Type:
Educational Exhibit
Keywords:
Ear / Nose / Throat, Head and neck, Mediastinum, CT, Localisation, Aneurysms, Neoplasia, Speech disorders
Authors:
A. Micolich Vergara, J. Capellades, F. Zuccarino
DOI:
10.26044/ecr2023/C-17377
Findings and procedure details
DIAGNOSTIC ASESSMENT
Once VCP is suspected, patients must undergo a clinical evaluation of the larynx followed by a thorough head and neck radiological evaluation.
Cross sectional imaging modality of choice is CECT. The study must include the upper mediastinum up to the aortopulmonary window and acquired during quiet respiration so the cords are in an abducted position.
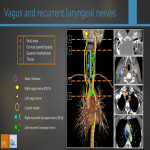
Both the CN X and RLN cannot be directly visualized on CT, therefore, it is imperative for radiologists to recognize their expected courses so we dont miss out on pathologies that may have more significance than the VCP itself .
IMAGING FEATURES OF VCP
VCP can be reliably identified at CT due to characteristic findings although careful evaluation must be carried out by appropriately handling the scan planes of the glottis so we can avoid potential pitfalls and mimics.
The scan planes we must utilize when evaluating the glottis are:
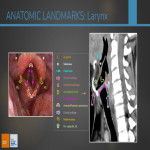
- STRICT AXIAL PLANE = at the level of the anterior and posterior comissures.
- OBLIQUE AXIAL PLANE = at the level of true vocal cords (cricoarytenoid joints)
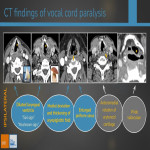
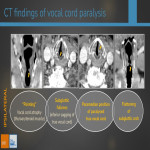
CT signs of VCP are all ipsilateral and the most specific ones are the first three:
- Dilated laryngeal ventricle: due to atrophy of thyroarytenoid muscle.
- “sail sign” (oblique axial plane) = unilateral dilation of laryngeal ventricle + medialisation of posterior margin of true vocal cords
- “mushroom sign” (strict axial plane) = unilateral dilation of laryngeal ventricle + medialisation of posterior margin of true vocal cords + contralateral anterior subglottic air
- Medial deviation and thickening of aryepiglottic fold = due to paralysis of the posterior cricoarytenoid muscle (only abductor muscle).
- Enlarged piriform sinus = due to medial deviation of aryepiglottic fold which forms the medial wall of the piriform sinus.
- Anteromedial rotation of arytenoid cartilage = this causes the affected vocal cord to sag inferiorly.
- Wide valleculae = probably due to the medially deviated aryepiglottic fold that generates some epiglottic displacement.
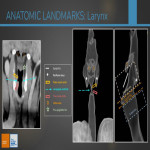
- “Pointing” of the atrophied cord (coronal view) = due to atrophy of thyroarytenoid muscle, the paralysed cord looses its globular medial edge resulting in a sharp medial margin.
- Subglottic fullness = the anteromedial rotation of arytenoid cartilage provokes the inferior sagging of the paralysed cord resulting in fullness of the subglottic area.
- Paramedian position of affected true vocal cord = the less reliable sign because of the multiple positions the cord can take on CT.
- Flattening of subglottic arch (coronal view) = the subglottic arch forms a 90º degrees angle and this angulation is lost on the affected side.
DIFFERENTIAL DIAGNOSIS OF VCP BY LOCATION
LARYNX
- Laryngocele
- Polyps, cysts
- Squamous cell carcinoma
- Papillomatosis
- Amyloidosis
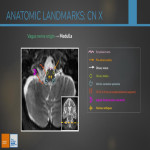
BRAINSTEM
SKULL BASE
- Meningioma
- Metastases
- Glomus jugulare
CAROTID SHEATH
- Glomus vagale
- Schwannoma
- Trauma
- Extrinsic compression: ostheoarthritis
UPPER MEDIASTINUM
- Neoplastic :
- Vascular etiologies:
- Ortner's syndrome
- aortic aneurysm
- Inflammatory
- Miscellaneus:
- medial bullae
- esophageal diverticulum


![Fig 7: Internal bilateral laryngoceles → left VCP.
