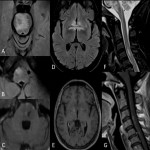
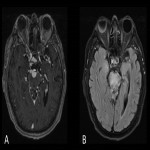
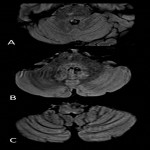
Multiple sclerosis (MS)
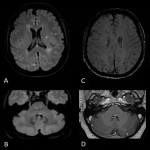
MS is an acquired inflammatory disorder of the Central Nervous System (CNS) that usually starts between adolescence and the sixth decade. Patients that have brainstem lesions show ocular dysmotility, nystagmus, facial sensory loss, trigeminal neuralgia, dysarthria, pyramidal weakness and ataxia. CSF-restricted oligoclonal bands are found in 85% of patients.
Neuroimage
- Diagnosis can be done by MRI if there is evidence of dissemination of lesions in time and space.
- Lesions are ovoid, well-circumscribed, hyperintense on T2-weighted sequences and fluid-attenuated inversion recovery (FLAIR) sequences.
- Acute lesions enhance with gadolinium and may show restricted diffusion. Chronic lesions can be replaced by black holes.
- Perivenular lesions show hypointense central line (central vein sign) in susceptibility-weighted imaging (swi).
- Typical locations are periventricular, pericallosal and deep white matter, cortical and juxtacortical, infratentorial in the brainstem and cerebellum, optic nerves and spinal cord.
- Brainstem lesions are well-defined, more likely in the pons than medulla, and occur in the dorsal and ventral brainstem.
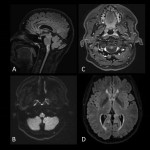
Neuromyelitis Optica Spectrum Disorder (NMOSD)
It is an autoimmune CNS´s astrocytopathy with demyelination due to AQP4-IgG. Patients present optic neuritis, acute myelitis, or brainstem syndromes. Brainstem lesions cause hiccups, nausea, vomiting, deafness, diplopia, vertigo and facial palsies.
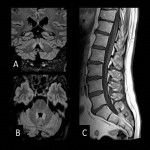
Neuroimage
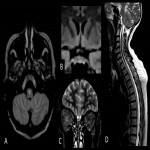
- Longitudinally extensive unilateral or bilateral optic neuritis and transverse myelitis with involvement of ≥3 spinal cord segments are characteristic.
- Lesions are mostly infratentorial, involving brainstem at the medulla. They are linear, T2-hyperintense, occur near the fourth ventricle and can be contiguous with cervical transverse myelitis.
- Diencephalic lesions appear around the third ventricle and rostral midbrain.
- Patchy contrast-enhancement is seen on T1-weighted sequences, particularly periventricular and pericallosal.
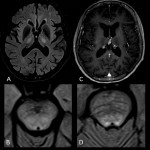
Myelin oligodendrocyte glycoprotein (MOG) antibody-induced demyelination
Up to 42% of the seronegative for AQP4-IgG NMOSD patients, mostly young adults, present serum MOG antibodies. Those suffer bilateral optic neuritis with or without simultaneous myelitis symptoms that can be monophasic or chronic relapsing.
Neuroimage
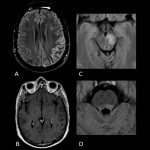
- Lesions involve cortical and deep grey matter, subcortical and deep white matter, retrobulbar optic nerve, diencephalic or the peri-fourth ventricle pons white matter and caudal spinal cord.
- Lesions are hyperintense, large and edematous on T2-weighted sequences.
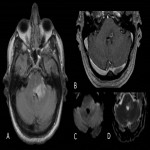
Neuro-Behçet disease
Behçet disease is a multisystemic vasculitis of small vessels. Neuro-Behçet causes brainstem manifestations, alone or in combination with hemispheric or spinal cord symptoms. Other manifestations include oral and genital ulceration, skin problems and fever.
