These diseases may be infectious (cellulitis,
necrotizing fasciitis,
soft-tissue abscesses,
pyomyositis,
osteomyelitis,
septic arthritis),
inflammatory (arthritis,
polymyositis),
or neoplastic (lymphoma,
Kaposi sarcoma).
INFECTIOUS CONDITIONS:
Patients with AIDS are susceptible to opportunistic and non-opportunistic infections that can affect the skin,
subcutanous layers,
bones and joints.
- Cellulitis
Cellulitis is frequently due to bacterial infection or local trauma that compromises the dermis and subcutaneous tissue and is usually caused by local flora such as Streptococcus and Staphylococcus.
Although most cases of cellulitis are diagnosed clinically it is important to assess if there is extension to deeper layers.
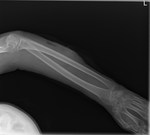
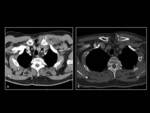
In uncomplicated cellulitis skin thickening,
septation of the subcutanous fat,
and thickening of the underlying superficial fascia is usually demonstrated (Fig 1). MRI is more sensitive at depicting subtle subcutaneous infections.
Conservative treatment with antibiotics is sufficient in this superfitial infection.
- Fascitis:
Both necrotizing and nonnecrotizing fasciitis are commonly preceded by trauma in patients with some degree of immunosuppression but can also be primary findings.
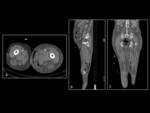
Necrotising fasciitis refers to a rapidly progressive and often fatal infection of soft-tissue fascia deep to the skin but superficial to the muscles often resulting from a polymicrobial infection.
The process initially begins in the superficial fascial planes and progresses into the deep fascial layers causing necrosis by microvascular occlusion (fig.2).
It should always be noted that no imaging modality can reliably exclude underlying necrotising fasciitis in the absence of soft tissue gas and negative study should not preclude obtaining tissue biopsy.
Also,
in cases with very high clinical suspicion imaging should not delay surgical intervention.
Hence,
imaging plays a very limited role in diagnosis and management of necrotising fasciitis.
- Pyomiositis:
Pyomyositis is a more common manifestation in HIV.
This is usually the result of opportunistic infection with Staph aureus,
although other organisms can be implicated including; S pyogenes,
Mycobacterium tuberculosis,
M avium-intracellulare,
Nocardia asteroides,
Cryptococcus neoformans,
and Toxoplasma.
The clinical presentation consists of three stages: Pain in one muscle group and low grade fever; followed by increasing pain,
fever and oedematous change; and finally development of an abscess with necrosis of the muscle and worsening systemic illness.
CT is useful in demonstrating the asymmetry in muscle size,
oedema and collections.
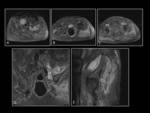
As already mentioned MRI is more sensitive for early changes.
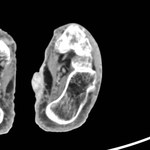
Intravenous administration of contrast material can help differentiate necrotic from viable musculature because the nonviable tissue will demonstrate lack of enhancement (fig.3).
If antibiotic therapy is initiated before substan- tial suppuration occurs,
surgery can be avoided.
- Osteomyelitis.
After septic arthritis,
osteomyelitis is the second most common musculoskeletal infection in HIV-positive patients and results from hematogenous spread,
direct extension from a contiguous focus of infection,
or direct inoculation.
Like pyomyositis the most common organism isolated is S aureus,
though infection with any number of organisms including mycobacterium tuberculosis,
E coli,
C neoformans and N gonorrhoea are encountered.
The most frequently involved bones are the wrist,
tibia,
femoral heads.
The radiological findings are not specific to HIV infection.
Plain radiography may be normal in the early stages of infection; later showing soft tissue swelling,
periosteal reaction,
cortical destruction and sequestration.
Bone scintigraphy is sensitive for infection,
but its specificity is poor with false positives seen in trauma and degenerative change.
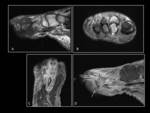
MRI has been shown to be most sensitive and specific for the diagnosis of osteomyelitis.
Areas of bone oedema and pus appear as low signal on T1WI and high signal on T2WI.
Contrast enhancement can demonstrate areas of bone and soft tissue infection as well as demonstrating necrotic bone (fig.
4).
Bacillary angiomatosis is an unusual form of osteomyelitis that specifically affects the HIV infected population.
The name “bacillary angiomatosis” came from the descriptions of the vascular proliferation,
seen on histologic examination of clinical specimens.
Bone lesions on imaging tend to be osteolytic foci that may range from well-circumscribed lytic lesions involving the cortex to ill-defined lesions with extensive cortical destruction,
medullary permeation,
and periosteal reaction.
CT and MRI are more sensitive,
especially MRI where the lytic lesions appear dark on T1WI and bright on T2WI.
- Septic arthritis
Septic arthritis and osteomyelitis generally present in a similar way in HIV-positive and HIV-negative individuals (Fig.
