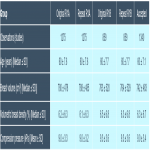
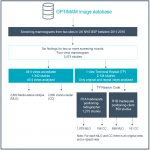
Comparing the population statistics of the women who had TPs and women who had studies in which all images were accepted, there were no significant differences in age, volumetric breast density, breast volume, or compression, as summarized in Figure 2.
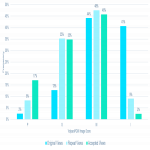
Distributions across the Volpara PGMI categories varied between the original views that were subsequently repeated as a TP (“Original”) and accepted images, with significantly fewer Perfect (2% vs 17%, p<0.001) and more Inadequate (41% vs 2%, p<0.001) scores in the Original versus accepted groups, respectively, as illustrated in Figure 3.
A significant (p<0.001) reduction in Inadequate scores was observed between the Original (41%) versus repeat views (9%) of the TP studies.
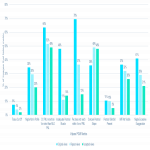
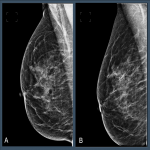
For Original views, measurements related to inadequate visualization of the pectoral muscle on MLO views represented the most common positioning deficiencies. The Original views had over four times more images where the pectoral muscle failed to descend to within 1cm of the PNL line compared to the accepted images (70% vs 15%, p<0.001), and over three times more Original views fail to be assessed as having adequate visualization of the pectoral muscle compared to the accepted images (48% vs 14%, p<0.001), as illustrated in Figure 4.
For CC views, there were significantly more Original images where the nipple was exaggerated from the central midline compared to accepted images (41% vs 21%, p<0.001).
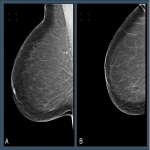
Pectoral shape was one metric where the Original views had a lower number of images that failed compared to the accepted images (36% vs 48%, p<0.001), such as observed in Figure 5.
The inclusion of the component metric related to pectoral shape is based on the American College of Radiology guidelines which state that optimal MLO positioning should include a pectoral muscle with a convex anterior border, [7] however, the UK NHSBSP guidelines specify no explicit condition for the shape of the pectoral muscle. [8]
A review of the Original views scored Perfect by Volpara PGMI showed the majority of these were due to the presence of other body parts obscuring tissue, as seen in Figure 6
, or images were the CC posterior nipple line (PNL) reached to within 1cm of the MLO PNL and passed but the repeat appears to have improved visualisation of posterior tissue, such as is observed in Figure 7.
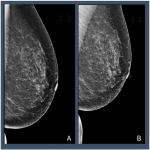
For 1,128 TP studies the Image Score was higher for the repeated view than the Original view, this is 53% of the total TP studies, Figures 8 and 9.
For 850 TP studies the Image Score was the same for the Original and repeated views, this is 40% of the total TP studies. We conjecture that many of these cases, such as the example in Figure 10
, would reflect the difficulty of positioning some women due to patient-related factors.
For 156 TP studies the Image Score was lower for the repeat view than the Original view, this is 7% of the total TP studies. A review of the images, such as in Figures 11 and 12,
indicates the majority of those repeats scored Inadequate are partial or modified views that were likely acquired with the aim to improve visualisation of particular areas of breast tissue. As such, most of these findings likely represent ‘false negatives’ and highlights the limitations of analysis without having a secondary review. However, we find it instructive that the study methodology revealed that cases may exist where the Repeat Reason code may not have been accurately assigned and that this is one source of uncertainty for the interpretation of results.
Limitations
The cases collected were sourced from two screening centres and were predominantly Hologic equipment.
The images were reviewed independently of priors and clinical information, which is important information when deciding to repeat or not repeat an image.
The component metrics used to assess breast positioning did not include a metric related to other body parts creating obscuring artefacts in the image.
Future work
As future work we propose a prospective study where the automated software is used to provide feedback on breast positioning during the screening exam to measure the impact on technical repeats and technical recall rates.
Future work could also include a retrospective analysis of repeated views by a panel of experienced radiographers and radiologists to confirm the need for repeat in the identified technical repeats. Furthermore, for this study, TP cases with R1A and R1B repeat reason codes were grouped for analysis, but a breakdown per category would be of interest to study the potential for different positioning deficiencies and likelihoods for their resolution between the groups.