64 year-old female with history of smoking and chronic obstructive pulmonary disease is referred to the otorhinolaryngologist because of chronic dysphonia and dysphagia. Laryngoscopic evaluation showed a left vocal cord paralysis and a neck CECT was performed, revealing the presence of bilateral air-filled lesions (more prominent on the left side) located at the level of laryngeal ventricles [a.b.c,d], inside the paraglottic space bounded by the thyroid cartilage [e]. Additionally, we can see signs of left VCP with asymmetric enlargement of both pyriform sinuses, with left side predominance [h] and anteromedial rotation of left arytenoid cartilage and vocal cord displaced medially [g,i] disclosing the “pointing” sign on coronal view [f] and the “sail sign” [*] on axial oblique plane [j].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2021](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939322?maxheight=150&maxwidth=150)
![Fig 8: Left vagus nerve benign tumor → left VCP.
78 year-old male with history of multiple cardiovascular risk factors and allergy to iodinated contrast, presents with 3 weeks of dysphonia. Laryngoscopic examination showed signs of left VCP. Thoracic NECT was performed displaying an elliptical prevascular lesion of soft tissue density [c,d] that connects to a millimetric tubular structure [a,b] that runs superiorly towards the juxta-jugular region and inferiorly towards the inferior margin of the aortic arch where it bifurcates [e,f], probably corresponding to a benign nerve sheath tumor arising from the left CN X (vagal Schwannoma) .
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2015](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939330?maxheight=150&maxwidth=150)
![Fig 9: Cervical osteoarthritis → right VCP.
69 year-old male presents with months of mild dysphonia and globus pharyngeus. Laryngoscopy showed signs of right VCP as well as the cervicothoracic CECT: dilated right ventricle represented by “mushroom sign” in strict axial plane [a] and “sail sign” on oblique axial plane [b], right piriform sinus enlargement [c], medial deviation of right vocal cord [d] and “pointing” on coronal view demonstrating right vocal cord atrophy [e].](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939331?maxheight=150&maxwidth=150)
![Fig 10: Cervical osteoarthritis → right VCP.
Thoracic images revealed severe degenerative changes of the cervical spine, especially at the level of:
- soft palate = affecting the right atlanto-axoid joint in the form of sclerosis, hypertrophy and large osteophytes [a,b] projecting anteriorly with bulging of the airway [a] and occupation of the right parapharyngeal fat [e].
- cricoid ring = affecting the right uncovertebral joint of C5-C6 with an anterior osteophyte[d] that displaces the prevertebral muscles and reduces such space [c].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2020](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939332?maxheight=150&maxwidth=150)
![Fig 11: Esophageal stage IV squamous cell carcinoma → left VCP.
65 year-old male with history of smoking and alcohol abuse, presents with intermittent dysphonia, dysphagia and weight loss. Laryngoscopy showed loss of normal mobility affecting the left vocal cord and the cervicothoracic CECT revealed signs of left VCP: left piriform sinus enlargement [a] and medial deviation and thickening of AEF [b]. Thoracic images depicted a mass occupying the left tracheoesophageal groove [g] that arises from the left wall of cervical esophagus (20 cm below the incisors) [c] with tracheal contact and obliteration of the esophageal lumen [c,g]. The PET-CT showed a large hypermetabolic mass extending from T2 until T4 [d,e,h] and endoscopic images of the tumor with biopsy confirming squamous cell carcinoma [f].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2020](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939329?maxheight=150&maxwidth=150)
![Fig 12: Stage III NSCLC → left VCP.
71 year-old male with history of smoking and asbestos exposure, presents with 5 months of dysphonia with weight loss. Laryngoscopy showed signs of left VCP. Cervico-thoracic CECT was performed revealing a solid pulmonary nodule located in the periphery of left upper lobe [a] and a large mediastinal conglomeration of lymphadenopathies located at the left paratracheal station [d], probably injuring the course of left RLN at the aortopulmonary window [c]. PET-CT showed intense metabolic activity of the solid nodule and adenopathic conglomerate [b,e,f].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2021](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939333?maxheight=150&maxwidth=150)
![Fig 13: Thoracic aorta pseudoaneurysm (Ortner’s syndrome)→ left VCP.
