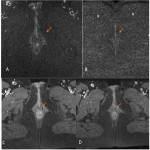
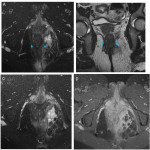
Perianal Fistula consists in an inflammatory condition that creates abnormal connections between the anal canal and the perineal skin.
Anoperineal complications such as fistulae and abscesses are particularly frequent in patients with Crohn’s disease. The prevalence of perianal fistula in these patients ranges between 13% and 38%. It reaches 92% in case of colonic involvement.
1/Radiologic anatomy of the perineal region:
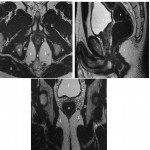
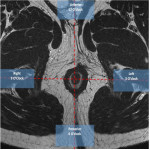
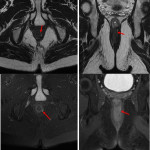
* Perineum anatomy (Fig1):
The perineum is the anatomical region below the pelvic floor. It is divided by an imaginary line passing through the two ischial tuberosities into two spaces:
- The anterior urogenital triangle.
- The posterior anal triangle.
The anal triangle is the posterior half of the perineum with the anal canal located centrally and the ischioanal fossae on either side.
The pelvic floor defines two spaces:
- The supralevator space
- The infralevator space
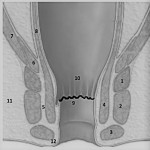
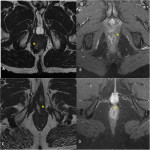
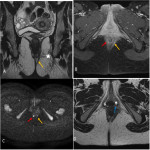
* Anal canal anatomy (Fig 2):
The anal canal represents the terminal portion of the digestive tract. It crosses the posterior perineum with an average length of 3cm. It is formed by two nested muscular cylinders:
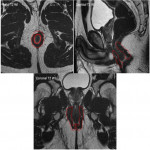
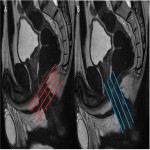
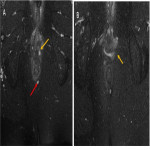
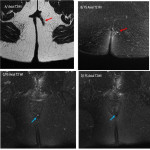
- The external sphincter (Fig 3):
External muscular layer made of striated muscle which is in continuity with the striated muscle of the pelvic floor. It contracts voluntary and is responsible for the 15% resting tone of the anal canal
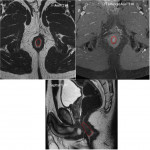
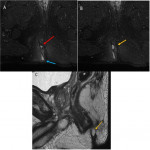
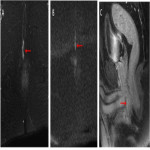
- The internal sphincter (Fig 4):
Internal muscular layer made of smooth muscle, which is in continuity with the smooth muscle of the rectum It contracts involuntary and is responsible for 85% of the resting tone of the anal canal.
* Intersphincteric space: These two sphincters are separated by an intersphincteric space that contains fat and interstitial tissue. It emits extensions towards the skin of the anal margin forming the corrugator cutis ani.
2/ Indications of MRI:
* MRI has a high sensitivity in detecting blind extensions and secondary tracts therefore it guides the therapeutic management to avoid relapsing. It makes an accurate fistula mapping and perineum evaluation.
* MRI is of value to detect sepses outside the anal sphincter and their relationship with the sphincter and levator ani muscles, particularly in complex fistulae. It is fundamental to detect and drain abscesses before introducing biological therapy or immunomodulatory agents to avoid septic complications.
* MRI is a good tool for the follow-up, it monitors the treatment response of the perianal fistula. It provides information about the disease activity and inflammatory changes.
* MRI helps with diagnosis in a symptomatic patient with painful clinical examination.
3/ Parks’ classification:
Parks’ classification is the first classification of perianal fistula. It is a surgical finding based classification that describes the primary fistulous track among the perineal anatomy on coronal projection. There are four groups :
- Intersphincteric Fistula: It is the most frequent type of perianal fistula, the track goes down through the intersphincteritic space to reach the perianal skin.
- Transsphincteric Fistula: The track passes through internal and external sphincters to the ischiorectal fossa.
- Suprasphincteric Fistula: The track moves up in the intersphincteric space, steps over the puborectalis muscle, then descends through the pelvic floor to the ischioanal fossa and the skin.
- Extrasphincteric Fistula: This is the least frequent type of perianal fistula. The point of origin is above the anal canal, in the rectum. The track passes down through the pelvic floor and ischioanal fossa to reach the skin. There is no sphincter involvement.
4/ St James’ University Hospital Classification:
It is a radiological classification that relates Parks’ classification to anatomic MR findings on axial and coronal planes. It is based on main and secondary tracks and abscesses. However, it is not an official surgical reference. It contains fives grades :
- Grade 1: Simple Linear Intersphincteric Fistula
- Grade 2: Intersphincteric Fistula with an Abscess or Secondary Track
- Grade 3: Simple Transsphincteric Fistula.
- Grade 4: Transsphincteric Fistula with an Abscess or Secondary Track in the Ischiorectal or Ischioanal Fossa
- Grade 5: Supralevator and Translevator Disease
5/ MRI protocol:
Patient Preparation :
- The patient is placed in a decubitus position
- The exam is performed with a phased-array surface coil.
- It is possible to use endoanal coils to improve the contrast of the perianal region but they are poorly tolerated in symptomatic patients.
- There is no need for bowel preparation or pre-medication
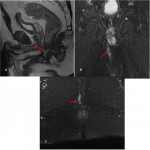
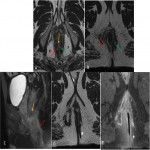
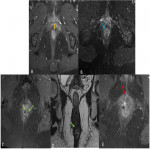
The MRI protocol in our institution includes(Fig 5):
- Sagittal FSE T2 sequence
- Oblique Axial FSE T2 sequence (perpendicular to anal canal axis)
- Oblique Coronal FSE T1 sequence (parallel to anal canal axis)
- Oblique Axial Fat-suppressed FSE T2 sequence
- Oblique Coronal fat-suppressed FSE T2 sequence
- Oblique Axial Diffusion sequence (B0 - B1000)
- Oblique axial fat-suppressed GRE T1 sequence after IV injection of Gadolinium-based material
- Oblique Coronal fat-suppressed GRE T1 sequence after IV injection of Gadolinium-based material
- T2 sequences demonstrate the contrast between the hyperintense signal of fluid within the fistula and the hypointense signal of the muscular canal. Fat suppressed T2 sequences sensitizes this detection
- Gadolinium-enhanced fat-suppressed T1 sequences as well as for Diffusion sequences enable to distinguish between active fistula that enhances avidly and chronic fistulous tract that remains hypointense. It also helps to detect abscesses.