Ossicles are just tiny bones; the term may point to any small bone throughout the body,
i.e.
the auditory ossicles,
or the ossicles of the hands and feet.
In the ankle and foot,
ossicles appear as either accessory centers of ossification,
or sesamoids.
Apart from the os tibiale externum,
which is usually called by its English name — the accessory navicular bone — ossicles are referred to by their Latin names.
On MR,
ossicles generally have a fatty signal.
Accessory centers of ossification are variant centers of ossification,
associated with (and called after) a parent bone,
to which they may or may not fuse during adolescence.
In the latter case,
a synchondrosis (or,
less frequently,
a syndesmosis) usually exists.
All of these variant ossification centers may be bilaterally asymmetric.
In a Turkish study of 984 subjects,
accessory ossicles were found in 21,2 % of the population.
The most common were the accessory navicular bone (11,7 %),
the os peroneum (4,7 %),
os trigonum (2,3 %),
os supranaviculare (1,6 %),
os vesalianum (0,4%),
os supratalare (0,2 %), and the os intermetatarseum (0,2 %).
1.
THE OS TRIGONUM AND STIEDA PROCESS
The flexor hallucis longus tendon descends between the medial and lateral tubercles of the posterior talar process.
The ossification center for the lateral tubercle develops at 7 to 13 years of age and fuses with the talar body within one year.
In some instances,
the lateral tubercle (or trigonal process) remains unfused,
and is termed an os trigonum.
In other cases,
the lateral tubercle is hypertrophic and unusually long,
and is called a Stieda process.
In a larger sense,
the os trigonum can also refer to a chronic fracture through the lateral tubercle or Stieda process.
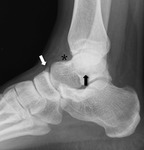
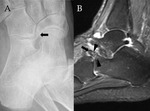
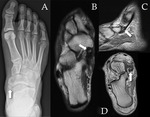
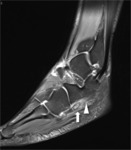
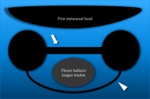
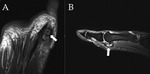
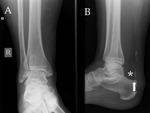
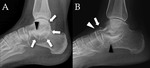
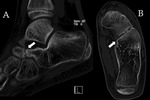
Stoller defines four anatomic variations of the posterolateral talus:
- type 1 is the normal lateral tubercle;
- type 2 is a Stieda process (Fig. 1);
- type 3 is the os trigonum,
as an entirely independent ossicle;
- type 4 is the os trigonum,
fused with the talus via a synchondrosis or,
less commonly,
a syndesmosis.
Shepherd fracture,
named after the Canadian surgeon Francis John Shepherd,
is a fracture of the trigonal or Stieda process.
These fractures occur in the setting of an acute,
blunt trauma,
or in the context of os trigonum syndrome (see further down).
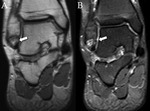
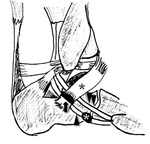
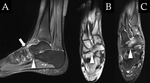
Acute or repetitive compression of the posterior structures of the ankle is generally categorized as posterior ankle impingement syndrome,
Haglund syndrome,
or posteromedial ankle impingement syndrome.
Variations in posterior ankle osseous and soft tissue anatomy contribute to posterior ankle impingement syndrome and Haglund syndromes.
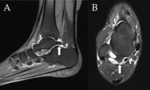
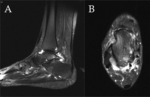
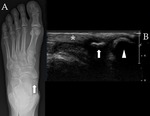
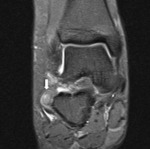
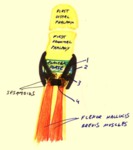
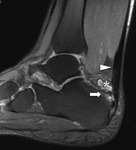
The presence of an os trigonum or a Stieda process is classically associated with posterior ankle impingement syndrome,
which,
in the former case,
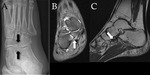
is then referred to as os trigonum syndrome (Fig. 2).
Other possible causes of posterior ankle impingement syndrome are: scarring of a posterior ligamentous tear,
posterior synovial cysts or synovitis,
loose bodies in the posterior joint recess,
and periarticular calcifications.
Posterior ankle impingement syndrome limits ankle plantarflexion and causes posterior ankle pain.
It is frequently seen in ballet dancers,
soccer and football players,
downhill runners,
and other athletes who actively plantar flex their feet.
Furthermore,
as a result of posterior impingement,
acute or stress fractures of the os trigonum or Stieda process may arise,
as well as disruption of the synchondrosis between os trigonum and talus.
Tenosynovitis of the flexor hallucis longus tendon may be another manifestation of os trigonum syndrome.
