Vocal cord paralysis (VCP) is the loss of mobility of the true vocal cords secondary to a mechanical cause infiltrating the glottis or a neural lesion affecting the vagus (CN X) or recurrent laryngeal nerves (RLN). These nerves provide motor innervation to the intrinsic muscles of the larynx and travel a long distance from the skull base into the upper mediastinum.
Most cases of VCP are unilateral due to a compressive mass, although up to 1/3 may be bilateral. VCP can be classified in central or peripheral, with central causes being about 10% and the vast majority are peripheral.
The main symptom of unilateral VCP is dysphonia but it can also manifest as hoarseness, aspiration episodes, liquid dysphagia, vocal fatigue and shortness of breath.
It is important to note that up to 40% of people with unilateral VCP are asymptomatic at the time of diagnosis.
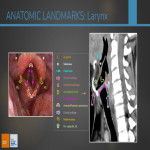
ANATOMY OF THE LARYNX
The larynx is a cervical hollow structure between the oropharynx and trachea, anchored on an external frame formed by the hyoid bone and six cartilaginous structure, the first three are unpaired and the rest are paired.
- Epiglottis
- Thyroid
- Cricoid
- Arytenoid cartilages
- Cornicuated cartilages
- Cuneiform cartilages
This cartilaginous “skeleton” forms the support of the larynx and is coated by an inner mucosal layer, shaping several prominent ridges and folds.
The vocal cords are a double layered mucous membrane infolding that stretch horizontally across the laryngeal cavity.
Three paralell structures, the false vocal cord, laringeal ventricles and true vocal cords, divide the larynx into (from cranial to caudal order):
1- Supraglottis: extends from the tip of the epiglottis to the laryngeal ventricle and it contains:
- Epiglottis
- PE fat
- Arytenoid cartilages
- AEF
- False vocal cords = superior layer of infolded membrane
2- Glottis: extends towards an arbitrary plane located 1 cm below the level of the true vocal cords. It contains:
- True vocal cords = formed from the inferior layer of infolded membrane and contain the thyroarytenoid (lateral fibers) and vocalis muscles (medial fibers).
- Laryngeal ventricles
- Cricoarytenoid joints
- Anterior/posterior comissures
3- Subglottis: extends from the plane under the true vocal cords (1 cm under the laryngeal ventricle) till the inferior margin of the cricoid cartilage.
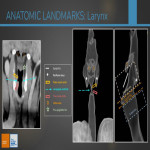
Vocal cord movement is controlled by the intrinsic laryngeal muscles (ILM), which have a complex and hard to remember nomenclature. We must emphasize on these 4 anatomic references in order to help us categorize them according to their point of origin:
- Epiglottis
- Aryepiglottic muscle (within the aryepiglottic fold)
- Thyroid cartilage
- Thyroepiglottic muscle
- Thyroarytenoid muscle (lateral fibers of true vocal cords)
- Cricoid cartilage
- Cricothyroid muscle
- Posterior cricoarytenoid muscle
- Lateral cricoarytenoid muscle
- Arytenoid cartilages
- Oblique arytenoid muscle
- Transverse or interarytenoid muscle
- Vocalis muscle
The muscles that control the inlet of the larynx are the aryepiglottic, oblique arytenoid and thyroepiglottic muscles and the ones that move the vocal ligaments are the cricothyroid, thyroarytenoid, posterior cricoarytenoid, lateral cricoarytenoid, transverse arytenoid and vocalis muscles.
The only abductor muscle amongst this group is the posterior cricoarythenoid muscle.
All ILM are innervated by the RLN, except for the cricothyroid muscle which is innervated by the superior laryngeal nerve (branch of the NC X).
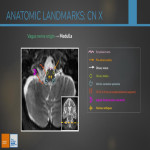
ANATOMY OF THE VAGUS NERVE (CN X)
Tenth and longest cranial nerve, originating in the medulla oblongata and has a sensitive, motor, sensorial and parasympathetic components.
It can be divided into three segments:
1) Intracranial:
Nucleus ambiguus gives rise to the motor fibers that innerve the ILM and is located:
- between the medullary pyramids and the inferior cerebellar peduncle
- posteriorly to the inferior olive
- anterolaterally to the lower part of the fourth ventricle.
The CN X exits the medulla oblongata through its posterolateral margin, between the olivar sulcus and inferior cerebellar peduncule.
It continues allong the lateral cerebelomedullary cisterns and emerges from the skull base via the pars vascularis located in the posterolateral half of the jugular foramen, in close proximity with the glossopharyngeal (NC IX) and accesory cranial nerves (NC XI).
2) Cervical:
Descends throughout the neck within the carotid sheath:
- Posteromedial to the internal jugular vein
- Posterolateral to the internal/common carotid artery
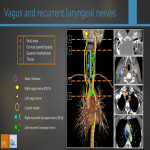
3) Upper mediastinum:
At this level right and left vagus nerve pathways differ:
Right CN X =
- Runs anterior to the origin of the right subclavian artery and posterior to the sternoclavicular artery and brachiocephalic vein.
