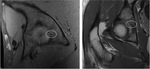
We retrospectively collected from 2010 until 2015,
25 cases of OO,
13 of them were intra or juxta articular hip OOs (table1).
The much higher percentage of intra or juxta-articular hip OOs depicted in this series,
when comparing with published radiological series,
was due to the fact that our hospital is a reference centre on hip surgery.
We have made the correlation between the radiological findings and the histology after surgery to validate the imaging diagnosis.
The most affected joint in OOs is the hip (4).
Evaluating the topographic distribution of our series 6 out of 13 were located in the femoral neck,
whereas the femoral head was the second most frequent localization.
To the best of our knowledge,
only one study was found in the literature evaluating the topographic distribution of OOs in the hip.
According to Laredo et al.,
from the 11 cases evaluated,
five lesions were located in the femoral neck while the other six were located in the trochanters,
intertrochanteric crest and line (9).
Considering our series,
the average age was 26 years old,
the youngest being 7 and the oldest 55 years of age.
These data is in keeping with the known bibliography that has been already referred.
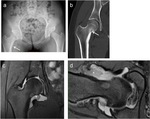
Standard radiographs in spite of being the first radiological approach only provide subtle findings due to the lack of sclerosis or periosteal reaction that usually is present in extra-articular localizations.
(4) In the present series,
standard radiographs only depicted in several cases some cortical thickening,
which is consider a non specific sign in the diagnosis of OOs.
(figure 3 and 3)
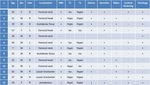
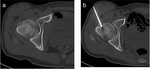
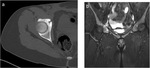
Computed tomography (CT) remains for some authors the modality of choice for detecting osteoid osteoma (figure 4),
providing the best characterization of both the nidus and the surrounding cortical sclerosis.
On CT the nidus appears as a defined radiolucent region with varying degrees of central mineralization (10).
Although there is some controversy in the use of intravenous contrast,
the nidus enhances at contrast-enhanced CT on a early phase,
some of them demonstrating wash-out (8).
However,
some OOs particularly the intra-articular ones might have little to no reactive sclerosis at all.
In those,
other signals such as synovitis and marrow edema are much better depicted on MRI.
Furthermore,
one must not forget that OO is a tumor and according to the vast majority of authors,
MRI remains the modality of choice for bone tumor exploration (9).
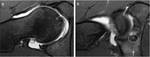
At MRI,
the signal in the nidus usually is isointense comparing with the muscle on T1-weighted images and is variable but mainly hyperintense on T2-weighted images.
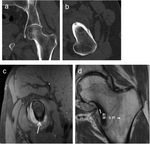
Precise localization of the nidus may not be easy on intra-articular lesions.
Some authors state that in 21% of intra-articular OOs the nidus is not identified on MR imaging and poorly identified in a further 29% (9).
In our series 5 out of 12 cases the nidus was not well visualized,
making up almost 45% of the cases (figure 5,
6 and 7).
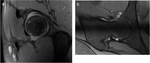
About 80% of patients with both intra and extra articular OO of the proximal femur develop synovitis and articular effusion of the hip joint (10).
No data was found reporting the percentage of synovitis specifically on intra-articular OOs.
Interestingly,
we found synovitis in all intra articular OOs that MRI was performed.
The only two cases where synovitis were not seen were the ones on juxta-articular localization.
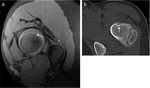
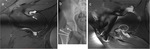
Bone marrow edema has been reported to occur in more than 60% of patients with OO (figure 8 and 9).
This edema is related by the replacement of cellular marrow elements by inflammatory cells and proteinaceous material (11).
Bone marrow edema produces low signal intensity on T1-weighted images and high signal intensity on fat-supressed T2-weighted images.
We consistently depicted bone marrow edema in 10 out of 12 cases.
While cortical thickening might be useful in depicting OO on CT the results in our MRI series proved to be very heterogeneous.
We also report two cases,
which initially were studied by MRI for femoro-acetabular impingement and subsequently underwent surgery (figure 10).
However,
persistence of symptoms after surgery led the clinicians to further investigate and seek the opinion of a multidisciplinary team,
so the MRIs were repeated and an intraarticular OO were depicted in both cases.
We retrospectively analysed the initial MRI of both cases and found a very small nidus that was overlooked.
The initial musculoskeletal radiologist in both cases,
in fact,
notice bone edema and synovitis on the MRIs that were interpreted in keeping with the cam FAI.
The leading MRI signal depicted in this series was synovitis.
It is well established that prolonged synovitis might cause severe hypertrophic deformation around the joint that leads to painful limitation of joint range movement and finally permanent sequelae.
Normal 0 false false false PT JA X-NONE
Thus,
a good understanding about the main radiological features of intra/juxta-articular OO may lead to shorten the usual diagnosis delay allowing to an early therapeutic intervention that may prevent potential skeletal complications.