Extrapulmonary tuberculosis (TB) constitutes 15-20% of all TB cases. In the past years, the incidence has increased, particularly in patients with immune system disorders (AIDS, patients receiving chemotherapy, etc.) and those in other high-risk groups including people with diabetes.
Extrapulmonary TB can be challenging to diagnose as it can mimic many other diseases, so a biopsy is often required. It is important to be aware of the imaging findings, especially in high-risk patients, so we can find an early diagnosis and reduce complications.
LYMPHATIC TB
Lymphatic TB is the most frequent extrapulmonary manifestation.
Cervical adenitis is the most common, and it is usually caused by lymphatic spread from mediastinal adenopathy. In children, it can be acquired by direct spread from bacilli in the oropharyngeal mucosa.
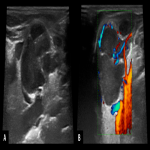
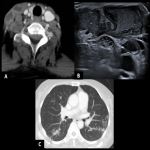
Tuberculous adenitis usually consists in multiple necrotic lymph nodes that can evolve into necrotic masses, so at imaging, we usually find multispatial enlarged lymph nodes with thick, irregular peripheral enhancement and loss of fat planes.
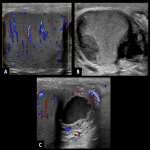
Differential diagnoses of TB cervical adenitis include metastatic necrotic lymph nodes. Imaging Doppler Ultrasound (US) features suggestive of TB are peripheral displacement of the vessels by central areas of necrosis, the persistence of central hilar vascularity, and low intranodal vascular resistance.
CENTRAL NERVOUS SYSTEM (CNS) TB
- Tuberculous Lemptomeningitis
Tuberculous leptomeningitis is the most common form of TB affecting CNS. It most commonly manifests as subacute or chronic meningitis.
The most specific imaging finding is a basal meningeal enhancement, best seen in MRI, although it can also affect the superficial sulci, the ventricle surface, and the choroid plexus.
Some typical complications are:
-communicating hydrocephalus due to the high-viscosity exudates
-brain infarctions caused by vasculitis changes of the lenticulostriate and thalamoperforating arteries
-cranial nerve involvement
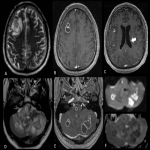
Tuberculomas are the most common parenchymal brain manifestation. They are usually caused by hematogenous spread or by extension of a CSF infection.
They can be divided into three types:
- Non-caseating tuberculomas: solid without necrosis. They appear as round lesions in the subcortical white matter, hypointense on T1, and hyperintense on T2-weighted imaging, and show a homogenous enhancement. They are usually surrounded by mild vasogenic edema.
- Solid caseating tuberculomas: they have a central caseating zone of necrosis with an external collagenous capsule. They are hypo- or isointense on T1-weighted imaging and slightly hypointense on T2-weighted imaging. They show a ring enhancement at contrast-enhanced imaging.
- Tuberculomas with central liquefaction of caseous material: indistinguishable from other infectious abscesses. At MRI, the caseous center is hypointense on T1 and hyperintense on T2- weighted imaging and they show peripheral contrast enhancement and restricted diffusion.
GENITOURINARY TB
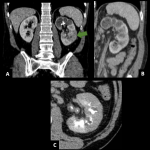
Renal TB is more frequently unilateral.
The bacilli reach the kidneys through hematogenous spread. They form granulomas in the periglomerular capillaries and during a breakdown in immunity, granulomas grow and enter the glomerular system.
The earliest imaging findings are erosion in the minor calyces and papillary necrosis causing a "moth-eaten" appearance. Asymmetric caliectasias caused by necrosis and fibrosis can be seen in more advanced stages. Focal calcification is the most common finding on CT imaging. In terminal stages, we can find a non-functioning kidney with extensive calcifications, known as “mastic kidney”. Cortical granulomas can also be seen as solid hypoenhancing masses.
Ureteral manifestations appear after a kidney infection, with thickened urothelial walls and sometimes focal filling defects that represent debris.
Genital TB is rare in males, and it is more frequent in association with renal TB.
The prostate and epididymis are the most frequent sites affected.
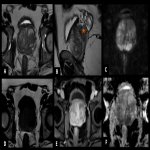
Prostatic TB is usually asymptomatic and incidentally diagnosed with a biopsy performed to rule out malignancy. Hematogenous spread is the most frequent mechanism. TB prostatitis shows an irregular peripheral zone with hypoechoic areas on US and linear areas of hypointensity on T2-weighted imaging MRI. The main findings are prostatic abscesses that appear as hypointense with peripheral enhancement and restricted diffusion.
Epididymal TB can occur secondary to renal TB or by hematogenous spread from prostatic infection. It cannot be differentiated from other bacterial infections. US shows a heterogenous and enlarged epididymis. Tuberculous abscesses can also be formed.
