Keywords:
Oncology, Paediatric, Radioprotection / Radiation dose, MR, Radiation therapy / Oncology, Radiobiology, Biological effects, Cancer, Toxicity
Authors:
P. U. Sakhavalkar, S. Avula, N. Thorp, B. Pizer, M. Jenkinson
DOI:
10.26044/ecr2022/C-10308
Conclusion
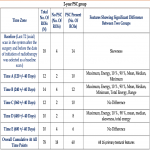
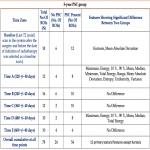
Longitudinal texture analysis showed a significant difference in visibly normal regions of the dentate nucleus between patients with and without qualitative progressive signal changes at 2-year and 5-years. These differences in textural values were dynamic and different texture features showed significant differences at different times points over a 2-year period. Textural values also showed significant differences between groups when analysed cumulatively over a 2-year period.
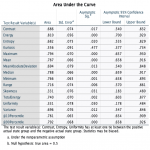
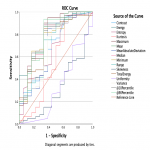
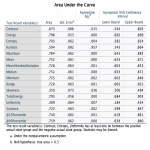
Results of AUC after ROC analysis showed 9 texture features for the 2-year PSC group and 12 features for the 5-year PSC groups with the fair to good ability to distinguish between two groups suggesting the good predictive ability of the texture analysis (Fig 7-10). Skewness and uniformity were not useful for distinguishing the groups with or without PSC in 2-year as well as 5-year groups while kurtosis showed borderline performance. Our results are similar to a study on the classification of brain metastasis where support vector machine-based classification could distinguish between radiation necrosis and brain metastasis with high accuracy of AUC >0.94 [11].
Thus, radiomic texture analysis is a promising quantitative tool to distinguish patients with and without qualitative progressive signal changes even in visibly normal brain areas. Radiomics can predict 5-year signal change such as T2 hyperintensity within the first 2 years after radiotherapy in paediatric patients with medulloblastoma when analysed at different time points and cumulatively.
Predicting these changes earlier may help to identify children likely to manifest these changes in future. A further larger study is planned to examine the wider normal brain and to correlate radiomic findings with clinical features.