Concept
Synovial sarcoma (SS) is a high-grade sarcoma, representing 5-10% of all soft tissue sarcomas. It arises from primitive mesenchymal cells with epithelial and not synovial differentiation as previously thought. (1)
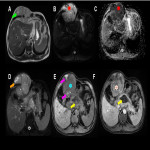
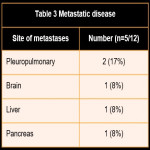
It mainly affects the extremities (about 80%), near the joints of the lower and upper extremities (the knee joint, head, and neck are the most affected). However, it can affect any organ, but it is very rare in the intrathoracic cavity. SS represents 14.7% of primary intrathoracic sarcomas, being the most common type of primary intrathoracic sarcoma. (1, 2)
Most cases of primary intrathoracic SS occur in the pleura and lung, whereas those of the heart and mediastinum are rare. (2) Intrathoracic lesions have a worse prognosis, with a high recurrence rate and worse prognosis. (1)
Epidemiology, etiology and histology
Most patients present between 15 and 35 years, and 90% of cases are reported before 50 years. Both sexes are equally affected. (3, 4)
The etiologic cause of SS is thought to be a chromosomal abnormality that usually occurs in more than 90% of cases, known as T(x; 18) (P11.2; q11.2), resulting in fusion formation of SS18-SSX oncogenes. (1, 2)
Histologically, it presents three types: monophasic (most common), biphasic, and poorly differentiated (worst prognostic). (1)
Clinic
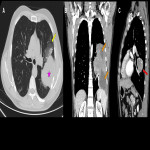
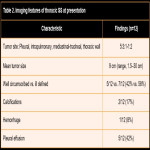
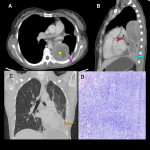
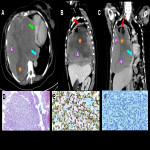
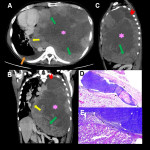
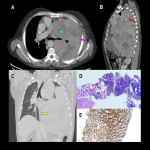
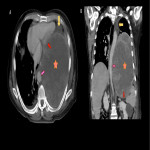
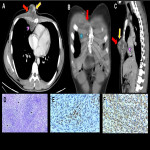
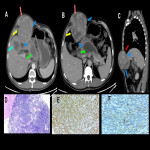
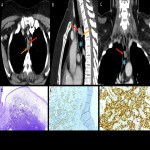
The clinical presentation of primary intrathoracic sarcomas is usually nonspecific and includes chest pain, dyspnea, cough, and hemoptysis. Imaging usually reveals intrathoracic masses, accompanied by bilateral pleural effusion. (5)
In a series of cases it was found that the majority of patients presented symptoms, among the most frequent cough and chest pain, however, some patients were asymptomatic. Some courses with pleural or pericardial effusion or hemothorax and pneumothorax. (1)
Diagnostic methods, treatment and Forecast
Since primary intrathoracic SS is rare, there is still inexperience in its clinical diagnosis and treatment.
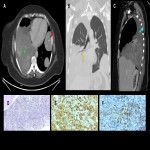
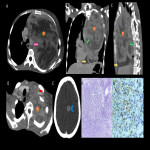
The confirmatory diagnosis is through immunohistochemistry and pathognomonic molecular translocation, with a sensitivity close to 100%. (5, 6)
From a histological point of view, since it is resectable in soft tissues, it is not difficult to diagnose by means of sufficient samples under a microscope; however, the differential diagnosis remains difficult in patients with atypical mediastinal morphology, especially when dealing with round cell tumors. Small and spindle cells, sarcomatoid, leiomyosarcoma, mesothelioma, and fibrosarcoma, among others, as well as small cells obtained by puncture and not surgically. (2, 5, 6)
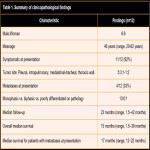
The treatment will depend mainly on the tumor's location and the surgery's difficulty since it requires a safe margin around the soft tissue tumor of at least 2 cm. The size, depth, and location of the tumor associated with the possibility of achieving complete resection of it are factors that play an important role in the prognosis of these patients. (2, 6, 7)
Due to all of the above, the medical management of these patients is multidisciplinary, both for diagnosis and treatment.
The prognosis is poor, with an overall 5-year survival rate of 50%. (6, 7)
Differential diagnosis
It can be confused with other pulmonary sarcomas, histopathologically, such as leiomyosarcoma, fibrosarcoma, and malignant tumors of the peripheral nerve sheath, which requires a cytogenetic study for a definitive diagnosis. (2, 5, 8, 9)
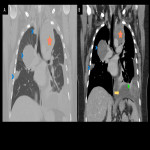
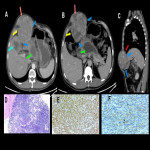
In this educational poster, we retrospectively reviewed the different localization of synovial sarcoma in our Institution from 2019 to 2022, focusing on the thoracic zone. Imaging findings were performed by CT and MR images, and the confirmation was made by anatomopathological correlation.