Genital TB in females is infrequent. Early diagnosis is crucial because it is an important cause of infertility.
Bilateral Fallopian tube involvement is the most common.
Imaging findings are usually tubal stenosis, fallopian tube nodular scarring, and hydrosalpinx or pyosalpinx. Irregular calcifications in the adnexal area also can be present.
ABDOMINAL TB
Although intestinal TB is rare, it is a common abdominal manifestation.
The bacilli infect the gastrointestinal tract after the ingestion of respiratory secretions. The bacteria infect the submucosal lymphoid tissue producing granulomas that can ulcerate.
The terminal ileum and ileocecal region are the most common sites affected.
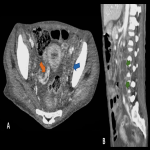
CT usually shows asymmetric wall thickening of the terminal ileum, cecum, or ileocecal region with necrotic lymph nodes. After chronic inflammation, they may appear small and irregular due to fibrosis.
It must be differentiated from Crohn's disease. Imaging findings suggestive of TB are involvement of the ileum rather than the cecum, absence of skip lesions, and wall thickening without mural stratification. Also, increased mesenteric vascularity is more common in Crohn's disease.
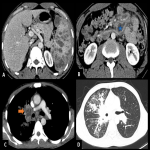
Abdominal solid-organ TB most frequently affects the spleen and liver. It usually affects immunocompromised patients, and it is caused by hematogenous spread.
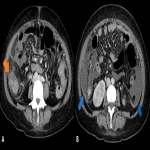
CT usually shows a micronodular manifestation with multiple hypoattenuating nodules throughout the parenchyma. Sometimes hepatosplenomegaly is the only manifestation. Differential diagnoses include fungal infection, lymphoma, or metastases.
Sometimes a focal hepatic pattern can be seen, with large nodules with central necrosis, making it difficult to differentiate from abscesses of other etiologies.
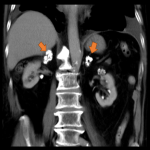
TB infection in the adrenal glands is rare and usually bilateral. In the early stages, the glands are enlarged with necrotic changes. At advanced stages, they appear atrophic with calcifications.
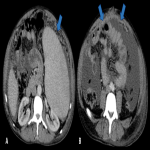
Peritoneal TB occurs associated with other forms of abdominal TB.
Ascites is the most common imaging finding.
- Wet type: exudative high attenuation ascites due to high protein and cellular content.
- Dry type: fibrous adhesions and thickened, "cake-like" omentum with a carcinomatosis appearance.
- Fibrotic type: fixed bowel loops and loculated ascites.
MUSCULOSKELETAL TB
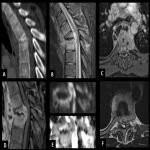
- Tuberculous spondylitis (Pott's disease)
It represents half of the musculoskeletal TB cases. The bacilli reach the spine through the hematogenous spread, infecting the anterior portion of the vertebral bodies.
It usually affects the thoracic spine. Due to the slow inflammatory response, they usually spread to contiguous or distant vertebral bodies. The intervertebral disks are preserved initially due to mycobacteria's lack of proteolytic enzymes. Vertebral body destruction begins in the anterior portion of the plates, leading to focal kyphosis. It usually spreads to the paraspinal space forming cold abscesses with thin and smooth walls and mild perilesional edema.
A differential diagnosis of pyogenic infection must be done. Pyogenic spondylitis is more often localized at the lumbar spine and usually affects less than two vertebral levels, and it causes vertebral body and intervertebral disk destruction rapidly with extensive edema. Paraspinal abscesses have thicker irregular walls.
It is usually monoarticular and most frequently affects the knee or hip. It is usually secondary to osteomyelitis or hematogenous spread.
In the beginning, it causes thickening of the synovial membrane and reactive joint effusion. Later the granulomatous lesions cause bone erosions. Cartilage destruction is a late finding. Joint effusion at T2-weighted images may have an intermediate signal intensity because of debris and caseation necrosis.
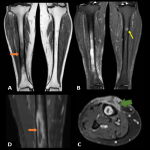
- Tuberculous osteomyelitis
TB osteomyelitis is usually unifocal, but multifocal involvement is seen in children. The femur, tibia, and small bones of the hands and feet are more commonly affected.
The bacilli enter the metaphyses by hematogenous spread.
Imaging findings are nonspecific. Bone marrow edema and intraosseous abscesses can be seen at MRI.
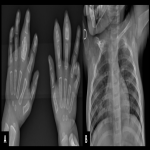
Tuberculous dactylitis is a rare skeletal manifestation of TB where the short tubular bones of the hands and feet are affected.
It typically affects children. In children multiple or consecutive bones are involved, compared to a single bone in adults.
At radiography, these lesions demonstrate soft-tissue swelling and periostitis. These findings are followed by gradual bone destruction and sequestrum formation. Expansion of the bone with cystic changes is known as spina ventosa.