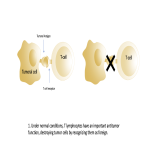
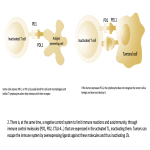
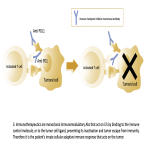
Complications usually occur in the first 3 months of onset (up to 12 months) and resolve in about 2-3 months. There have been described a series of factors that favor the development of adverse events:
- History of autoimmunity and chronic infections
- Male sex
- Renal failure (grade 3-4)
- Combined therapies (PD1 + CTLA4)
Otherwise, the use of pretreatment corticosteroids and female sex are considered protective factors.
From the immune-related adverse effects described in the scientific literature, we found some cases of hypophysitis, synovitis, enteritis,different types of pneumonitis and colitis. These will be explained more in detail in the next lines.
1. Pneumonytis
Pneumonitis is a focal or diffuse inflammation of the lung parenchyma. Studies have described pneumonitis in the context of ICI, classifying them in five radiological subtypes.
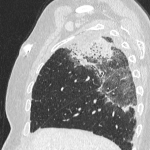
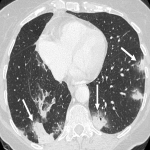
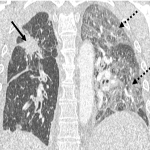
- Cryptogenic organizing pneumonia, the most prevalent in our center, consisting on a discrete patchy or confluent consolidation ± air bronchograms predominantly in a peripheral or subpleural distribution. Ground glass opacities is also observed in some cases, seen as discrete focal areas of increased attenuation with preserved bronchovascular markings.
In our center there was a case of a patient that after 2 months of treatment with Pembrolizumab in a PET CT study showed patchy peripheral consolidations, being diagnosed with inflammatory pneumonitis. This patient died 2 months later due to an infectious pneumonia.
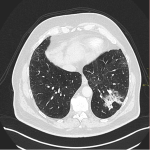
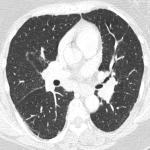
- The interstitial subtype CT findings consists of subpleural reticulation, with interlobular septal thickening and peribronchovascular infiltrates.There was a case in our center of a patient treated with Atezolizumab with lung cancer.
- The hypersensitivity subtype is described as centrilobular ground glass nodules and air trapping.
- The pneumonitis not otherwise specified subgroup is characterized by a mixture of nodular and other subtype patterns on CT.
There are no pathognomonic radiographic features to distinguish ICI-related pneumonitis from pneumonitis of another etiology. Clinical history of concomitant ICI use, lack of infective symptoms and progressive changes despite antimicrobial is indicative of ICI-induced pneumonitis.
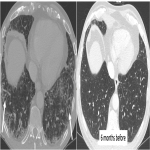
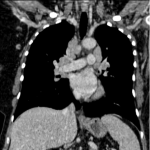
There is another rare type of lung affection, called sarcoid reaction. It is characterized by bilateral and symmetric hilar and mediastinal lymphadenopathy of new appearance +/- alterations in the parenchyma without infection and with evidence of response at other levels. It is more common in melanoma treated with anti-CTLA4. There was a case in our center where a patient that after 5 months of being treated with Pembrolizumab developed a sarcoid reaction. Treatment was changed to Dabrafenib and Trametinib. CT imaging findings disappeared a year after.
2. Hypophysitis
Hypophysitis is inflammation of the anterior lobe of the pituitary gland which presents with headache, fatigue, dizziness and memory impairment. Most patients have anterior pituitary hormone deficiencies at presentation and hormone replacement should be instituted soon after diagnosis.
It has been reported in patients with CTLA-4 ICIs and in patients treated with anti PD-1 or anti PD-L1 ICIs. It is the most common endocrine irAE in patients receiving ipilimumab. It typically presents at 6–12 weeks after initiation of anti CTLA-4 therapy.
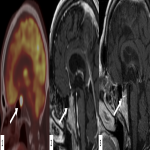
MRI findings include an enlarged pituitary gland and stalk with variable heterogeneous or homogeneous enhancement.
Treatment is a form of high-dose glucocorticoids and temporary or complete cessation of ICI treatment.
Resolution of pituitary findings at MRI along with resolution of clinical symptoms is often noted during the course of immune-related hypophysitis, where MRI plays an important role for both detection and monitoring of this irAE
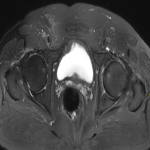
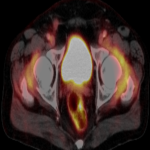
A case of hypophysitis was described in our center in a patient treated with ipilimumab due to a melanoma. It was an incidental finding while routine PET TC, where there was a high FDG uptake in the pituitary gland. An MRI was performed, where there was evidence of a solid mass in the sella turcica. Two months later, after corticosteroid treatment, the mass disappeared, confirming the autoinflammatory etiology.
3. Colitis and enteritis
Colitis and enteritis are the most frequent severe complications. They can reach high mortality if treatment with corticosteroids is delayed.
Typical clinical features are diarrhea, abdominal pain and fever.
Imaging can depict signs of colitis/enteritis on CT as well as its complications, such as bowel perforation, obstruction and toxic megacolon.
Radiological findings are diffuse wall thickening, mucosal enhancement, submucosal edema and fat striation.
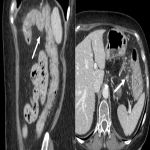
There was a case of enteritis in our center, a 73 year old woman with breast cancer that after 3 months of treatment with Bevacizumab and Pembrolizumab started with diarrhea and vomiting. Generalized thickening of the small bowel wall, more evident in the jejunum and proximal ileum associated with vascular engorgement of the mesenteric vessels.
As far as colitis is concerned, two distinct forms have been reported.
The more common pattern is diffuse colitis with mild bowel wall thickening, mesenteric vessel engorgement and a fluid-filled colonic distension.This was the case of a patient in our center, who was treated for lung cancer with Pembrolizumab and 6 months later started with abdominal pain and diarrhea. An autoimmune episode was diagnosed.
The other type consists of a segmental colitis associated with diverticulosis, and affects a segment with pre-existing diverticulosis with superimposed circumferential bowel wall thickening and mesenteric vessel engorgement.
4. Hepatobiliary toxicity
Pancreatitis is a rare irAE. Imaging is indistinguishable from pancreatitis of any other etiology. Pancreatitis has also been observed in association with anti CTLA-4-induced enterocolitis.
Hepatitis is typically asymptomatic, diagnosed as an elevation of transaminase on routine blood tests.
The CT findings described in these patients included new mild hepatomegaly, periportal oedema, periportal lymphadenopathy and diffuse hypoattenuation of the liver. These imaging findings are indistinguishable from an acute hepatitis of another aetiology, leading to a diagnosis of exclusion.
5. Rheumatological toxicity
Mild or moderate myalgias, arthralgias and non-septic arthritis have been reported. Treatment with non-steroidal anti-inflammatory drugs are recommended for mild arthralgias and possible low-dose steroids.
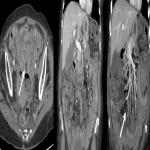
In our center there was a case of bilateral hip synovitis in a patient that underwent immunotherapy due to hypopharynx cancer.The patient referred an important bilateral hip pain that unabled walking. An MRI study was performed and showed a small amount of fluid in both hip joints and a slight alteration of the signal intensity of the musculature adjacent to both coxofemoral joints.