Purpose
In screening mammography achieving good breast positioning is vital to ensuring there is adequate tissue visualization. Work by Taplin et al. showed that when image positioning quality failed to meet positioning criteria, the sensitivity of mammography fell from 84% to 66.3%. [1] However, manually evaluating breast positioning is time consuming and subjective. Recently, Sharma et al. demonstrated substantial variability between evaluation of breast positioning by a group of ten readers (nine radiographers and one radiologist), where levels of agreement on a series of criteria ranged...
Methods and materials
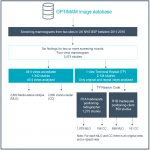
A dataset of four-view mammographic screening studies was retrospectively identified, as per Figure 1 [Fig 1], from the OPTIMAM image database (screening mammograms from two sites in the UK NHSBSP between 2011-2018) among women without findings (“normal”) for two or more screening rounds.[5]
There were 2,134 “technical repeat” (TP) studies identified which included a single, same-day repeated view and reason codes related to inadequate positioning. [6] There were 1,275 images with repeat code R1A, i.e., “Inadequate positioning – Client” and 859 images with repeat code...
Results
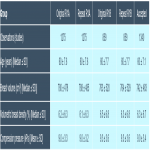
Comparing the population statistics of the women who had TPs and women who had studies in which all images were accepted, there were no significant differences in age, volumetric breast density, breast volume, or compression, as summarized in Figure 2. [Fig 2]
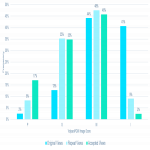
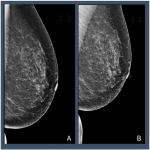
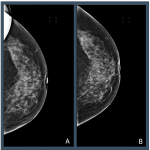
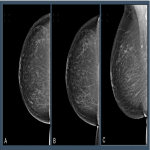
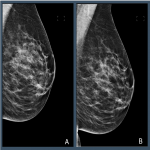
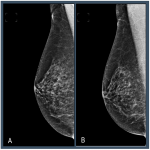
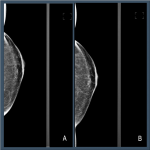
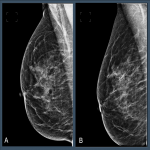
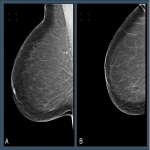
Distributions across the Volpara PGMI categories varied between the original views that were subsequently repeated as a TP (“Original”) and accepted images, with significantly fewer Perfect (2% vs 17%, p<0.001) and more Inadequate (41% vs 2%, p<0.001) scores in the Original versus accepted...
Conclusion
A retrospective study of mammographic screening images from the UK NHSBSP showed automated analysis of breast positioning found significantly more inadequate images in the technical repeats attributed to positioning errors than in a reference group of accepted studies.
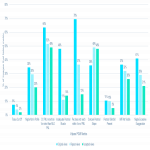
For technical repeat images, automated measurements related to inadequate visualization of the pectoral muscle on MLO views represented the most common positioning deficiencies.
Automated positioning measurement represents a promising means to continuously monitor image quality and radiographer performance in an objective manner.
Personal information and conflict of interest
H-M. Gilroy:
Employee: Volpara Health Limited
M. L. Hill:
Consultant: Volpara Health Limited
A. Chan:
Employee: Volpara Health Limited
M. Halling-Brown:
Grant Recipient: CRUK
R. P. Highnam:
CEO: Volpara Health Limited
References
[1] Taplin SH., et al., Screening Mammography: Clinical Image Quality and the Risk of Interval Breast Cancer. AJR:178, April 2002.
[2] Sharma N., et al., Mammography positioning errors: a multi-centre study. Insights Imaging: 10(Suppl 1); S512, 2019.
[3] Johnston L., et al., C-1029, European Congress of Radiology, 2017, Vienna, Austria.
[4] Wang K., et al., C-0854, European Congress of Radiology, 2016, Vienna, Austria.
[5] Halling-Brown M.D., et al., OPTIMAM Mammography Image Database: A Large-Scale Resource of Mammography Images and Clinical Data. Radiology: Artificial Intelligence, Nov...