in aiding Obstetricians plan for delivery and subsequently reduce morbidity and mortality.
Methods and Materials
Retrospective and prospective analysis of placental 1.5T MRI with the corresponding gross pathology and histopathology imaging of 5 individual anonymised patients.
In our institution, if there is a clinical suspicion of invasive placentation, we aim to perform placental MRI at approximately 28 weeks gestation. The recommended time frame to perform placental MRI is between 24-30 weeks gestation as the normal placenta exhibits homogeneous intermediate signal and is usually clearly distinct from the more heterogeneous myometrium. Before week 24, the placenta is immature and therefore diagnosis can be difficult and inaccurate on MRI. After 30 weeks, the internal placental signal becomes more heterogeneous as the placenta matures.[9] However if patients are symptomatic, imaging can be performed outside of this timeframe and repeated if necessary as gestation progresses.
MRI protocol for suspected placental adhesive disease:
MRI Sequence and Main Radiographic Features Evaluated
Multi-planar T2 SSFSE -
- Anatomical assessment including location of placenta in relation to cervix.
- Placental homogeneity; placental:myometrial interface
- Invasive bands
- Assess for invasive placentation outwith the uterus.
T1 GE FS -
DWI; B values 0, 600, 1000 -
- Placental:myometrial interface
- Placental contour
N.B. Diffusion Weighted Images can be helpful in difficult cases to further assess abnormal placentation, however can be significantly degraded due to the degree of foetal movement.