Be aware that fluid in the flexor hallucis longus tendon sheath may be a sign of tenosynovitis that is unrelated to os trigonum syndrome,
or even be a normal finding,
as the tendon sheath communicates with the tibiotalar joint in 20% of the population.
Longstanding os trigonum syndrome can lead to degenerative changes along the synchondrosis,
with subchondral sclerosis,
subchondral cysts,
and bone remodeling.
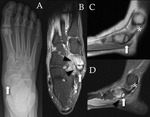
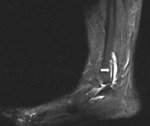
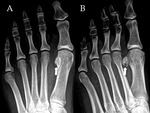
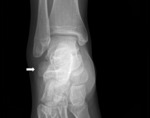
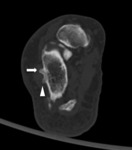
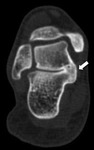
CT
CT is the first choice modality for differentiating between anatomic variations of the posterolateral talus and potential fractures.
Acute fractures have nonsclerotic,
irregular margins.
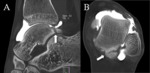
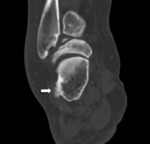
CT is also superior in demonstrating degenerative changes in chronic os trigonum syndrome (Fig. 3).
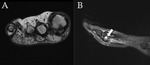
MR
Thick,
irregular,
heterogeneous material posterior to the ankle joint on MR imaging is suggestive of posterior ankle impingement syndrome.
MR can show fluid inside the synchondrosis,
frank disruption of the synchondrosis (with displacement of the os trigonum),
degenerative changes at the synchondrosis,
edema of the posterolateral talus and/or surrounding soft tissues,
synovitis,
capsular thickening and loose bodies in the posterior subtalar joint,
tenosynovitis of the flexor hallucis longus tendon,
and evaluate the ligamentous structures involved in posterior impingement syndrome.
Chronic,
degenerative changes can be seen as subchondral cysts on T2- and T1-weighted images and subchondral sclerosis on T1-weighted images.
A Haglund deformity is the osseous predisposing factor in Haglund's syndrome.
This syndrome wil be discussed further down in section 10.
Posteromedial ankle impingement syndrome has no defined predisposing anatomical variants but typically follows an inversion-supination injury,
with compression of the posterior tibiotalar ligament between the medial malleolus and the talus.
2.
THE OS SUPRANAVICULARE
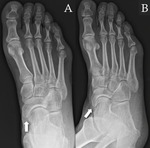
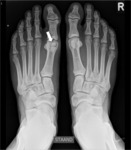
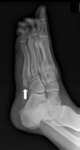
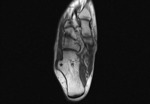
The os supranaviculare (Fig. 4),
also referred to as os talonaviculare dorsale or Pirie bone,
is a round and well-corticated accessory center of ossification located at the proximal dorsal cortex of the navicular bone at its midpoint.
The os supranaviculare has a prevalence of approximately 1 %.
If it becomes become symptomatic,
the main diagnostic objective is to differentiate the os supranaviculare from a cortical avulsion fracture of the navicular bone or the talus.
This avulsion can occur when extensive plantar flexion of the ankle joint causes a separation of the talonavicular joint and a hyperextension of the dorsal talonavicular ligament.
This leads to detachment of a bone flake from the dorsum of the talar head.
Ingalls and colleagues suggested that the presence of an os supranaviculare is a predisposing factor for navicular stress fractures.
They hypothesized that a dorsal cortical notch on the navicular bone,
frequently accompanying an os supranaviculare,
may contribute to the development of navicular stress fractures in the hypovascular central third of the navicular bone.
The os supranaviculare is easily detected on lateral ankle radiographs or sagittal MR or CT images.
We didn’t find radiologic literature describing the imaging characteristics of a symptomatic os supranaviculare.
3.
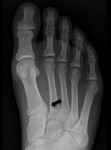
THE OS INTERMETATARSEUM
The os intermetatarseum (Fig. 5) is a relatively uncommon accessory bone of the foot,
usually found between the base of the first and second metatarsal bones,
often bilaterally.
The incidence ranges between 1,2 and 14 %.
Its etiology is uncertain: it may be due to variations in formation of the tarsal mesenchyme or it may be a true accessory center of ossification.
Most ossa intermetatarsea are asymptomatic; otherwise,
patients complain of pain and paresthesia,
with numbness radiating from the dorsum of the foot to the hallux and second toe,
increasing with plantar flexion. These symptoms are also known as anterior tarsal tunnel syndrome,
which is caused by compression of the deep peroneal nerve by the inferior retinaculum.
Standard anteroposterior,
lateral and oblique radiographs of the foot or CT should be made to identify the os intermetatarseum and to determine certain characteristics such as the position,
shape,
and size of a painful os intermetatarseum.
4.
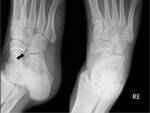
THE OS CALCANEUS SECUNDARIUS
The os calcaneus secundarius is a rare accessory ossification center of the foot,
present in 0,6 % of the population.
