A. Types of HNSCC surgeries
- Types of glossectomies [Figure 1]
- Partial glossectomy: Lesion along with adjacent normal mucosa, submucosa, and intrinsic muscles up to the surface of the extrinsic muscles ipsilateral to the lesion, are removed. [1]
- Hemiglossectomy: Mucosa, submucosa, intrinsic, and extrinsic muscles ipsilateral to the lesion are removed with preserved base of tongue. [1]
- Compartmental hemiglossectomy: Mucosa, submucosa, intrinsic and extrinsic muscles ipsilateral to the lesion, genioglossus, hyoglossus and styloglossus muscles, and the inferior portion of the palatoglossus muscle are removed along with midline raphe. [1]
- Subtotal glossectomy: Base of the tongue is preserved on both sides, rest removed. [1]
- Near-total glossectomy: Ipsilateral base of tongue is also removed along with other structures. [1]
- Total glossectomy: Entire mobile tongue along with base is removed. [1]
- Types of mandibulectomies [Figure 2]
- Marginal mandibulectomy: Rim of mandible is removed with preserved medullary and mandibular continuity. Prerequisite for performing this surgery is that preserved height of mandible free of paramandibular soft tissue should be more than 1 cm and there should be no/only superficial mandibular cortical erosions. [2,3]
- Segmental mandibulectomy: Performed when mandibular canal is involved and criteria for marginal mandibulectomy are not met. It is also performed in edentulous patients with inadequate mandibular height.[2,3]
- Hemimandibulectomy: Performed when one half of mandible is extensively involved.
- Types of maxillectomies [Figure 3]
- Total maxillectomy: Removal of complete maxilla. [4]
- Partial maxillectomy: Could be infrastructure, suprastructure, medial, or subtotal, depending upon the structures removed. [4]
- Types of laryngectomies
- Total laryngectomy with creation of neopharynx [Figure 4]: Removal of complete larynx with repair of the resultant pharyngeal defect known as “neopharynx”. [5] Neopharynx on CT scan shows inner hyperdense enhancing layer of mucosa, middle hypodense layer of submucosa and outer isodense layer of pharyngeal constrictor muscle, formed by the free flap. [6]
- Partial laryngectomy: Part of larynx is removed.
5. Types of flap reconstructions
Flaps are used for covering surgical defect.
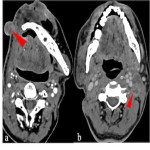
- Myocutaneous flap [Figure 5]: Regional flap with preserved vasculature, initially shows muscle density/intensity on CT/MRI respectively, eventually undergoes denervation atrophy resulting in volume loss and fatty replacement with fat density/signal intensity on CT/MRI respectively. Sharp boundaries between flap and adjacent normal structures, distinguishes it from a recurrent mass. Myocutaneous flaps may show moderate to intense enhancement, or no enhancement. [7- 11]
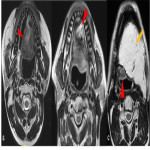
- Free flap [Figure 6]: Here host tissue away from the primary tumour site is used to cover the surgical defect and the donor vessel is anastomosed with the recipient vessel. Jejunal free flap, used for neopharynx, may develop reactive lymphadenopathy due to environmental changes post-surgery, and should not be confused with metastatic lymphadenopathy. Fibular free flap reconstruction used after segmental reconstruction, can undergo ossification of periosteal vascular pedicle within one month. [10-13]
6. Types of neck dissection [Figure 7]
Soft tissue density/intensity may be seen encircling the carotid sheath after neck dissection due to fibrosis and scar. Depending upon the structures and level of nodes removed, neck dissection could be radical, modified radical, selective, and extended. [10, 11, 14, 15]
B. Expected changes after RT/CRT
- Early changes (< 2 weeks to 3 months) [Figure 8]
These include subcutaneous fat stranding and reticulations, pharyngeal and laryngeal oedema, enlarged and intensely enhancing submandibular and parotid glands, and oedematous and heterogeneously enhancing thyroid gland. [10, 11, 16]
- Delayed changes (> 90 days) [Figure 9]
These include thickening of skin and platysma muscles, atrophy of salivary glands and thyroid gland. [10, 11, 16]
C.Complications after surgery and RT/CRT
Post operative complications [Figure 10]
- Seroma: Non-enhancing fluid collection.
- Abscess: Rim enhancing fluid collection showing diffusion restriction on MRI.
- Haematoma: Appears hyperdense on CT, hyperintense on T1 and shows mixed signal on T2 depending upon the stage of haematoma.
- Fistula: Direct visualization of fistulous track communicating between the oral cavity/larynx and cutis, or oral cavity and paranasal sinus.
- Flap necrosis: Can occur due to arterial or venous thrombosis, or infection. Arterial or venous thrombosis shows filling defect on doppler, CT/MR angiography with non-enhancement of flap. Rim enhancing collections with air locules at the flap/surgical site suggests infection.