Neuroimage
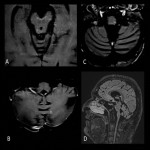
- Lesions are edematous, appear hyperintense on T2-weighted sequences, show microhemorrhages in swi and acute lesions show contrast enhancement on T1-weighted sequences.
- Brainstem is the most commonly involved structure. Other typical locations are basal ganglia, thalamus, and less frequent subcortical white matter and spinal cord.
- Intracranial sinus thrombosis and optic neuritis are common.
- Chronic disease causes infratentorial atrophy and black holes.
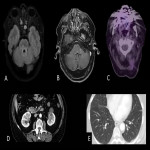
Neurosarcoidosis
Sarcoidosis is a systemic granulomatous disease that rarely involves CNS. It can cause brainstem and cerebellar syndromes. Typical granulomatous lesions in other systems seen on a whole-body CT suggest the diagnosis.
Neuroimage
- Contrast enhancement of leptomeningeal structures around the pituitary stalk and in basal cisterns. Hydrocephalus is possible.
- Brainstem T2- hyperintense lesions are inespecific.
- There are sarcoid masses in the posterior fossa that show noncontiguous contrast enhancement and T2-hypointensity.
Histiocytic disorders
Langerhans cell histiocytosis (LCH) and Erdheim Chester disease (ECD), are malignant disorders that often present inflammatory lesions in the brainstem. Classically, LCH presents in childhood and ECD in adulthood. Clinical manifestations include bone pain, skin and visceral issues. Neurologic symptoms are diabetes insipidus, neurodegeneration with deterioration in cognition, dysarthria, dysphagia, and gait disturbance.
Neuroimage
- Avidly contrast-enhancing space-occupying lesions in the pituitary stalk, choroid plexus, meninges, brainstem, or orbit.
- Progressive symmetric T2-hyperintense lesions appear in the cerebellum, globus pallidus and pons.
- Brainstem lesions, when present, appear simultaneous to the dentate nucleus, pontine pyramidal tracts or the tegmental white matter´s T2-hyperintensity and can have a mottled appearance, spreading into the cerebellar peduncle.
- Contrast enhancement can persist for weeks.
Bickerstaff Brainstem Encephalitis (BBE)
BBE is a variant of Guillain-Barre and Miller Fischer syndromes with specific antiGQ1b antibodies in serum or CSF. Patients have alterations in consciousness, ataxia, ophthalmoplegia, and upper motor neuron signs after a viral illness.
Neuroimage
- There are no MRI findings in up to 70% of the cases.
- T2-hyperintense foci located at the pons, medulla, cerebellum, and thalamus. They usually disappear when patients recover.
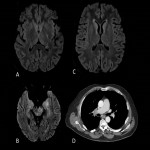
Hurts disease
The most severe form of Acute Disseminated Encephalomyelitis is a rare sporadic demyelinating disease that causes a rapidly progressive fulminant hemorrhagic inflammation of the white matter. Neurologic manifestations are preceded by upper respiratory tract´s infections, can produce high fever, neutrophilic pleocytosis on CSF and leukocytosis.
Neuroimage
- Bilateral and asymmetric lesions occur at the subcortical white matter, thalamus, cerebellum, brainstem and spinal cord.
- Big demyelinating lesions appear hyperintense on T2-weighted sequences, with less oedema than expected for the length and possible patchy contrast enhancement.
- Haemorrhagic foci visible in swi.
Paraneoplastic encephalitis
This entity is secondary to cerebral inflammation due to antibodies that appear in some paraneoplastic syndromes. Anti-neuronal autoantibodies are present and some of them have specific MRI features.
Neuroimage
- Limbic encephalitis show bilateral, medial temporal lobe T2- hyperintensity.
- Anti–NMDA receptor encephalitis: MRI may be normal, but there can be T2-hyperintense lesions in the cerebral or cerebellar cortex, medial temporal lobes, and rarely the brainstem.
