Keywords:
Artificial Intelligence, Breast, Radiographers, Mammography, Screening, Technology assessment, Education and training, Image verification, Quality assurance
Authors:
H.-M. Gilroy1, M. L. Hill1, A. Chan1, M. Halling-Brown2, R. P. Highnam1; 1Wellington/NZ, 2Guildford/UK
DOI:
10.26044/ecr2021/C-13781
Purpose
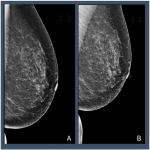
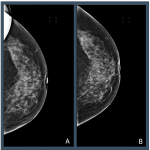
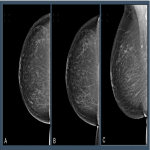
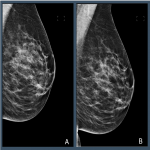
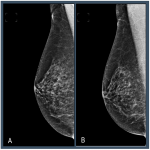
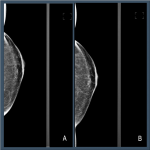
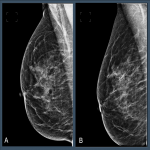
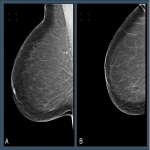
In screening mammography achieving good breast positioning is vital to ensuring there is adequate tissue visualization. Work by Taplin et al. showed that when image positioning quality failed to meet positioning criteria, the sensitivity of mammography fell from 84% to 66.3%. [1] However, manually evaluating breast positioning is time consuming and subjective. Recently, Sharma et al. demonstrated substantial variability between evaluation of breast positioning by a group of ten readers (nine radiographers and one radiologist), where levels of agreement on a series of criteria ranged from k= 0.52 to 0.88 within a centre to k = 0.06 to 0.39 for readers at different centres. [2]
Automated tools have the potential to help improve the efficacy and lower the subjectivity of assessing breast positioning. By providing objective and timely feedback on every image, algorithms could help to:
- ensure analysis is independent of reader’s training and experience by applying the same rules to every image,
- provide timely analysis of positioning while the patient is in the room to aid the Radiographer in deciding if a study is acceptable, and thereby avoid potential technical recall (TC),
- identify trends and provide regular feedback for continuous quality improvement.
Emerging commercial offerings of automated positioning assessment tools require evaluation to provide evidence of measurement accuracy, of adequacy to reflect the desired evaluation scheme in the target setting, and ultimately, that their implementation would improve clinical practice.
Previous work has already reviewed the accuracy of many of the automated mammographic breast positioning metrics discussed in this study. [3,4]
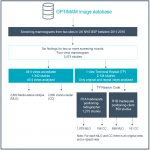
This study aimed to provide first evidence of adequacy for an automated algorithm for scoring breast positioning, based on a PGMI (Perfect, Good, Moderate, Inadequate) quality classification system by investigating the association between technical repeats in the United Kingdom National Health Service Breast Screen Program (UK NHSBSP) and algorithm ratings.