Type:
Educational Exhibit
Keywords:
Cardiac, MR, Education, Pathology
Authors:
C. Urtasun Iriarte, M. B. Barrio Piqueras, A. Ezponda Casajús, M. Jiménez Vázquez, C. Mbongo, N. Cherrez, P. Del Nido Recio, M. R. López de la Torre Carretero, G. Bastarrika Alemañ
DOI:
10.26044/ecr2023/C-18966
Findings and procedure details
A. DIAGNOSIS AND RECOMMENDATIONS
Once the clinical scenario of a TpNOCA appears, the first thing to do is to reconsider the clinical context and exclude alternative diagnoses (i.e. sepsis, pulmonary embolism and stroke among other non-cardiac entities that increase troponins). The next step is to exclude a missed obstruction or another non-ischemic myocardial injury mechanism. Finally, as a diagnosis of exclusion, we call it MINOCA, so it is necessary to go further and try to clarify the aetiology [1,4].
- (Level 1A recommendation) – Coronary CT angiography (CCTA) as an alternative to ICA to exclude ACS when there is a low-to-intermediate likelihood of coronary artery disease and when cardiac troponins and/or ECG are normal or inconclusive [4].
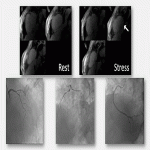
- (Level 1B recommendation) – Non-invasive stress imaging test (stress-CMR or stress-CT) or CCTA before deciding on an invasive approach, in patients with no recurrence of chest pain, normal ECG, and normal cardiac troponin levels, but still with suspected ACS [4].
- (Level 1B recommendation) – Perform CMR on every MINOCA patient without an obvious underlying cause [4].
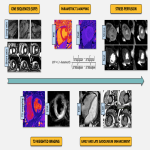
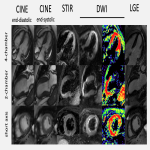
B. STANDARD CMR PROTOCOL
CMR is a non-invasive, safe and helpful imaging technique that plays a key role in identifying/excluding the conditions responsible for the MINOCA. A standard CMR protocol [5] must include the following:
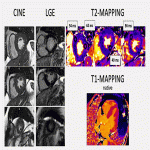
- Steady-State Free Precession (SSFP) CINE sequences: evaluation of global cardiac function and regional wall motion.
- T2-weighted imaging: STIR and T2 mapping. Main role in detecting myocardial oedema and intramyocardial haemorrhage post-acute myocardial infarction.
-
- DWI/ADC: not routinely used (usually for research) but sensitive for identifying oedema.
-
- T2*: imaging useful to detect intramyocardial haemorrhage.
- Parametric T1 mapping (native and post-contrast): for objective and quantitative tissue characterisation and extracellular volume (ECV) calculation [6].
- Early and late gadolinium enhancement sequences (EGE and LGE, respectively): assessment of intracavitary thrombus, microvascular obstruction, and myocardial tissue characterization (infarction and scar).
- Extra: Stress myocardial perfusion: assessment of ischemic myocardial tissue.
C. CORONARY DISORDERS: MINOCA
MINOCA’s prevalence ranges from 5% to 6% among ACS patients with acute myocardial infarction. A higher incidence has been observed in women, young age, and Asian population [1,3,4].
MINOCA encompasses a group of heterogeneous ischemic-related coronary entities [3,7]:
Arteriosclerotic
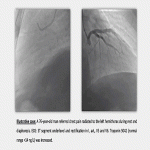
- Coronary plaque disruption: must be suspected in patients with known coronary disease and unstable plaques.
-
- Pearls: Cardiac-CT angiography (1A recommendation) should be performed in patients experiencing ACS with intermediate-risk and no known coronary artery disease after negative or inconclusive evaluation [1,4].
Non-arteriosclerotic
- Coronary artery vasospasm (CAVS; Prinzmetal’s angina): transient narrowing of the coronary arteries that can reduce blood flow to the heart.
-
- Pearls: precipitating factors are drugs (adrenaline, sumatriptan, cocaine, amphetamines) and environmental factors (cold water, hyperventilation).
- Coronary artery dissection: involves a tear in the inner layer of a coronary artery.
-
- Pearls: most frequently seen in middle-aged women, postpartum and with fibromuscular dysplasia.
- Coronary thrombosis/embolism: may present with epicardial and microvascular damage.