It is located anteromedial to the calcaneus,
flanked by the talar,
cuboid and navicular bone,
and has an ovoid or triangular shape.
An os calcaneus secundarius rarely causes symptoms and is most often an incidental finding on routine radiographs.
Patients can present with pain,
reduced mobility of the subtalar joint and repetitive spraining of the ankle joint.
Clinical differentiation with a calcaneonavicular coalition may be difficult.
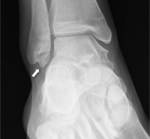
Plain radiographs reveal a smoothly corticated ossicle anterior of the calcaneus,
best visualized on (medial or lateral) oblique films (Fig. 6 and Fig. 7).
CT is more suited to evaluate the relation with the adjacent bones.
On MR,
a small and well-corticated ossicle is seen adjacent to the anterior calcaneal process.
If the os calcaneus secundarius is symptomatic,
reactive bone marrow edema is present in both the accessory ossicle and the anterior calcaneal process (Fig. 7).
The main differential diagnosis of an os calcaneus secundarius is an old avulsion fracture of the anterior calcaneal process.
Imaging findings in these entities are similar and therefore,
diagnosis should rather be based on clinical and anamnestic findings; a history of severe trauma suggests avulsion fracture rather than os calcaneus secundarius.
5.
THE ACCESSORY NAVICULAR BONE
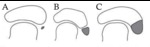
According to Geist,
three variants have been described (Fig. 8),
with a collective incidence of 4 to 21 %.
Type 1 accessory navicular bone (also referred to as os tibiale externum) (30 % of accessory navicular bones) (Fig. 9 and Fig. 10):
- is a well-defined round to oval bone,
2-3 mm in diameter,
located up to 5 mm medial and posterior to the navicular tuberosity;
- occurs as a sesamoid bone within the tibialis posterior tendon,
near the navicular insertion;
- is usually asymptomatic.
Type 2 accessory navicular bone (50-60 %) (Fig. 11):
- is a hemispherical bone,
measuring up to 12 mm;
- is connected to the navicular tuberosity by a 1-2 mm thick layer of either fibrocartilage or hyaline cartilage (syndesmosis or synchondrosis,
respectively);
- the posterior tibial tendon inserts on its rounded surface,
its flatter surface is facing the navicular bone,
to which it is connected;
- bilateral in 50-90 % of cases.
Type 3 accessory navicular bone (also referred to as cornuate navicular bone) (10-20 %) (Fig. 12):
- occurs as a very prominent navicular tuberosity;
- is thought to represent a type 2 accessory navicular bone that is fused to the navicular bone by a synostosis (as opposed to a syndesmosis or synchondrosis).
TIBIALIS POSTERIOR TENDINOPATHY
As the presence of a type 2 or 3 accessory navicular bone acts as if it were the native os naviculare with the bulk of the posterior tibialis tendon inserting onto it,
the leverage of the malleolus on the tibialis posterior tendon is reduced (Fig. 13).
This causes more stress on the tendon,
thus augmenting the risk for a tendinopathy.
Clinically,
patients can present with a flat foot deformity (and associated hindfoot valgus).
On MR,
tibialis posterior tendinopathy is characterized by a contour deformity with intrasubstance signal intensity alterations.
SYMPTOMATIC ACCESSORY NAVICULAR BONE
In the case of type 2 accessory navicular bone,
repetitive contractions of the tibialis posterior tendon can produce shearing stress at the synchondrosis and accessory navicular bone and generate medial foot pain.
CT reveals cortical irregularity and sometimes even fragmentation of the accessory navicular bone.
MR demonstrates bone narrow edema inside the bone and/or high signal intensity at the synchondrosis and surrounding soft tissues.
A valgus stress injury may even fracture the synchondrosis.
A type 3 accessory navicular bone may become symptomatic by causing irritation of the overlying soft tissue,
with possible adventitial bursa formation.
6.
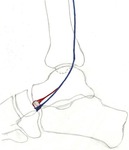
THE OS PERONEUM
The os peroneum is a sesamoid bone located within the peroneus longus tendon.
The peroneus longus muscle is a strong foot evertor.
Its tendon passes downward around the lateral malleolus,
on the lateral surface of the calcaneum,
and the groove of the cuboid,
to enter the sole of the foot.
Two anatomical variants can be present along the course of the tendon: a hypertrophic peroneal tubercle and an os peroneum.
The hypertrophic peroneal tubercle will be discussed in another section.
The position of the os peroneum is variable,
but typically adjacent to the lateral or plantar aspect of the cuboid,
at the level of the calcaneocuboid articulation.
There are multipele soft tissue tethers that anchor the ossicle to the plantar fascia,
fifth metatarsal base,
cuboid,
and peroneus brevis tendon.
The os peroneum is one of the most common ossicles of the foot,
with an incidence varying between 5 % and 26 %.