- Below the right subclavian artery, the RLN branches from the CN X.
Left CN X =
- Runs between the common carotid artery/left subclavian artery and posterior to the sternoclavicular artery and brachiocephalic vein.
- Crosses anterior to the aortic arch, where the RLN branches from the CN X.
Both CN X enter the upper abdomen through the esophageal hiatus (at the level of T10).
ANATOMY OF RLN
The course and length of both RLN differs making the left almost twice as long as the right.
Right RLN =
- loops posteromedially under the origin of the right subclavian artery/brachiocephalic trunk
Left RLN =
- loops posteromedially under the aortic arch (through the aortopulmonary window)
Both of them ascend along the tracheoesophageal groove towards the larynx, however the right RLN only reaches the tracheoesophageal groove at a more distal level (near the cricothyroid joint) because of its more lateral origin and oblique course


![Fig 7: Internal bilateral laryngoceles → left VCP.
64 year-old female with history of smoking and chronic obstructive pulmonary disease is referred to the otorhinolaryngologist because of chronic dysphonia and dysphagia. Laryngoscopic evaluation showed a left vocal cord paralysis and a neck CECT was performed, revealing the presence of bilateral air-filled lesions (more prominent on the left side) located at the level of laryngeal ventricles [a.b.c,d], inside the paraglottic space bounded by the thyroid cartilage [e]. Additionally, we can see signs of left VCP with asymmetric enlargement of both pyriform sinuses, with left side predominance [h] and anteromedial rotation of left arytenoid cartilage and vocal cord displaced medially [g,i] disclosing the “pointing” sign on coronal view [f] and the “sail sign” [*] on axial oblique plane [j].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2021](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939322?maxheight=150&maxwidth=150)
![Fig 8: Left vagus nerve benign tumor → left VCP.
78 year-old male with history of multiple cardiovascular risk factors and allergy to iodinated contrast, presents with 3 weeks of dysphonia. Laryngoscopic examination showed signs of left VCP. Thoracic NECT was performed displaying an elliptical prevascular lesion of soft tissue density [c,d] that connects to a millimetric tubular structure [a,b] that runs superiorly towards the juxta-jugular region and inferiorly towards the inferior margin of the aortic arch where it bifurcates [e,f], probably corresponding to a benign nerve sheath tumor arising from the left CN X (vagal Schwannoma) .
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2015](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939330?maxheight=150&maxwidth=150)
![Fig 9: Cervical osteoarthritis → right VCP.
69 year-old male presents with months of mild dysphonia and globus pharyngeus. Laryngoscopy showed signs of right VCP as well as the cervicothoracic CECT: dilated right ventricle represented by “mushroom sign” in strict axial plane [a] and “sail sign” on oblique axial plane [b], right piriform sinus enlargement [c], medial deviation of right vocal cord [d] and “pointing” on coronal view demonstrating right vocal cord atrophy [e].](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939331?maxheight=150&maxwidth=150)
![Fig 10: Cervical osteoarthritis → right VCP.
Thoracic images revealed severe degenerative changes of the cervical spine, especially at the level of:
- soft palate = affecting the right atlanto-axoid joint in the form of sclerosis, hypertrophy and large osteophytes [a,b] projecting anteriorly with bulging of the airway [a] and occupation of the right parapharyngeal fat [e].
- cricoid ring = affecting the right uncovertebral joint of C5-C6 with an anterior osteophyte[d] that displaces the prevertebral muscles and reduces such space [c].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2020](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939332?maxheight=150&maxwidth=150)
![Fig 11: Esophageal stage IV squamous cell carcinoma → left VCP.
65 year-old male with history of smoking and alcohol abuse, presents with intermittent dysphonia, dysphagia and weight loss. Laryngoscopy showed loss of normal mobility affecting the left vocal cord and the cervicothoracic CECT revealed signs of left VCP: left piriform sinus enlargement [a] and medial deviation and thickening of AEF [b]. Thoracic images depicted a mass occupying the left tracheoesophageal groove [g] that arises from the left wall of cervical esophagus (20 cm below the incisors) [c] with tracheal contact and obliteration of the esophageal lumen [c,g]. The PET-CT showed a large hypermetabolic mass extending from T2 until T4 [d,e,h] and endoscopic images of the tumor with biopsy confirming squamous cell carcinoma [f].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2020](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939329?maxheight=150&maxwidth=150)
![Fig 12: Stage III NSCLC → left VCP.