-
- Pearls: Patients with a high pretest probability, such as the presence of prosthetic heart valves, atrial fibrillation, endocarditis or blood dyscrasias, are highly suspicious.
- Coronary microvascular disorder (CMD): secondary to damage to the small blood vessels that branch off the main coronary arteries (coronary microvasculature).
-
- Pearls: Coronary reactivity testing (i.e. stress CRM) is required for diagnosis, most often detected as reduced coronary flow reserve (CFR). Diabetes, hypertension, smoking and autoimmune diseases are among the conditions that increase a patient's risk [8].
- Myocardial oxygen demand-supply imbalance: can also cause infarctions (bradyarrhythmias, severe hypoxia or anaemia).
D. MYOCARDIAL INJURIES: MINOCA “MIMICS”
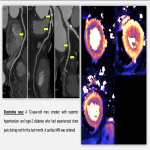
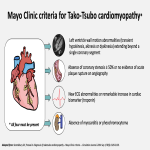
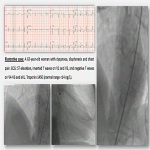
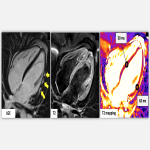
- Stress cardiomyopathy (Tako-Tsubo syndrome; TTS): it is an acute form of reversible and transient systolic failure. Scientific evidence suggests that the pathophysiology involves a sympathetic overstimulation secondary to an excessive release of catecholamines (i.e. a strong emotional event) [9,10]. Diagnosis: Mayo Clinic Criteria.
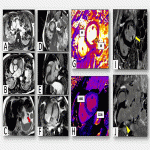
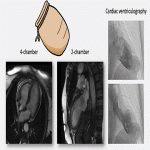
The most characteristic CMR features include:
-
- In its typical form (75% cases): Hypo/akinesia of apical segments (apical ballooning pattern) with compensatory hyperkinesia of basal segments.
-
- Myocardial oedema of meso/subepicardial distribution within the affected regions.
-
- Typically, absence of LGE.
-
- Pearl: highlight EGE sequence for ruling out intracavitary thrombus that can form secondary to contractile dysfunction.
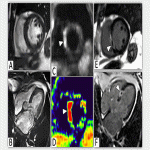
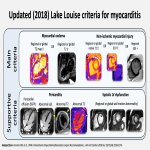
- Acute myocarditis: an inflammation of the myocardium most frequently caused by viral infections [11]. Diagnosis: Lake Louise criteria 2018.
The most characteristic CMR features include:
-
- Left ventricle wall motion abnormalities are common but not specific.
-
- Myocardial oedema with a subepicardial distribution (increased T1 and T2 values on parametric mapping).
-
- Subepicardial LGE is unrestrained to coronary segments.
-
- Pearl: Lateral wall involvement on LGE and mapping sequences is highly suspicious of this entity.
- Others: dilated cardiomyopathy, hypertrophic myocardiopathy, and infiltrative cardiomyopathy.
E. EXTRACARDIAC PATHOLOGIES:
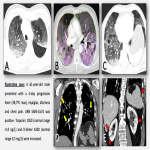
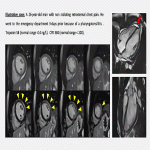
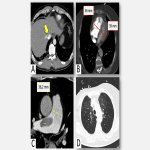
- Pulmonary thromboembolism (PE): CT-Pulmonary angiography (CTPA) is the modality of choice for diagnosing PE in patients with moderate-high risk [12]. Troponin levels are increased in 30-50% of patients experiencing a moderate to large pulmonary embolism, being a marker of right ventricular dysfunction and, therefore, linked to a worse clinical outcome. Lung scintigraphy (ventilation/perfusion scan) is mostly performed when CTPA is contraindicated or inconclusive [12].
-
- Pearls: Do not forget to assess for right ventricular overload and other complications (infarct, pulmonary haemorrhage, and pulmonary hypertension).
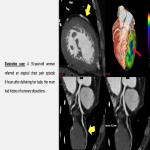
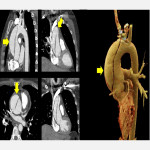
- Aortic dissection: Stanford A-type aortic dissection affects the proximal segment of the ascending aorta. Due to retrograde extension to the aortic root, the coronary ostia can be compromised, leading to ischemia, elevated troponin levels and, eventually, myocardial infarction. CT aortography is usually the modality of choice.
-
- Pearl: CT angiography should be synchronized with the ECG to avoid misinterpretation of artifacts.