It is bilateral in approximately 60 % of cases and has a variable appearance,
being bipartite or multipartite in approximately 30 % of adults (Fig. 14).
Histologically,
the os peroneum consists of a variable mixture of bony and fibrocartilage tissues. Fibrocartilaginous substance is present in tendons at the site where they wrap around the bony pulley. Mechanical stress leads to enchondral ossification at the center of the fibrocartilaginous portion of the tendon. The degree of ossification is variable,
with some ossa peronea appearing as well-formed cancellous bony masses while others are diffuse and stippled with only a few trabeculae. As such,
the os peroneum ranges in size from a small spicule to a bony mass. These spicules should not be misinterpreted as calcific tendonitis.
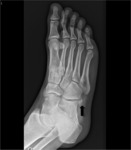
This variable histological composition is reflected in imaging studies. In only 20 % of adults,
the os peroneum is fully ossified,
and radiographically visible on an oblique view of the foot.
US is more sensitive than radiographs in detecting non-ossified fibrocartilaginous remnants,
as ultrasound is exquisitely sensitive in detecting structures with differing acoustic impedance.
On MR imaging,
the ossicle appears as a discrete area of bone marrow or cartilage at all pulse sequences and should not be confused with an intrasubstance tear of the peroneus longus tendon.
The os peroneum is mostly asymptomatic and appears as an incidental finding on imaging studies performed for other reasons. However,
due to its superficial and intratendinous location,
adjacent to the cuboid bone and embedded in the peroneus longus tendon,
the os peroneum is prone to acute and chronic injury.
Acute injury occurs after direct trauma or forceful inversion/supination of the foot,
with violent contraction of the peroneus longus tendon,
whereas chronic injury follows poorly defined repetitive or recurrent injuries to the foot.
PAINFUL OS PERONEUM SYNDROME (POPS)
The painful os peroneum syndrome or POPS,
a term coined by Sobel et al,
includes a spectrum of conditions,
such as a frank rupture or chronic attrition of the peroneus longus tendon,
(stenosing) tenosynovitis of the peroneus longus tendon,
acute or chronic fracture of the os peroneum (sometimes complicated by hypertrophic callus formation),
diastasis of a multipartite os peroneum,
or chronic mechanical stress of the os peroneum against adjacent structures (os peroneum friction syndrome). A fracture of the os peroneum or diastasis may be associated with a complete rupture of the peroneus longus tendon.
Physical examination reveals swelling and tenderness over the cuboid bone area. Pain is exacerbated by resisted plantar flexion of the first ray and during the heel rise phase of gait. Eversion strength can be reduced.
POPS is a rare cause of lateral foot pain,
and can be easily overlooked due to its rareness.
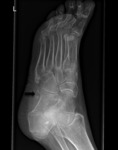
Plain films
Plain films are the first choice imaging modality in an acute traumatic setting.
The presence of soft tissue abnormalities cannot be assessed.
- Bony fragments with irregular contours that fit like ‘pieces of a puzzle’ suggest a fracture (Fig. 15).
- Fragment displacement of 6 mm or more is diagnostic of a fracture complicated by a complete rupture of the peroneus longus tendon.
Ultrasound
High resolution ultrasound can demonstrate cortical bone irregularities and can,
as such,
complement plain films in the diagnosis of an os peroneum fracture.
Furthermore,
focal pain under transducer pressure is suggestive of a (stress) fracture of the os peroneum.
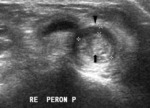
Ultrasound may show such associated abnormalities of the peroneus longus tendon as
- Tendinosis: inhomogineously hypoechoic thickening of the tendon.
- Tenosynovitis: anechoic fluid in the tendon sheath. Hypoechoic thickening of the synovium of the tendon sheath,
with reduced mobility of the tendon,
indicates stenosing tenosynovitis (Fig. 16).
- Partial tear: longitudinal anechoic splits within a thickened tendon.
- Complete tear: fluid filled gap or discontinuity of the tendon.
MR
MR has a superb capability to detect bone marrow and soft tissue edema: early diagnosis of stress reaction to the os peroneum and adjacent structures (Fig. 17).
Diagnosis of abnormalities of the peroneus longus tendon can be:
- Tendinosis:
- Increased signal intensity of the tendon on all pulse sequences (Fig. 18).
- Pitfall: magic angle phenomenon.
This may occur when tendon fibers form an angle of about 55° with the main magnetic vector,
especially when a short echo time is used (T1,
PD and gradient echo sequences). The peroneal tendons are particularly susceptible to the magic angle effect,
as they descend down the ankle. Imaging the foot in mild plantar flexion (approximately 20°) can avoid this phenomenon.
- Tenosynovitis: high signal intensity fluid surrounding the tendon (Fig. 19). Stenosing tenosynovitis occurs when synovial proliferation and fibrosis surround the tendons,
preventing their free excursion. Stenosing tenosynovitis appears as intermediate signal intensity on all pulse sequences. Gadolinium enhancement and complete obliteration of the fluid may also be seen.
