Type:
Educational Exhibit
Keywords:
Cardiac, Cardiovascular system, CT, Diagnostic procedure, Image compression, Congenital, Ischaemia / Infarction
Authors:
M. B. Barrio Piqueras, C. Urtasun Iriarte, M. Jiménez Vázquez, C. Mbongo, F. M. Caballeros, G. Bastarrika Alemañ, A. Ezponda Casajús
DOI:
10.26044/ecr2023/C-13057
Findings and procedure details
This pictorial review includes the most common cardiac findings on routine chest-CT, based on the anatomical location:
- Coronary arteries[1]:
-
- Anatomical variants and anomalies: variations in coronary anatomy are often associated with congenital heart diseases or sudden death in young adults.
-
-
- Variants: 3 types of dominance (which branch supplies the posterior descending artery;PDA): right coronary artery(RCA dominance), circumflex(CX), and both(co-dominance).
-
- Anomalies are related to the origin of the coronary arteries and may be benign or dangerous
-
-
-
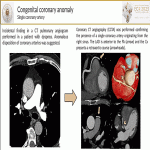
- The single coronary artery(SCA, one coronary artery emerges from a single coronary ostium in the aorta), is a rare finding. The SCA can arise from the right cusp with the LMCA coursing anterior to the RV outflow tract or originate in the left cusp with the RCA coursing posterior to the aorta.
- The CX arises from the right aortic cusp and courses posterior to the aorta.
- The RCA originates in the aorta superior to the cusp.
- Miscellaneous anomalies: congenital hypoplasia or origin of the coronaries from the subclavian or internal mammary arteries.
-
-
-
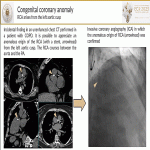
- RCA arises from the left aortic cusp and courses between the aorta and the pulmonary artery(PA).
-
-
-
- LMCA arises from the right cusp and curses between the aorta and the PA.
Both show the risk of compression in the interarterial segment.
-
-
-
- ALCAPA(anomalous origin of the left coronary artery from the pulmonary artery).
-
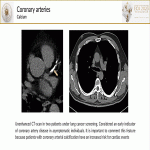
- Coronary artery calcium[2] can be an early indicator of coronary artery disease in asymptomatic individuals. It is the most frequent cardiac finding on chest-CT and can be characterized in non-ECG-gated-unenhanced-CT. These patients have an increased risk for cardiac events.
-
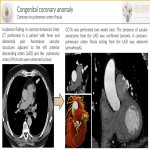
- Coronary aneurysms(CA)[3] develop in several scenarios and show different symptoms, radiological features, and outcomes. Depending on their etiology, they are classified into atherosclerotic, inflammatory, and non-inflammatory. It is important to describe their morphology (fusiform or saccular), diameter, wall calcification, luminal thrombosis, significant stenosis, origin, and termination, number, segments affected, and potential complications like myocardial abnormalities, fistula formation, or rupture.
-
- Coronary artery fistula(CAF) is an abnormal communication of a coronary artery with cardiac chambers or with any segment of the systemic or pulmonary circulation. Coronary to pulmonary artery fistula accounts around 15-30% of all the CAFs.
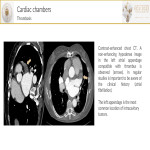
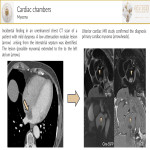
- Cardiac chambers:
-
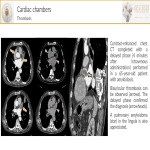
- Intracavitary thrombus[2] is the most common filling defect in cardiac chambers. On CT, thrombi do not enhance but chronic ones can appear heterogeneous with a peripheral fibrous capsule or could calcify.
-
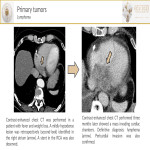
- Tumors[2](myxoma): Cardiac myxomas are the most common primary neoplasm. They arise from the interatrial septum near the limbus of the fossa ovalis. Myxomas can be asymptomatic or present with cardiac obstructive symptoms (due to intracavitary extension), embolic phenomena, and constitutional symptoms. In contrast-enhanced-chest-CT, myxomas are usually lower in attenuation compared to the myocardium. Myxomas may be heterogeneous.