Systemic lupus erythematosus (SLE)
SLE is an autoimmune disease that can involve CNS. Patients show headaches, seizures, psychosis, mood disorder, cranial neuropathy, cognitive dysfunction, altered mental status, myelopathy, and movement disorders. Supratentorial cerebritis, aseptic meningitis, stroke, demyelination, transverse myelitis, and rarely brainstem encephalitis are possible.
Neuroimage
- Acute lesions are T2- hyperintense and T1-hypointense, which can show punctate or peripheral contrast enhancement due to oedema, inflammation and demyelination.
Alexander leukodystrophy
Fibrinoid leukodystrophy is rare, fatal and usually is diagnosed in childhood. It starts in the frontal region and extends posteriorly. Subcortical U-fibers are early affected and in end-stages, there is a contrast-enhancing cystic leukomalacia.
Neuroimage
- Lesions are symmetrical and bilateral in frontal white matter, appear hyperintense on T2-weighted sequences, show enhancement on T1-weighted sequences and may present diffusion restriction.
- Affects in order caudate head, globus pallidus, thalamus and brainstem.
- Characteristic periventricular rim.
- Obstructive hydrocephalus is possible.
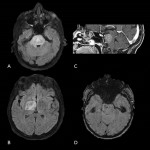
Wilson disease
Hepatolenticular degeneration is a rare multisystemic autosomal recessive disorder of copper metabolism. Symptoms appear in adulthood and neurologic manifestations include dystonia, dysarthria, weakening of hands and pseudo-parkinsonian and cerebellar symptoms.
Neuroimage
- Characteristic bilateral putaminal T2-hyperintensity.
- T2-hyperintense areas can appear involving the midbrain tegmentum and the pons (double panda sign). They are hypointense on T1-weighted sequences in patients with neurologic symptoms.
- Diffusion restriction is possible in early stages.
Wernicke-Korsakoff syndrome
Wernicke encephalopathy is caused by a deficiency of thiamine, common in alcoholics.
Neuroimage
- Areas of T2-hyperintensity at the mammillary bodies, dorsomedial thalami, tectal plate, periaqueductal grey matter and around the third ventricle.
- These can show contrast enhancement on T1-weighted sequences and restriction of diffusion.
An infectious origin of the brainstem inflammation must be excluded before introducing immunotherapy.
Listeria
Listeria monocytogenes infects CNS and causes symptoms in immunocompromised patients. It causes fever, headaches, and vomiting, followed by asymmetric brainstem dysfunction.
Neuroimage
- T1-hypointense and T2-hyperintense foci involving the brainstem, especially the floor of the fourth ventricle and cerebellum.
- Presence of ring-enhancing with central restricted diffusion and T2-hyperintense abscesses in the brainstem.
- Trigeminal nerve enhancement is possible.
Tuberculosis
CNS´s involvement is rare but it is described in immunocompromised patients with high morbimortality. The disease spectrum includes meningitis, hydrocephalus, cerebritis, tuberculoma, abscess, and spinal tuberculosis.
Neuroimage
- Brainstem encephalitis appears as leptomeningeal contrast enhancement of the basal cisterns.
- CSF is turbid, hyperintense on FLAIR and shows contrast enhancement.
- Tuberculomas have solid enhancement in the noncaseating phase and ring enhancement with T2-hypointense centre in the caseating stage.
Viral infections: enterovirus
Enteroviruses are a common infectious cause of brainstem infectious encephalitis. EV-A71 is the most common subtype; it causes hand-foot-and-mouth disease, upper respiratory infections and gastroenteritis. 25% of the patients have neurologic affection.
Neuroimaging findings
- Lesions are hypointense on T1 and hyperintense on T2.
- Specific locations of E-A71-induced lesions: dorsal pons, medulla followed by the cerebellar dentate nucleus, midbrain, and thalami with no supratentorial lesions.