- Partial tear: high signal intensity longitudinal splits within the tendon.
- Complete tear: high signal intensity and discontinuity of the tendon.
MR imaging can be equivocal in case of an os peroneum fracture:
- The small size and low signal intensity of the distal fragments can cause difficulty in visualization.
- The bigger proximal fragment can be distracted over several centimeters proximal to the calcaneocuboid joint
- Bone marrow edema in the os peroneum can also complicate assessment of os peroneum fracture because the edema can be difficult to distinguish from the abnormally high signal intensity in adjacent abnormal peroneal tendons.
7.
THE SESAMOIDS
Sesamoids are ossicles arising inside a tendon.
The largest sesamoid in the human body is the patella,
arising in the quadriceps tendon.
The os peroneum,
os vesalianum,
and accessory navicular bone type 1,
discussed in other sections of this poster,
are also sesmoid bones.
Functionally,
they act to protect the tendon and to increase its mechanical effect.
Like the accessory centers of ossification,
sesamoids may not be bilaterally symmetric.
Unlike the other ossicles,
sesamoids can be part of a synovial joint,
and have one or more articular facets. The sesamoid dorsal surfaces are cartilaginous and articulate with concave facets of the first metatarsal head.
The sesamoids of the great toe are almost always present; they can be found beneath the first metatarsal head and include the tibial and the fibular sesamoids,
embedded in the medial and lateral tendon slips of the flexor hallucis brevis muscle,
which are blended with the distal tendons of the abductor and adductor hallucis muscles,
respectively,
before they insert into the base of the first proximal phalanx.
They may be unipartite,
bipartite (in 10 % of the population) or multipartite.
Bipartite sesamoids are usually larger and occur bilaterally in 25 % of cases.
Almost 90 % of bipartite,
and as good as all multipartite sesamoids,
involve the tibial one (Fig. 20).
Several studies report an association between bipartite tibial sesamoids and hallux valgus.
Bipartite and multipartite sesamoids are more rounded than fractured sesamoids.
The medial sesamoid usually lies slightly more distal than the lateral one,
making it more readily visualized by arthroscopy.
As it is more impacted by weight bearing than the fibular sesamoid,
it has a higher incidence of traumatic injuries.
Ossification occurs from 7 to 10 years of age,
earlier in females than in males.
Congenital absence of one or both sesamoids is exceedingly rare.
Tibial and fibular sesamoids are interconnected by a thick intersesamoid ligament,
which acts as a reflexion pulley for the flexor hallucis longus tendon,
and further stabilized by a thin superficial ligament (Fig. 21).
The capsuloligamentous complex of the first metatarsophalangeal joint consists of,
other than the intersesamoid ligament: the medial and lateral metatarsosesamoid ligaments,
sesamoid-phalangeal ligaments,
and collateral ligaments (Fig. 22).
Lesions of the capsuloligamentous complex,
fracture,
osteochondritis,
sesamoiditis,
avascular necrosis,
and arthritis are relatively common pathologies.
TURF TOE
Turf toe is named from the injury being associated with playing sports on rigid surfaces such as artificial turf and is a fairly common injury in football,
baseball,
basketball,
and soccer.
Often,
the injury occurs when someone falls on the back of the calf while that leg's knee and tips of the toes are touching the ground.
Athletic shoes with very flexible soles and cleats that get stuck in the turf also cause overextension of the big toe.
The capsuloligamentous complex thus becomes overstretched or even torn,
usually at the metatarsal neck,
which is the weakest point of attachment (Fig. 23).
Complete disruption of the capsuloligamentous complex with associated tearing of the plantar plate may lead to dorsal subluxation of the first proximal phalanx,
causing impaction into the dorsal surface of the first metatarsal head with cartilaginous damage.
Other associated injuries include adductor,
abductor or flexor hallucis injury and fracture of the sesamoids or separation of a bipartite sesamoid.
FRACTURE
Sesamoid fractures are usually transverse and involve the tibial sesamoid.
The fracture site is sharp,
irregular and there may be displacement (Fig. 24).
Nonetheless,
bipartite morphology is more common.
The bipartite cleft is transverse,
smooth,
with sclerotic cortical edges and no callus (Fig. 20).
Fractures have been described in bipartite and even in multipartite sesamoids.
Stress fractures usually appear in the context of sesamoiditis (see further down).
CT is essential in differentiating fractures from congenital clefts.
On MR,
edema replaces bone marrow fat and can as well be seen in the surrounding soft-tissue structures (Fig. 25).
OSTEOCHONDRITIS AND AVASCULAR NECROSIS
Osteochondritis of the sesamoids occurs infrequently.
Trauma probably is the most frequent cause.
Osteonecrosis with subsequent regeneration and excessive calcification may be present.
Usually,
the lateral sesamoid is involved (Fig. 26).
CT may show an enlarged or deformed sesamoid,
with irregular areas of increased density,
mottling,
and fragmentation.
