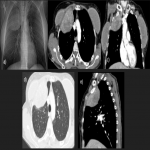
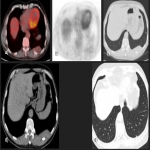
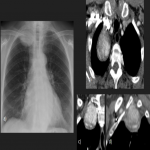
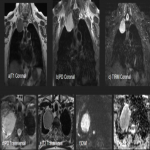
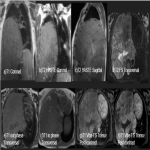
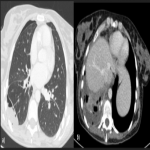
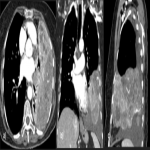
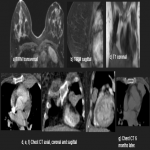
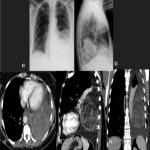
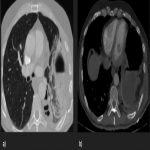
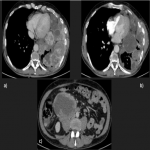
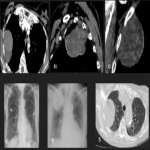
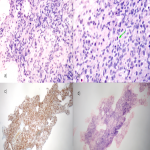
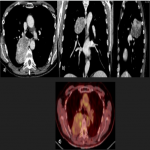
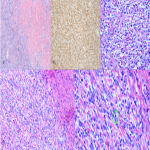
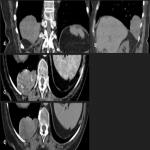
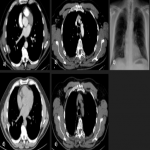
Solitary tumor of the pleura is a rare primary tumor of the pleura that has presented an increase in its incidence due to the elevated performance of radiological tests, being in most cases an incidental finding. [1]
The pleura could be affected by metastatic spread of neoplasms that represent 90% of pleural tumors in conjunction with lymphomas. The other 10% of pleural tumors are primary neoplasms and include in the first place the malignant pleural mesothelioma and in the second the solitary fibrous tumor. [2]
Solitary fibrous tumors are mesenchymal tumors that can occur at any anatomical site, including superficial and deep soft tissues and within visceral organs and bone, being the extrapleural location more common [3][4]. For this reason, pleural solitary fibrous tumors (PSFT) account for less than 5-10% of cases of pleural tumors, with a prevalence of 2.8 cases per 100,000 population. PSFTs affect men and women equally and the most common age peak incidence is between 40-70 years. The prognosis is uncertain, being in most cases a benign tumor, although up to 12% of the entire cases are malign, and the proportion of benign PSFT and malign is 7:1. [5]
The etiology is unknown, being the genetic cause unlikely, with no association with the exposure of asbestos, tobacco, or other environmental factors. [1]
PSFTs are soft tissue neoplasms of pluripotent fibroblastic or myofibroblastic cells that in the most recent World Health Organization (WHO) guidelines (2016) have been combined into a single designation as solitary fibrous tumor/hemangiopericytoma (SFT/HPC). The genetic hallmark of PSFTs is a paracentric inversion involving chromosome 12q, resulting in the fusion of the NAB2 and STAT6 genes, that result in a feedforward loop of constituted EGR1-mediated transactivation of proliferation and survival associated growth factors. [4-5]
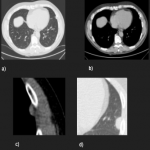
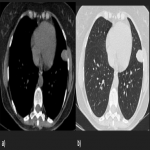
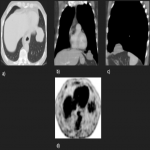
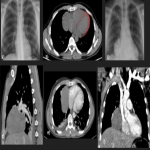
Most tumors present as slow-growing painless masses and are asymptomatic or have non-specific symptoms, usually found incidentally on imaging. Symptoms may be chest pain, dyspnea, cough, weight loss, thoracic pain, superior vena cava syndrome, as well as paraneoplastic syndromes such as Doege–Potter Syndrome that produce the induction of severe hypoglycemia and hypertrophic osteoarthropathy, known as Pierre-Marie-Bamberger syndrome, that is characterized by clubbing of the fingers due to bone surface and soft tissue calcification. It is known that there is a correlation between the tumor size and symptoms, being asymptomatic patients with tumors <10cm in general and symptomatic >10cm. [1-7]
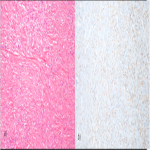
The development of multivariate risk models has resulted in improved prognostication over the traditional benign/malignant distinction. The most widely used model for metastatic risk incorporates mitotic count (≥2mitoses/mm2), patient age (≥55 years), tumor size stratified by 5cm tiers to classify tumors into intermediate and high-risk groups, and tumor necrosis. Despite this, differentiation between malignant and benign PSFT is done using histological features like the presence of tumoral necrosis; the presence of atypical nuclei, cellular pleomorphism, and hypercellularity ( ≥4 mitosis/10 HPF (high power field)). [4-6-7]