5).
S.areus is the most commonly isolated agent.
Presentation is usually monoarticular and the hip is the joint most affected.
Patients with CD4 counts of less than 100 cells/μl may present with multiple involved sites,
concomitant skin infections,
and are often infected with agents other than S.aureus.
Treatment consists of surgical debridement and antibiotics.
INFLAMMATORY PROCESSES
HIV-infected individuals are at an increased risk of developing rheumatic pathology.
Before the widespread implementation of highly active anti-retroviral therapy (HAART),
retrospective studies calculated the rates of musculoskeletal complications from 11% to 72%.
In the HAART era,
rheumatic complications declined significantly but continue to be prevalent with even new manifestations emerging.
- Arthralgia:
Arthralgia is a common but unspecific complaint of HIV-infected persons.
It is most frequently observed in the knees,
shoulders and elbows.
An intermittent painful articular syndrome has only a short duration (a few hours),
but may require opioid analgesics.
- Reiter Syndrome
Reiter syndrome has been linked to HLA B27 in both HIV positive and negative individuals.
Reiter syndrome has been described in HIV infected patients following infection with Salmonella Yersinia and Shigella species but may follow an incomplete course from the classic triad of urethritis,
conjunctivitis and arthritis.
Distal lower extremity involvement is more prevalent than upper extremity involvement. It affects hands,
wrists,
and feet with a distribution that is unilateral or bilateral and asymmetric (it becomes symmetric in later stages).
It can have a very similar appearance to psoriatic arthritis with the classic features of ill-defined erosions,
enthesopathy,
bone proliferation,
early juxta-articular osteoporosis,
uniform joint space loss and fusiform soft tissue swelling.
Dramatic improvement with effective HIV suppression or anti-TNF-α biologics was described.
- Psoriatic arthritis:
Psoriatic arthritis has a higher prevalence among HIV-infected and AIDS patients than in the general population.
Exacerbation of underlying psoriasis or development of the disease in high-risk individuals requires assessment for HIV infection.
In general,
the severity of psoriasis parallels the impairment of the immune system and the use of anti-retrovirals generally improves HIV-associated psoriasis.
In advanced HIV infection,
psoriasis can be generalized and extremely resistant to therapy.
Anti-TNF-α agents have been successfully administered to a few patients,
but in some cases have been associated with polymicrobial infections.
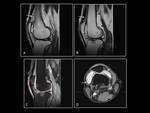
The hall mark of Psoriatic arthritis is the combination of erosive change with bone proliferation in a predominantly distal distribution.
It most commonly affect sacroiliac joints and spine,
involving less frequently knees (fig.
6),
elbows,
ankles and shoulders.
- Polymiositis
Polymyositis is the most common muscular manifestation in HIV-infected patients and must be distinguished from pyomyositis,
which is its most important differential diagnosis,
because their treatments differ.
In contrast to pyomyositis,
polymyositis typically occurs early in the course of HIV infection .
Symptoms of polymyositis include bilateral symmetric muscle weakness most often affecting the proximal muscles,
and a usual elevation of creatinine kinase levels.
Radiographically both entities can be distinguished because in pyomiositis rim enhancement is usually demonstrated.
- Zidovudine myopathy
Zidovudine causes a myopathy by interfering with the replication of mitochondrial DNA.
High doses of AZT for prolonged periods of time have been associated with a dose-dependent reversible myopathy that is clinically and radiographically indistinguishable from polymyositis.
The treatment of choice is cessation of ZDV,
with subsequent normalization of clinical and laboratory features in several months.
NEOPLASMS
Musculoskeletal neoplastic manifestations that may be seen in HIV infection include lymphoma and Kaposi sarcoma.
- Lymphoma:
NHL is the second most common type of tumor in patients with HIV infection and AIDS after Kaposi sarcoma and typically occurs in the late stages of the disease with CD4 counts below 200 cells per microliter.
The relative risk of NHL in AIDS patients is about 60 times that in the general population and it appears in younger patients (median age 37).
It is considered a diagnostic criteria of AIDS.
AIDS-NHL are more frequently of high grade and involve extranodal sites.
20-30% have concomitant bone infiltration.
Primary NHL of bone is very rare accounting for only 3-7 % of extronadl disease.
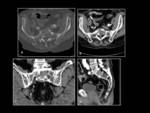
On radiographs and CT lytic lesions with extensive cortical destruction may be seen.
Soft tissue masses are usually associated.
Skull,
pelvis,
spine and the lower extremities are most often involved (fig.
7).
- Kaposi Sarcoma:
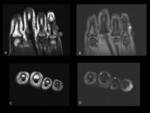
Kaposi sarcoma can present with a wide range of clinical features ranging from minimal cutaneous disease to a rapidly progressing neoplasm.
Bone lesions are most often discovered accidentaly in the context of radiological investigations done for the screening of visceral involvement.
It is a very rare entity and is most frequently secondary to local extension from the skin (fig.
8 and 9).