On MR,
a subacute and a chronic phase can be discerned,
with variable increased signal intensity,
and hypointensity on PD fat-saturated images,
respectively.
INFECTION
Osteomyelitis rarely occurs in the sesamoids,
except in patients with diabetic peripheral neuropathy,
who are susceptible to direct contamination from skin damage and ulceration.
MR is of particular usefulness in evaluating diabetic neuropathy and infectious spreading in the forefoot.
SESAMOIDITIS
Sesamoiditis is an overuse injury involving chronic inflammation of one or both sesamoid bones and adjacent tendons.
It is most common in young adults and teenagers.
As with turf toe,
it is a common problem among athletes,
especially those whom require maximum dorsiflexion of the great toe.
There is a broad spectrum of changes on imaging,
ranging from bone marrow edema,
soft tissue edema,
joint effusion,
synovitis,
and tendinopathy,
to a frank stress fracture.
CT is helpful to demonstrate a possible stress fracture.
Some authors state that sesamoiditis can be withheld when edema on STIR,
T2-weighted fat-suppressed or proton density-seighted fat suppressed images is seen in the absence of abnormalities on T1-weighted images (Fig. 27).
OSTEOARTHRITIS
Arthritis of the sesamoids may result from progression of sesamoiditis,
chondromalacia,
or trauma.
Hallux rigidus,
gouty arthropathy,
or rheumatoid arthritis may be present.
As in any joint,
it is characterized by erosion of articular cartilage,
subchondral sclerosis,
and osteophyte formation.
On MR,
a joint effusion may be seen (Fig. 28).
SYMPTOMATIC BIPARTITE SESAMOIDS
Some literature reports describe a considerable rate of occurrence of symptomatic bipartite sesamoids,
especially when associated with hallux valgus.
On MR,
bone marrow edema concentrated at both sides near the bipartite cleft,
in the absence of a traumatic background,
may suggest this controversial entity (Fig. 29).
The authors of this poster believe that symptomatic bipartite sesamoids,
as a pathologic entity,
should be diagnosed with caution,
after a (stress) fracture has formally been excluded by MDCT.
Plain anteroposterior and/or oblique films can demonstrate such incidental findings as multipartite sesamoids,
absent sesamoids,
and give an overview of their left-right symmetry.
In addition,
they can suggest the presence of a fracture.
Lateral x-rays usually are not useful in evaluating a sesamoid-related disorder.
As CT better displays the cortication of margins than radiographs,
it is indispensable in the differentiation between a bipartite sesamoid and a fracture.
Both feet are preferentially being scanned,
so that comparisons can be made.
MR is superior in demonstrating bone marrow edema and in assessing the integrity of surrounding soft-tissue structures.
A third hallucal sesamoid may be seen more distally,
at plantar side of the first interphalangeal joint,
inside the flexor hallucis longus tendon.
The sesamoids of the second to fifth toes are variably present; they may develop at the metatarsophalangeal or at the interphalangeal joints.
At the fifth metatarsophalangeal joint,
there may be both a medial and lateral sesamoid.
Given the paucity of pathologic conditions linked to these ossicles,
they fall outside the scope of this poster.
8.
THE OS VESALIANUM
The os vesalianum is an accessory ossification center of the foot located proximal to the fifth metatarsal and found within the peroneus brevis tendon.
The incidence ranges from 0,1 % tot 0,4 %.
Oblique radiographs (Fig. 30) and CT reveal a small corticated bone at the lateral side of the base of the fifth metatarsal.
If it becomes become symptomatic,
the main diagnostic objective is to differentiate the os vesalianum from an ossifying apophysis of the fifth metatarsal base,
an apophysitis of the fifth metatarsal base (Iselin disease),
a fracture of the tuberosity of the fifth metatarsal,
non-union of a tuberosity fracture of the fifth metatarsal,
an ununited apophysis of the fifth metatarsal base,
or an os peroneum.
9.
THE OS SUBFIBULARE
The os subfibulare originates from an accessory ossification center under the tip of the lateral malleolus and is present in approximately 2,1 % of the general population.
The ossicle is usually asymptomatic.
Occasionally,
patients present with pain around the lateral malleolus or ankle instability with recurrent sprains.
An os subfibulare is typically an incidental finding on plain radiographs,
visualised as a round or comma-shaped bone with a well-defined cortex underneath the lateral malleolus (Fig. 31).
When symptomatic,
MR images generally reveal bone marrow edema in both the os fibulare and the adjacent bone (Fig. 32).
Additionally,
joint effusion and/or soft tissue swelling may be noticed.
The main differential diagnosis of a symptomatic os subfibulare is an avulsion fracture of the lateral malleolus.
In most cases,
differentiation can easily be made based on anamnestic and clinical grounds: a history of trauma and a swollen,
tender lateral malleolus are highly suggestive of an avulsion injury.
Plain radiographs show an irregular cortex of both the avulsion fragment and the tip of the lateral malleolus.
