METHODS AND MATERIALS:
The wide range of injuries was observed on 1.5 and 3 T MR imaging closed system.
A dedicated flex coil for studying small parts of the limbs was used.
Scanning was done either in supine positioning of the patient,
with the arm at the side of the body or prone position was used in claustrophobic patients with arm extended and placed in the scanner.
Routine MR imaging of the finger was performed in the axial,
sagittal,
and coronal planes in relation to the MCP and PIP joints of the extended finger or in some cases with flexed finger .Sequences included T1-weighted images,
PD fat suppression,
short inversion time inversion-recovery images,
3-D gradient sequences.
Routinely the field of view was 8–9-cm with a section thickness of 3–4 mm.
However 1–2-mm-thick sections were obtained with a three-dimensional VIBE gradient-echo pulse sequence.
Systematic approach was adopted to review the image and after reviewing the bones and joints (9) tendons and ligaments were analyzed.
These included evaluation of the flexor mechanism,
extensor mechanism,
collateral ligaments,
volar plates,
and sagittal bands.
Because the MRI anatomy of tendons and ligaments is especially complex firstly the focus will be on these anatomical details and in that context evaluation of injuries (13).
FLEXOR TENDONS AND PULLEY SYSTEM:
The digital flexor tendons pass through the carpal tunnel and extend toward their respective fingers.
The flexor mechanism of the index,
middle,
ring,
and small fingers consists of the flexor
digitorum profundus (FDP) and the flexor digitorum superficialis (FDS) tendons(12).The FDS tendon splits at the distal metacarpal,
passes around the FDP tendon,
and reunites deep to the FDP tendon at the level of the PIP joint forming Camper chaiasma .
Each FDS tendon has two separate slips that insert on the volar surface of the mid diaphysis of middle phalanx.
Similarly,
each FDP tendon inserts on the volar aspect of the proximal diaphysis of distal phalanx.
Flexor tendons run along osteofibrous canals lined by a synovial sheath and are connected to the synovial sheath by the vincula,
from which they blood supply .The floor of the fibro-osseous canal is the volar aspect of the phalanges and the volar plates of the MCP and interphalangeal joints.
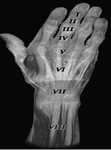
The fibrous portion of the canal consists of five annular pulleys (A1–A5),
which are transverse thickening of the tendon sheath,
and three cruciform pulleys (C1–C3),
formed by crisscrossing fibers of the components of the annular pulley (Fig 2)
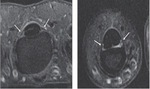
MRI anatomy of Flexor Tendons:
On MRI,
normal flexor tendons have low
T1 and low T2 signal.
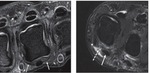
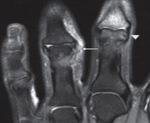
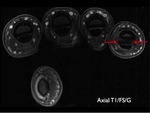
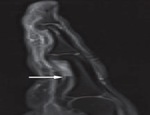
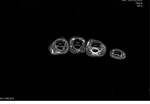
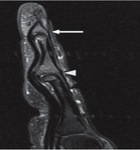
The FDS located superficial to FDP tendons is best assessed on axial proton density–weighted fat-suppressed images (Fig 1).
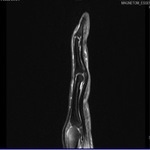
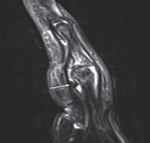
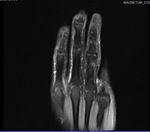
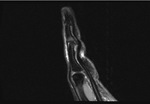
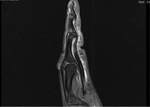
The insertion of the flexor tendons is best seen on sagittal proton density–weighted fat-suppressed images
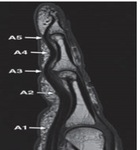
MRI Anatomy of Pulley System:
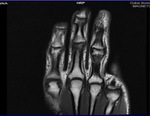
On 1.5 or 3-T MRI,
the five annular pulleys are best seen in axial and sagittal planes as small areas of soft-tissue thickening along the volar aspect of the flexor tendons (Fig 3).
· A1 along the volar aspect of the MCP joint and base of the proximal phalanx
· A2 along the volar aspect of the mid diaphysis of the proximal phalanx
· A3 along the volar aspect of the PIP joint
· A4 along the volar aspect of the mid diaphysis of the middle phalanx
· A5 along the volar aspect of the DIP joint.