- Complications specific to neck dissection: Chylous fistula, with level IV neck dissection, suspected when collections are located predominantly in left lower neck on imaging.
Post RT/CRT complications
- Mucosal necrosis: Occurs between 6-12 months. Absence of mucosal enhancement on CT and MRI with/without ulceration. [11]
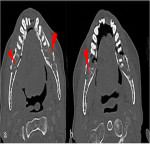
- Osteoradionecrosis (ORN) [Figure 11]: Occurs between 1-3 years. Mandible is most commonly affected, incidence has reduced due to intensity modulated RT (IMRT) technique, but not nullified. [11] On CT, ORN appears as patchy lytic areas, disorganized sclerosis, cortical destruction, pathological fracture, loss of trabecular pattern, with/without fistulization to the skin [10, 11, 16] On MRI, a new abnormal marrow signal intensity, cortical destruction without any soft tissue component, diffuse, intense enhancement of the abnormal marrow is suggestive of ORN. [10, 11]
- Chondroradionecrosis (CRN): Occurs between 1-10 years. Fragmented, collapsed thyroid cartilage with/without presence of gas bubbles on CT. [10] Effusion in cricoarytenoid joint leading to anterior dislocation of arytenoid cartilage, eventually increasing lysis leading to its disappearance. [10] Sclerosis of the cricoid cartilage may be seen. [10] Post contrast enhancement and loss of high medullary signal on TWI within the ossified cartilage is suggestive of CRN on MRI. [16]
- Vascular complications: Occurs between 4 months to 20 years. Internal jugular vein thrombosis can occur, seen as filling defect on CT/MR angiography or directly visualised on colour doppler. Mural thickening of carotid artery suggestive of atherosclerosis may be seen. [11]
- Radiation induced lung damage: Radiation pneumonitis is seen as focal ground glass densities, with or without consolidation on CT, occurs within 1-3 months. [11] Radiation fibrosis manifests as a well demarcated area of volume loss, linear scarring , and traction bronchiectasis on CT, occurs within 6-12 months. [17]
- Radiation induced neoplasm: It is defined as a tumour with a different histology occurring within an irradiated field at a site away from the original tumour after a latency period of 5 years or more. [16, 18] Imaging findings depend upon the new malignancy that has developed.
D.Post NACT response assessment on imaging
Response Evaluation Criteria In Solid Tumours (RECIST 1.1), though has limitations, is still used for assessing response after NACT [Figure 12]. [19]
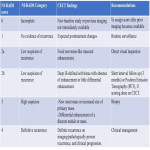
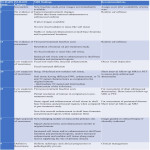
E. Reporting of posttreatment findings using NI-RADS
American College of Radiology (ACR) has devised NI-RADS template for reporting posttreatment findings based on the level of suspicion of recurrence. [20] NI-RADS templates are separate for primary site and neck (for lymph nodal assessment). CT and MRI NI-RADS template for the primary site are shown in figures 13 and 14 respectively (adapted from ACR). NI-RADS for neck is shown in figure 15 (adapted from ACR).
Posttreatment cases and their NI-RADS categories on imaging are shown in figures 16 and 17.


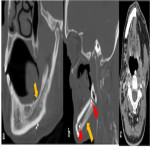
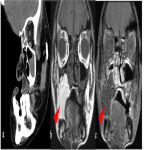
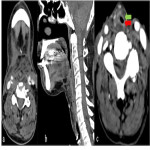
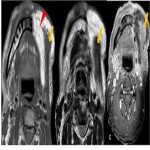
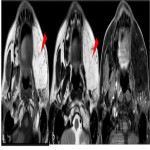
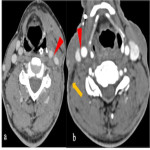
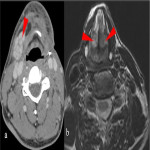
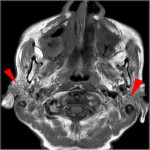
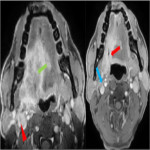
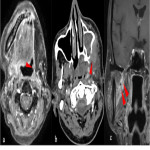
![Fig 10: Figure 10: Post operative complications. Axial (a) and Coronal (b) CECT 8 weeks post treatment in a post-operative case of left lower alveolus shows rim enhancing collection at the operative bed (arrowhead) with presence of air locule (red arrow) suggestive of abscess. In addition, two fistulae are seen, one between the oral cavity and skin (orocutaneous fistula) [green arrow] and another between oral cavity and left maxillary sinus antrum (oroantral fistula) [blue arrow]
References: © Dr. Nivedita Chakrabarty, Department of Radiodiagnosis, Tata Memorial Hospital, Tata Memorial Centre, Mumbai, India.](https://epos.myesr.org/posterimage/esr/ecr2023/162973/media/936490?maxheight=150&maxwidth=150)