On MRI,
recent fractures are characterised by T2-hyperintense bone marrow edema adjacent to the fracture lines.
10.
THE HAGLUND DEFORMITY
A Haglund exostosis is a bony tuberosity on the posterosuperior aspect of the calcaneus,
located adjacent to the retrocalcaneal bursa.
Chronic repetitive compression of this exostosis,
usually associated with low-back shoes,
may lead to inflammation of the retrocalcaneal bursa and Achilles tendinosis,
together known as the Haglund syndrome.
Plain films
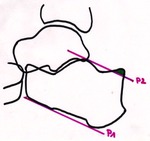
Plain films depicts the abnormal tuberosity on the posterior aspect of the calcaneus and can be used to draw the parallel pitch lines (Fig. 33).
The most frequently used measuring method for diagnosing a Haglund exostosis are the parallel pitch lines,
drawn along the superior and inferior aspect of the calcaneus.
Any bony projection above the superior line is abnormal (Fig. 34).
Effacement of the retrocalcaneal fat pad is an indicator for bursitis.
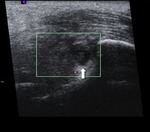
Ultrasound
Ultrasound is an excellent method for diagnosing bursitis and Achilles tendinosis,
depicting excessive fluid and hyperaemia of the bursa as well as thickening of the Achilles tendon (Fig. 35).
MRI
MRI may be helpful for equivocal cases as it may additionally demonstrate bone marrow edema in the posterior calcaneal tuberosity.
PD and T2-weighted sequences may also depict fluid distension of the retrocalcaneal bursa (Fig. 36).
The exostosis itself is best visualized on T1-weighted sequences.
Possible imaging differential diagnoses are Achilles insertional tendinopathy without associated exostosis or retrocalcaneal bursitis due to rheumatoid arthritis or seronegative spondyloarthropathy.
A stress fracture also often involves the posterior calcaneal process and may produce a similar bone marrow edema pattern on T2-weighted MRI-sequences,
but in this case the edema is most likely associated with a low intensity fracture line.
11.
THE HYPERTROPHIC PERONEAL TUBERCLE
The peroneal tubercle and the retrotrochlear eminence are bony protuberances located at the junction of the anterior and middle third of the lateral wall of the calcaneus. The peroneal tubercle is present in 40 % of individuals and separates the peroneus brevis tendon (anterior) from the peroneus longus tendon (posterior) sheaths. Together with the inferior peroneal retinaculum,
this bony ridge forms the inferior fibro-osseous tunnel containing the peroneus longus tendon (Fig.
38).
Variations in the shape and size of the peroneal tubercle are frequent. Saupe et al.
defined hypertrophy of the peroneal tubercle as a height >5 mm.
In subjects with significant hypertrophy,
the tubercle can be palpated as a local firm lump located at the lateral aspect of the calcaneum,
just inferior to the lateral malleolus (Fig. 38).
Because of chronic friction while wearing shoes,
the tubercle can cause local pain due to inflammation of the skin and subcutaneous soft tissues. An adventitial bursa can develop superficial to the peroneal tubercle and may be symptomatic when inflamed.
A hypertrophic peroneal tubercle causes a significant decrease of the diameter of the inferior osteofibrous tunnel,
potentially leading to impingement of the peroneal longus tendon,
chronic degenerative tendinopathy,
and/or tenosynovitis.
With persisting local friction,
the tendon can enlarge and the inferior retinaculum can thicken,
leading to a further decrease of the tunnel size and stenosing tenosynovitis. Chronic friction and degeneration can eventually result in partial or complete tendon tears.
The retrotrochlear eminence is seen in 98 % of individuals and is located posterior to the peroneal tubercle and the peroneal tendons. Hypertrophy of the retrotrochlear eminence is often associated with an accessory peroneus quartus muscle.
Plain films
- Anteroposterior and lateral standard radiographs often suggest this deformity (Fig. 39).
- An additional axial view of the calcaneum clearly shows the tubercle enlargement as an osseous outgrowth originating from the external surface of the calcaneum and pointing laterally.
CT
- CT can provide an accurate documentation of tubercle morphology (Fig. 40 and Fig. 41).
MR
- MR clearly shows the enlarged tubercle and associated soft tissue abnormalities (Fig. 42).
- Diagnosis of abnormalities of the peroneus longus tendon is described above.
Ultrasound
- Ultrasound depicts associated disorders of the peroneus longus tendon,
such as tendinosis,
partial/complete tears,
and (stenosing) tenosynovitis,
as described in the above section on POPS.
12.
TARSAL COALITIONS
A tarsal coalition is an acquired of congenital fibrous (syndesmosis),
cartilaginous (synchondrosis) or bony (synostosis) union between two or more bones of the hind- and midfoot.
The overall incidence of tarsal coalitions is 1 %.
Coalitions are often bilateral.