The thinner more flexible cruciate pulleys are difficult to visualize on MRI.
Injuries of Flexor Tendons:
Normal 0 false false false EN-US JA X-NONE
Injuries to the flexor tendons are less common then injuries to the extensor apparatus.
There are two groups of lesions: open injuries and closed injuries.
Open Injuries:
Flexor tendon lacerations associated with skin wounds are more common than closed traumatic ruptures.
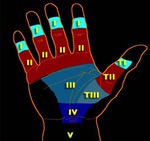
The flexor tendons are divided into five zones (Fig 4):
· Zone I extends from the distal insertion of the FDP tendon to the distal insertion of the FDS tendon.
· Zone II from the distal insertion of the FDS tendon to the distal palmar fold.
· Zone III extends from the proximal part of the A1 pulley to the distal part of the flexor reti- naculum.
· Zones IV and V consist of the carpal tunnel and the forearm proximal to the flexor reti- naculum,
respectively.
Zone I injuries are isolated lacerations of the FDP and manifest clinically as loss of active flexion of the distal phalanx.
Lacerations in zone II are the most frequent and carry the most severe prognosis.
Trauma in the four proximal zones is associated with lesions of both flexor tendons resulting in loss of active flexion of the PIP and DIP joints and injuries to the major neurovascular structures have been reported (15,16).
MR imaging has been successfully used to diagnose tendon disruption.
It can also accurately visualize the ends of the lacerated tendon and the degree of injury,
thus allowing differentiation of partial and complete tear (Fig 5).
Primary surgical repair (within 24 hours) is preferred for injury in any of the five zones.
Emergency repair is indicated when there are associated neurovascular bundle injuries.
Closed Injuries:
Closed tendon injuries include avulsion of the FDP tendon and avulsion of the FDS tendon .
Avulsion of the FDP tendon is the most frequent type of closed rupture caused by sudden hyperextension during active flexion.
This lesion is called “sweater finger” or “jersey finger” .The FDP tendon of the ring finger is most commonly injured.
This injury is often missed in the acute phase because of lack of classic deformity,
swelling and pain.
Sagittal T1-weighted MR image clearly shows a laceration of the FDP tendon and the gap between the tendon ends (Fig 6).
This injury is divided into four main types based on level of the lesion,
tendon retraction,
and the absence or presence of a bone fragment:
· Type I lesions - retraction of the tendon into the palm.
· Type II lesions- tendon retraction to the PIP joint with a small bone fleck at the level of the PIP joint.
· Type III lesions- avulsion of a large bone fragment,
in place by the A4 pulley.
· Type IV lesions- type III lesions associated with simultaneous avulsion of the FDP tendon from the fracture fragment.
Isolated avulsion of the FDS tendon is a rare injury,
most reported cases are associated with an FDP tendon injury.
• On T2-weighted fat-suppressed and proton density–weighted fat-suppressed sequences,
flexor tendon tears are seen as fluid signal.
• On T1weighted sequences,
flexor tendon tears are seen as intermediate or low signal,
although associated hemorrhage may show increased signal.
• Avulsion fractures are seen as focal areas of cortical discontinuity.
• Large avulsion fragments show increased T1 signal from fatty marrow.
• Small cortical avulsions are with decreased T1 and T2 signal.
• Flexor tendon tears may have associated tenosynovitis.
When it is chronic,
present with clinical findings of trigger finger.
Pulley Injuries on MRI:
Complete tears of the annular pulleys may be visualized directly as a focal discontinuity of the pulley fibers.
In the absence of direct visualization,
pulley tears may be suspected when bowstringing of the flexor tendon is present.
Bowstringing is seen as an increased gap between the flexor tendon and the volar surface of the phalanx (6).
The longitudinal extent and degree of the bowstringing is related to the number of pulleys torn and finger position increasing with forced flexion (Fig 8).
It is important to recognize that partial pulley tears may not result in bowstringing.
Additional indirect findings of pulley injuries include edema superficial and deep to the pulley and fluid within the tendon sheath (Fig 7).
Other authors have reported that the size of the tendinous gap during forced flexion increases proportionally with the number of disrupted pulleys.
This gap varies from 2–5 mm for isolated complete lesions to 5– 8 mm for simultaneous complete lesions of multiple pulleys.
Measurement of the tendinous gap has no significance in partial ruptures.
EXTENSOR MECHANISM:
The extrinsic extensor tendons,
receive contributions from intrinsic extensor tendons.