73 year-old male with multiple cardiovascular risk factors and aortic atherosclerosis, presents with abrupt dysphonia and a single episode of bronchoaspiration. Laryngoscopic examination showed shortening of left vocal cord and the cervicothoracic CECT depicted ipsilateral signs of left VCP such as enlargement of pyriform sinus [a] and vocal cord medially displaced [b]. Thoracic images confirmed severe atherosclerotic disease with complete occlusion of left common carotid artery [c] and calcified aortic atheromatosis affecting the aortic arch [d] towards descending aorta with thickened/irregular walls suggesting intramural ulcers and revealing the presence of a pseudoaneurysm at the inferior margin of the aortic arch [e] that projects anterior and caudally generating mil deformity in the anterior margin of the left pulmonary artery [f].](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939324?maxheight=150&maxwidth=150)
![Fig 14: Thoracic aorta pseudoaneurysm (Ortner’s syndrome)→ left VCP.
Volume rendering images displaying the entire thoracic aorta showing calcified atherosclerotic disease with irregular and thickened walls [a]. Image of penetrating atherosclerotic ulcer with pseudoaneurysm at the level of aortopulmonary window, that extends caudally deforming the anterior margin of the left pulmonary artery (which is mildly enlarged) [b].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2020](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939325?maxheight=150&maxwidth=150)
![Fig 15: Ascending aorta saccular aneurysm→ left VCP
71 year-old male with history of atherosclerortic cardiovascular disease and abdominal aortic aneurysm, presents with 1 month dysphonia. Laryngoscopic examination showed left vocal cord paralysis as well as the cervicothoracic CECT that showed dilated left laryngeal ventricle showing the “mushroom sign” [a] on strict axial view and the “sail sign”on oblique axial view [b ], piriform sinus enlargement [c,d] and thickening/medial deviation of aryepiglottic fold [b].
It also confirmed severe calcified atherosclerotic disease affecting carotid bifurcation and left internal carotid artery [e].
Thoracic images revealed the presence of an aneurysm located at the lateral margin of the aortic arch immediately after the origin of the left subclavian artery [c,e], that extends inferiorly at the aortopulmonary window with a saccular morphology [d]. It also demonstrated severe atherosclerosis affecting the entire thoracic aorta with calcified plaques and luminal irregularities specially along the descending aorta [a,b]. Volume rendering sagital image of the aortic arch showing a wide neck aneurysm (9mm) [f].](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939326?maxheight=150&maxwidth=150)
![Fig 16: Ascending aorta saccular aneurysm→ left VCP.
Thoracic images revealed the presence of an aneurysm located at the lateral margin of the aortic arch immediately after the origin of the left subclavian artery [c,e], that extends inferiorly at the aortopulmonary window with a saccular morphology [d].
It also demonstrated severe atherosclerosis affecting the entire thoracic aorta with calcified plaques and luminal irregularities specially along the descending aorta [a,b].
Volume rendering sagital image of the aortic arch showing a wide neck aneurysm (9 mm) [f].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2009](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939327?maxheight=150&maxwidth=150)
![Fig 17: Bilateral medial bullae → right VCP.
57 year-old male with history of smoking presents with mild hoarseness and single episode of choking. Laryngoscopy showed the presence of right VCP with good compensation from contralateral vocal cord, which probably explained the absence of dysphonia. Cervicothoracic CECT was performed showing ipsilateral signs of right VCP such as right vocal cord medially displaced [a], enlargement of pyriform sinus [b,c] and mild dilation of right laryngeal ventricle displaying the mushroom sign [e]. Thoracic CECT revealed paraseptal emphysema [f] with the presence of bilateral large medial bullae [g] that expanded towards the right retrotracheal space producing esophageal extrinsic compression [h], leading to right RLN paralysis.
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2021](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939323?maxheight=150&maxwidth=150)
![Fig 18: Esophageal diverticulum extending towards the aortic arch→ left VCP.
57 year-old female without any history of morbidity, presents with hoarseness and choking episodes without dysphagia. Laryngoscopic examination showed left vocal cord paralysis with compensation from contralateral cord. A cervicothoracic CECT was performed that did not reveal any abnormalities in the glottis, however, it revealed a 10 mm esophageal diverticulum protruding from the left wall of the middle segment of the esophagus (at the level of carina), extending inferiorly towards the inferior margin of the aortic arch (aortopulmonary window) [a,b,c,d,e,f].
Origin: Department of Radiology, Hospital del Mar – Parc de Salut Mar, Barcelona, Spain/2017](https://epos.myesr.org/posterimage/esr/ecr2023/162009/media/939328?maxheight=150&maxwidth=150)