Together,
calcaneonavicular coalitions and talocalcaneal coalitions represent 90% of all tarsal coalitions.
Talonavicular,
calcaneocuboid and cubonavicular (Fig. 43) coalitions are much less frequent.
Coalitions restrict normal subtalar motion and can result in ridged flatfoot deformity,
pain,
tenderness,
stiffness,
tarsal tunnel syndrome,
and peroneal spastic flatfoot.
With progressive ossification of the coalitions,
symptoms become more pronounced albeit some coalitions remain asymptomatic.
Plain films
Calcaneonavicular coalitions (Fig. 44) are fairly well demonstrated on oblique films.
In osseous coalitions,
a bony bar that connects the two bones can be seen.
In a syndesmosis or synchondrosis,
the bones are in close proximity,
with irregular articular surfaces,
and the anteromedial calcaneus is abnormally flattened or broadened.
On lateral and anteroposterior radiographs,
the following secondary signs of a calcaneonavicular coalition have been described:
- talar beak (flaring of the superior margin of the talar head);
- short talar neck;
- calcaneonavicular bar (AP radiographs);
- “anteater sign” (elongated,
widened anterior process of the calcaneus);
- broad navicular bone (proximal articular cortex of the navicular bone wider than the articular cortex of the talar head);
- laterally tapered navicular bone (the lateral portion smaller than the medial portion).
Talocalcaneal coalitions (Fig. 45) most commonly involve the middle facet at the level of the sustentaculum tali and can be difficult to detect on standard radiographic views of the foot.
However,
on the lateral radiograph,
many secondary radiographic signs of talocalcaneal coalitions have been described:
- talar beak (flaring of the superior margin of the talar head): not always present in talocalcaneal coalition,
and to be differentiated from a talar ridge (more proximally,
at the attachment of the ankle capsule) and an osteophyte (more hooklike);
- “C sign” (continuous arc between the medial cortex of the talus and the inferior cortex of the sustentaculum tali): may be observed in either osseous or non-osseous coalitions.
Variations in sustentacular size,
orientation and suboptimal patient positioning may affect the reliability of this sign;
- nonvisualized middle facet (nonvisualization of the articular cortex and joint space of the middle subtalar facet);
- dysmorphic sustentaculum tali (sustentaculum tali is enlarged and has an ovoid configuration);
- short talar neck.
CT
State-of-the-art CT is performed of both feet at the same time and with multiplanar reconstructions.
Calcaneonavicular coalitions (Fig. 46) are best evaluated on sagittal and axial reconstructions.
Axial images show widening of the medial aspect of the anterior calcaneus and apposition to the navicular bone.
In non-osseous coalitions,
changes may be inconspicuous,
with little narrowing of the space between the bones and minimally associated degenerative changes.
Coronal images are most useful for evaluation of talocalcaneal coalitions (Fig. 47).
In osseous coalitions,
a bony bridge connects the middle subtalar joint.
Involvement of the posterior and anterior facets is less frequent,
but abnormal apposition or even fusion of the posterior facet may be observed.
In non-osseous coalition,
the middle facet of the subtalar joint may be narrowed,
with reactive changes in the underlying bone.
Normally,
the sustentaculum tali slopes upwards and medially,
but in talocalcaneal coalition,
it generally slopes downwards or horizontally.
Difficulties in diagnosing talocalcaneal coalitions can be encountered in fibrous coalitions,
if there are only minimal reactive bone changes or just slight narrowing of the middle facet.
Some coalitions involve only to the most posterior aspects of the middle facet.
Occasionally,
a sustentaculum may be hypoplastic instead of widened.
CT offers a precise evaluation of the extent of a coalition and clearly depicts associated degenerative changes.
CT is helpful in the diagnosis of rare coalitions,
such as the calcaneonavicular or cubonavicular types.
CT is useful in surgical planning,
by helping to determine whether resection is possible or arthrodesis is necessary.
MRI
MR imaging of the ankle and hindfoot should be performed in the three planes and consist of T1 sequences with T2- or PD-weighted fat-saturated images or STIR images.
Calcaneonavicular coalitions (Fig. 48) are best depicted on sagittal images. The coronal plane is best for evaluating talocalcaneal coalitions (Fig. 49).
In addition to the previously described signs on radiographs and CT,
tarsal coalitions exhibit some specific features on MR.
In osseous coalitions,
there is bone marrow contiguity across the fused articulation.
In cartilaginous coalitions,
an area of signal intensity similar to that of fluid or cartilage may be present in the joint space. Intermediate to low signal intensity may indicate a fibrous coalition.
On PD–weighted and T2-weighted fat-suppressed images or on STIR-images,
bone marrow edema is frequently identified along the fused articulation.
This edema may be observed in both calcaneonavicular and talocalcaneal coalitions and helps identify an unsuspected coalition when MR-images are obtained for unrelated indications.
Some investigators believe that MR imaging is superior to CT in the diagnosis of fibrous coalitions,
as structural alterations are often minimal at these joints.