-
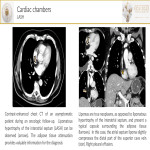
- Lipomatous hypertrophy of the interatrial septum;LASH)[4] is a benign lesion characterized by accumulation of fat in the interatrial septum of>2 cm in thickness. On chest-CT, LASH shows an attenuation coefficient of adipose tissue. Another atrial septum mass is the lipoma, characterized by the presence of a capsule.
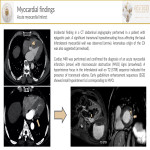
- Myocardium:
-
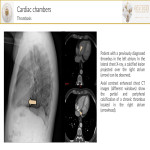
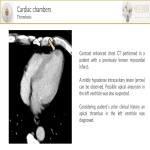
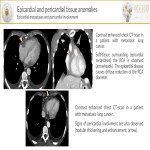
- Myocardial infarction: focal or linear subendocardial area of decreased myocardial enhancement may be suggestive of this pathology. The sensitivity of CT is higher for detecting chronic infarctions. Radiologists should be concerned about the heartbeat artifact prior to suggesting this diagnosis.
-
-
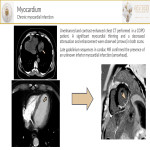
- Dilated: It is characterized by an impaired contraction of the left or both ventricles in the absence of ischemic heart disease. Patients present with progressive heart failure and the etiology can be idiopathic, genetic, viral, metabolic, or toxic. On non-ECG-gated-CT, a dilated left ventricular chamber is seen with a uniform left ventricular wall thickness.
-
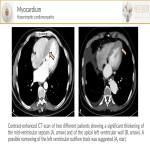
- Hypertrophic cardiomyopathy(HMV) is a genetic disorder that occurs in the absence of any hypertrophic stimulus and is the most common cause of sudden death in healthy young adults. On axial-CT images, the typical thickening of the mid-ventricular septum and narrowing of the left ventricular outflow track can be seen.
-
-
- Fibroma is a congenital neoplasm and is the pediatric cardiac tumor more commonly resected. This entity is associated with heart failure, arrhythmias, and sudden death. CT-scan demonstrates a homogeneous soft tissue mural mass with variable attenuation. Dystrophic calcification can be seen in ¼ of cases.
-
-
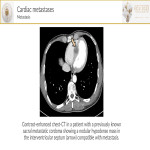
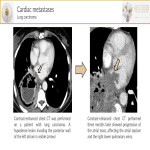
- Metastasis[2] is much more common than primary tumors. On chest-CT, they can manifest as a pulmonary or mediastinal mass with direct invasion, as myocardial masses (hematogenous spread), as a central mass extending to the left atrium (venous extension), or as a pericardial effusion with nodularity (lymphatic extension).
-
- A hyperdense myocardium, compared to a relatively hypodense left ventricular cavity or a hyperattenuating aortic wall compared to a relatively hypodense aortic blood pool in unenhanced-CT-scan may be seen in patients with severe anemia.
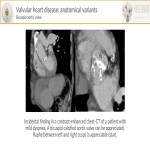
- Valvular heart disease:
-
-
- Bicuspid aortic valve[2] is the most common cardiac congenital lesion. It is associated with aortic root and ascending aortic dilatation, aortic coarctation, Turner´s syndrome, patent ductus arteriosus…On chest-CT, the cusps of the bicuspid valve show unequal size (one is composed of two fused cups).
-
-
- Mitral annular calcification is common in females over 65 years, in those with myxomatous degeneration of the mitral valve, and with elevated left ventricular pressures.
-
-
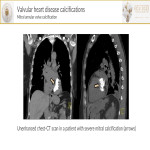
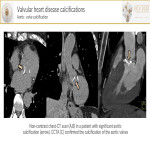
- Aortic valve calcification(AVC) is commonly found in thoracic CT-scans(especially in the elderly). AVC is considered a marker for significant aortic stenosis.