71 year-old male with history of smoking and asbestos exposure, presents with 5 months of dysphonia with weight loss. Laryngoscopy showed signs of left VCP. Cervico-thoracic CECT was performed revealing a solid pulmonary nodule located in the periphery of left upper lobe [a] and a large mediastinal conglomeration of lymphadenopathies located at the left paratracheal station [d], probably injuring the course of left RLN at the aortopulmonary window [c]. PET-CT showed intense metabolic activity of the solid nodule and adenopathic conglomerate [b,e,f].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2021](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939333?maxheight=150&maxwidth=150)
![Fig 13: Thoracic aorta pseudoaneurysm (Ortner’s syndrome)→ left VCP.
73 year-old male with multiple cardiovascular risk factors and aortic atherosclerosis, presents with abrupt dysphonia and a single episode of bronchoaspiration. Laryngoscopic examination showed shortening of left vocal cord and the cervicothoracic CECT depicted ipsilateral signs of left VCP such as enlargement of pyriform sinus [a] and vocal cord medially displaced [b]. Thoracic images confirmed severe atherosclerotic disease with complete occlusion of left common carotid artery [c] and calcified aortic atheromatosis affecting the aortic arch [d] towards descending aorta with thickened/irregular walls suggesting intramural ulcers and revealing the presence of a pseudoaneurysm at the inferior margin of the aortic arch [e] that projects anterior and caudally generating mil deformity in the anterior margin of the left pulmonary artery [f].](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939324?maxheight=150&maxwidth=150)
![Fig 14: Thoracic aorta pseudoaneurysm (Ortner’s syndrome)→ left VCP.
Volume rendering images displaying the entire thoracic aorta showing calcified atherosclerotic disease with irregular and thickened walls [a]. Image of penetrating atherosclerotic ulcer with pseudoaneurysm at the level of aortopulmonary window, that extends caudally deforming the anterior margin of the left pulmonary artery (which is mildly enlarged) [b].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2020](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939325?maxheight=150&maxwidth=150)
![Fig 15: Ascending aorta saccular aneurysm→ left VCP
71 year-old male with history of atherosclerortic cardiovascular disease and abdominal aortic aneurysm, presents with 1 month dysphonia. Laryngoscopic examination showed left vocal cord paralysis as well as the cervicothoracic CECT that showed dilated left laryngeal ventricle showing the “mushroom sign” [a] on strict axial view and the “sail sign”on oblique axial view [b ], piriform sinus enlargement [c,d] and thickening/medial deviation of aryepiglottic fold [b].
It also confirmed severe calcified atherosclerotic disease affecting carotid bifurcation and left internal carotid artery [e].
Thoracic images revealed the presence of an aneurysm located at the lateral margin of the aortic arch immediately after the origin of the left subclavian artery [c,e], that extends inferiorly at the aortopulmonary window with a saccular morphology [d]. It also demonstrated severe atherosclerosis affecting the entire thoracic aorta with calcified plaques and luminal irregularities specially along the descending aorta [a,b]. Volume rendering sagital image of the aortic arch showing a wide neck aneurysm (9mm) [f].](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939326?maxheight=150&maxwidth=150)
![Fig 16: Ascending aorta saccular aneurysm→ left VCP.
Thoracic images revealed the presence of an aneurysm located at the lateral margin of the aortic arch immediately after the origin of the left subclavian artery [c,e], that extends inferiorly at the aortopulmonary window with a saccular morphology [d].
It also demonstrated severe atherosclerosis affecting the entire thoracic aorta with calcified plaques and luminal irregularities specially along the descending aorta [a,b].
Volume rendering sagital image of the aortic arch showing a wide neck aneurysm (9 mm) [f].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2009](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939327?maxheight=150&maxwidth=150)
![Fig 17: Bilateral medial bullae → right VCP.
57 year-old male with history of smoking presents with mild hoarseness and single episode of choking. Laryngoscopy showed the presence of right VCP with good compensation from contralateral vocal cord, which probably explained the absence of dysphonia. Cervicothoracic CECT was performed showing ipsilateral signs of right VCP such as right vocal cord medially displaced [a], enlargement of pyriform sinus [b,c] and mild dilation of right laryngeal ventricle displaying the mushroom sign [e]. Thoracic CECT revealed paraseptal emphysema [f] with the presence of bilateral large medial bullae [g] that expanded towards the right retrotracheal space producing esophageal extrinsic compression [h], leading to right RLN paralysis.
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2021](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939323?maxheight=150&maxwidth=150)
![Fig 18: Esophageal diverticulum extending towards the aortic arch→ left VCP.
57 year-old female without any history of morbidity, presents with hoarseness and choking episodes without dysphagia. Laryngoscopic examination showed left vocal cord paralysis with compensation from contralateral cord. A cervicothoracic CECT was performed that did not reveal any abnormalities in the glottis, however, it revealed a 10 mm esophageal diverticulum protruding from the left wall of the middle segment of the esophagus (at the level of carina), extending inferiorly towards the inferior margin of the aortic arch (aortopulmonary window) [a,b,c,d,e,f].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2017](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939328?maxheight=150&maxwidth=150)
