Keywords:
Abdomen, Contrast agents, Pancreas, CT-Quantitative, Experimental investigations, Treatment effects, Cancer
Authors:
T. H. Perik, E. Van Geenen, E. J. Smit, L. A. A. Brosens, M. W. J. Stommel, E. C. Gootjes, K. J. H. M. Van Laarhoven, H. Huisman, J. J. Hermans; Nijmegen/NL
DOI:
10.26044/ecr2021/C-14092
Methods and materials
We present initial data from a prospective study in 12 patients (7 men and 5 women, 47-74 years) with biopsy proven PDAC, treated with chemotherapy between January 2018 and December 2019 (neoadjuvant n=9, palliative n=3). CTP was performed at baseline and follow-up after 3 months.
All patients were scanned on a 320-row detector CT scanner with 160 mm coverage. The amount of contrast agent (400 mg I/ml) is based on body weight (1,3 mg I/kg) with a fixed duration of the injection time of 5 seconds. A test bolus of 15 ml is used to determine the time of contrast arrival in the aorta. CTP was interleaved with a routine diagnostic CECT. Perfusion series started 2s before contrast arrival time in the aorta with 13 acquisitions with an interval of 2s, followed by a diagnostic volume scan in the parenchymal phase at 35s and 9 dynamic acquisitions with 3s interval. At 70s a portal-venous diagnostic scan of the thorax and abdomen was performed, followed by three dynamic acquisitions at 90, 120 and 150s.
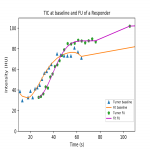
A free-hand drawn region of interest (ROI) was placed in the tumor section with the largest diameter, both at baseline and in a matching section at follow-up. In this ROI tumor enhancement was measured in Hounsfield units (HU). A perfusion analysis tool was developed to fit a stable time-intensity curve (TIC) through the HU values in all dynamic acquisitions. The TIC was used to calculate blood flow (BF; ml/100g/min) based on the Max-slope method: BF = Max slope of TIC / Peak aorta enhancement. The peak of the TIC is the maximum tumor enhancement (HU).
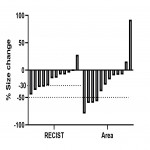
Chemothorapy response was defined in two ways: 1) more than 30% decrease in largest tumor diameter (RECIST-criteria) or 2) more than 50% decrease in area of tumor ROI (mm2), both measured in the same slice.


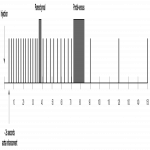


![Fig 6: Percentual change in blood flow (BF) after chemotherapy in responders [R] and non-responders [NR]. Categorized by the RECIST-criteria (p=0,972) and Area (p=0,024).](https://epos.myesr.org/posterimage/esr/ecr2021/158239/media/901820?maxheight=150&maxwidth=150)
![Fig 7: Percentual change in maximum enhancement after chemotherapy in responders [R] and non-responders [NR].](https://epos.myesr.org/posterimage/esr/ecr2021/158239/media/901821?maxheight=150&maxwidth=150)
