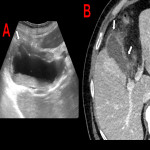
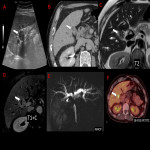
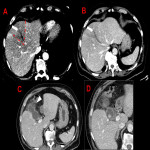
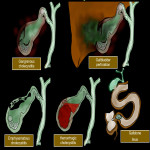
A. Gangrenous cholecystitis
When acute cholecystitis is severe or prolonged in time, excessive gallbladder distension leads to increased intraluminal pressure that can reach a point where the vascularization of the wall is compromised, with subsequent necrosis.
Gangrenous cholecystitis is the most common complication of acute cholecystitis, accounting for up to 30% of cases. An increased risk of gangrenous cholecystitis has been reported in elderly male patients with diabetes mellitus, elevated bilirubin and coronary artery disease. Due to parietal necrosis, US Murphy's sign may be negative in up to one third of cases.
The US presentation is similar to that of acute cholecystitis:
- Diffuse thickening of the gallbladder wall, although it can be irregular
- Presence of gallstones
- Perivesicular fluid
- Focal wall thinning areas
- Endoluminal slough membranes
Many of these ultrasound signs can also be found on CT, which sensitivity in detection parietal necrosis is greater.
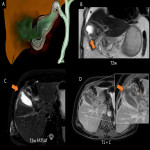
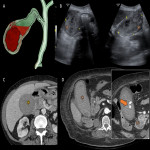
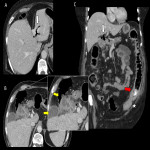
B. Perforated cholecystitis
Perforated cholecystitis is a severe complication of acute cholecystitis and its variants (emphysematous, gangrenous or haemorrhagic). It is described in up to 5-10% of patients, with a mortality of up to 40% in some series.
US is usually the initial technique for approaching perforated cholecystitis, but it is advisable to complete with CT if there is any doubt as to the extent of the perforation.
The different imaging tests show:
- Discontinuity of the gallbladder wall (more frequent in the fundus)
- Loss of the normal shape of the gallbladder
- Marked perivesicular inflammatory changes
- Formation of hepatic or peritoneal abscesses in the vicinity
Special attention should be taken to the possibility of free intraperitoneal gallstones, which may perpetuate infections or fistulise to neighboring organs.
With perforated cholecystitis, it is important to scrutinise neighbouring vascular structures for possible associated septic thrombosis.
Treatment of perforated cholecystitis should be consensual and multidisciplinary based on the type of perforation, the patient's history and general condition, and may require open surgery, laparoscopic surgery, percutaneous approach (cholecystostomy) or mixed approaches.
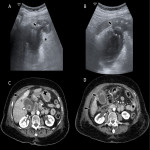
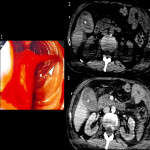
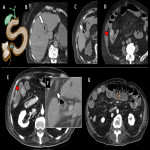
C. Emphysematous cholecystitis
Emphysematous cholecystitis is a rare variant of acute cholecystitis. It is most common in men aged 50-70 years, and strongly associated with diabetes mellitus. Its clinical course is insidious, and the patient’s general status can deteriorate rapidly. It may even present afebrile.
Cystic artery involvement, parietal necrosis and infection by gas-producing organisms play a role in its development.
It can be seen on abdominal plain radiography given the presence of gas, although it is not very sensitive. Its US is tricky, as the gas generates a reverberation artefact that may obscure the full assessment of the gallbladder. It can be confused with a porcelain gallbladder, multiple gallstones or even with the hepatic angle of the colon.
CT is superior in delimiting the extent of emphysematous cholecystitis. Emphysematous cholecystitis may have endoluminal, parietal and peritoneal air (the later only if there is associated gallbladder perforation).
Management can be either surgical or percutaneous.
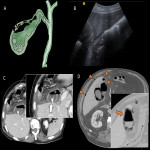
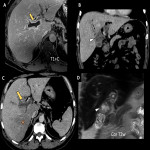
D. Hemorrhagic cholecystitis
Hemorrhagic cholecystitis is a haemorrhagic complication of acute cholecystitis. It must be differentiated from haemobilia, which only refers to bleeding within the gallbladder or biliary tree in the absence of inflammation. It can cause gastrointestinal bleeding if the blood content drains trough Vater’s papilla. Clots in the bile duct can cause biliary obstruction.
Risk factors include hemorrhagic diathesis, anticoagulant therapy and trauma. It is thought to be secondary to a vascular injury resulting from parietal inflammation.
US shows:
- Unstructured gallbladder wall
- Filled with echogenic content which may appear to be dense biliary sludge at first glance
However, CT will show a distended gallbladder at the expense of dense material compatible with clots. Active contrast extravasation may be seen if there is an underlying lesion.
The approach may be surgical, interventional (as cystic artery embolisation can be performed) or percutaneous (cholecystistomy).
OTHER COMPLICATIONS...
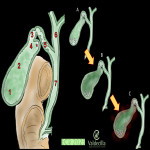
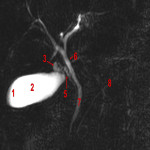
E. Mirizzi syndrome
Rare complications that results from extrinsic compression of the extrahepatic biliary duct due to the gallbladder's process or an impacted gallstone. It can mimic other pathologies such as cholangiocarcinoma. This condition can lead to the development of a cholecystoduodenal fistula.
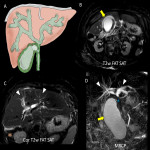
F. Xanthogranulomatous cholecystitis
Xanthogranulomatous cholecystitis is a rare variant of chronic cholecystitis. On pathology, it has a transmural histiocyte infiltrate. It occurs most frequently in women between 60-80 years of age. It may present as right upper quadrant pain, fever and leukocytosis, thus mimicking acute cholecystitis. Its main differential diagnosis is hilar cholangiocarcinoma or gallbladder carcinoma.
US and CT show diffuse thickening of the gallbladder with nodular formations in the gallbladder wall. Cholecystectomy is recommended, however intraoperative pathology might be necessary to exclude malignancy.
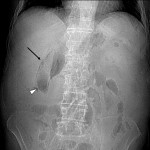
G. Gallstone ileus
Gallstone ileus is a rare cause of intestinal obstruction. The term "ileus" is a misnomer, as gallstone ileus is secondary to a mechanical obstruction due to an endoluminal large gallstone. It usually stops at the ileocecal valve or terminal ileum and leads to small bowel obstruction. For it to develop, there must be an enterobiliary fistula, usually cholecystoduodenal, although it can also be cholecystocolonic (in this case the gallstone is in the colon) or cause gastric outlet obstruction (Bouveret's syndrome). It is characterized by Rigler's triad of aerobilia, intestinal obstruction and visible endoluminal lithiasis.
Early surgical management improves morbidity and mortality in these patients.
H. Pylephlebitis
Pylephlebitis is a thrombotic obstruction of the portal vein and its branches secondary to neighbouring infection. The presentation is non-specific and depends on the underlying infectious pathology. Although it is more frequent in diverticulitis, appendicitis and pancreatitis, it can occur in any proinflammatory state such as cholecystitis.
Ultrasonography will show an absence of portal flow with echogenic occupation of the portal lumen. MRI and CT scan will show a portal thrombus and its extension and the extent of the associated complications will be better defined.
Treatment of pylephlebitis is a priori medical with antibiotics and anticoagulants.