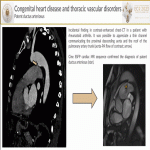
- Congenital heart disease, and thoracic vascular disorders:
-
- Atrial septal defect[2]: Most of them are secundum defects, near fossa ovalis. In contrast-enhanced-chest-CT, great atrial defects may be seen.
-
- Patent ductus arteriosum is a congenital cardiac anomaly where there is persistent patency of the ductus arteriosus, a normal connection of the fetal circulation between the aorta and the pulmonary arterial system. Left-to-right shunting is possible[6].
-
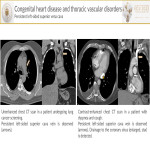
- Persistent left superior vena cava is caused by abnormal development of the coronary sinus during the early stages of fetal life.
-
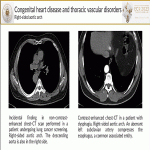
- Right-sided aortic arch is found when it courses to the right of the trachea. The two most common are the right-sided aortic arch with mirror image branching and the right-sided aortic arch with an aberrant left subclavian artery(ALSA)[7].
-
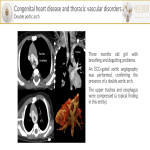
- Double aortic arch[8] results from the persistence of right and left arches during aortic development. This entity could cause esophagobronchial compression and can be associated with other developmental anomalies.
-
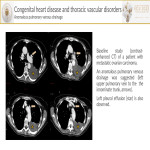
- Anomalous pulmonary venous drainage is a rare congenital cardiovascular condition in which some of the pulmonary veins drain into the systemic circulation.
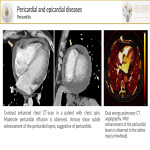
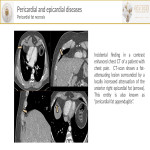
- Pericardial and epicardial diseases[9]:
-
- Pericarditis leading causes in developed countries include iatrogenic, post-traumatic, after radiation therapy, mediastinal tumors, and cardiac interventions. Pericarditis could also occur early after transmural infarction. On chest-CT, pericardial layers are thickened(>4mm) and show diffuse enhancement after contrast administration.
-
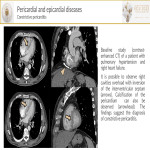
- Constrictive pericarditis consists of a decrease in pericardium compliance. Calcification of the pericardium is suggestive of the disease. Contrast-enhanced CT should also show:
-
-
- Signs of cardiac failure like pleural effusion
- Leftward deviation of the interventricular septum
- Retrograde flow of contrast into a dilated inferior vena cava and hepatic veins
-
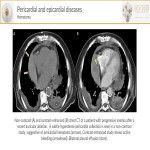
- Pericardial effusion is an abnormal accumulation of pericardial fluid due to different causes (heart failure, infection, neoplasia…). Inspection of the region and the morphology of the pericardial layers is necessary to rule out a subjacent malignancy. Three levels:
-
-
- <10 mm:small
- 10-20 mm:moderate
- >20 mm:large
-
- Pericardial hematomas. The CT-imaging characteristics of a pericardiac hematoma depend on the age of collection.
-
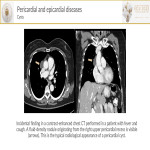
- Pericardiac cysts are benign unilocular masses of celomic origin and normally asymptomatic. On CT-scan they appear as an encapsulated fluid-filled structure without internal septa or nodules that are attached to the pericardium. The most typical location is the right cardiophrenic angle.
-
- Malignant pericardial involvement (direct invasion, metastases, venous extension). CT can show pleural effusion with pericardial adhesions, thickening and nodular changes and layer enhancement.
-
- Pericardial fat necrosis is a benign entity of unknown cause that manifests with sudden onset of chest pain, mimicking other diseases like myocardial infarction and pulmonary embolism. CT-scan shows a fat-attenuating lesion surrounded by a locally increased attenuation of the anterior mediastinal fat adjacent to the pericardium.