The extrinsic tendons include tendons of the extensor digitorum communis i.e.
EDC fourth extensor compartment,
extensor indexes proprius i.e.
EIP the fourth extensor compartment),
and extensor digiti quinti minimi the fifth extensor compartment(14).
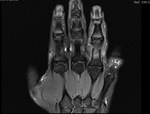
The EDC tendon provides tendon slips to the index through small fingers,
EIP tendon insertion the index finger,
extensor digiti quinti minimi tendon inserts on the small finger (Fig 9).
The intrinsic extensor tendons arise from the interosseous and lumbrical muscles.There are four lumbrical muscles,
three palmar interosseous muscles,
and four dorsal interosseous muscles.
The lumbrical tendons cross the MCP joint on the volar aspect of the deep transverse metacarpal ligament and the interosseous tendons cross the metacarpophalangeal joints on the dorsal aspect of deep transverse metacarpal ligament (17,26).
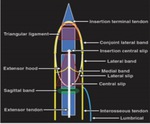
The intrinsic tendons insert on the radial or ulnar side of the proximal phalanx via the medial band and on the dorsal digital expansion as the lateral band .
The complex anatomic arrangement over the dorsum of the proximal phalanx is referred to as digital extensor expansion or extensor hood.
On MR images,
the normal extensor tendons appear as thin structures of very low signal intensity in the expected locations.
It is important to note :
· The axial and sagittal planes are the most useful for tendon identification (Fig 10) .
· The triangular and retinacular ligaments are not well visualized on MRI.
· Stabilizing fibrous structures,
especially the sagittal bands,
are characterized by uniform low signal intensity.
These bands are best seen in axial planes.
Injuries of Extensor Tendons:
Injuries to the extensor mechanism of the finger are common because it consists of thin,
superficially located structures.
Tendons have lacerations and also closed tendon injuries,
including avulsion.
Open Injuries:
There are eight zones (Fig 11):
· Zone 1 located at the DIP joint.
· Zone 8 at the distal forearm.
· The odd zones correspond to the articular areas and an injury to these zones may create a lesion of the extensor apparatus and the articular structures.
· Laceration of the terminal tendon may take place in zone 1,
leading to deformity of the distal phalanx in flexion i.e.
open mallet deformity
· Laceration of the central slip in zone 3 ends up to boutonnie`re deformity i.e.
flexion of the PIP joint and hyperextension of the DIP joint.
· In zone 5 there may be injury to the sagittal bands (20),
leading to tendinous subluxation or dislocation (Fig 12).
· In the even zones,
due to the semicircular morphology of the extensor apparatus,
a partial lesion is usually found.
Partial-thickness tear is seen as areas of increased signal intensity on T2-weighted within a portion of the tendon.
Complete tendon laceration show discontinuous tendons and ends are irregular.
MR imaging can also depict the gap produced by the lesion (18,19).
Acute laceration shows tendon gap with intermediate signal intensity on T1-weighted images and high signal intensity on T2-weighted images; consistent with edema and hemorrhage.
Sometimes by metallic devices,
a frequent finding is the presence of microartifacts,
which appear as tiny areas of signal void.
A possible “magic angle” effect can be detected due to orientation of the extensor tendons approaches an angle of 55°
Closed Injuries:
These include mallet finger,
boutonnie`re deformity,
and subluxation or dislocation of the extensor tendon mechanism at the MCP joint (23).
The site and deformity of these lesions is same as mentioned in the open injuries.
· Mallet finger is the most common closed tendon injury seen in sports and can result from a direct blow to the dorsum of the distal DIP joint.
If left untreated,
a mallet deformity will frequently progress to a swan-neck deformity caused by retraction of the extensor mechanism.
The MR imaging appearance overlaps that of open mallet injuries .
· A boutonnie`re deformity is the result of an injury to the central slip at or near its point of insertion on the base of the middle phalanx.
Less frequently,
a boutonnie`re deformity is associated with a fracture of the central slip attachment .
· Subluxation or dislocation of the extensor digitorum communis tendon at the MCP joint occurs as a result of tearing of the sagittal bands of the extensor hood (Fig 13).
This injury is the result of a direct blow forcing the finger into flexion or of forced flexion and ulnar deviation of the finger.
Ulnar subluxation is more common and radial subluxation is unusual (25) .
LIGAMENTOUS STRUCTURES OF FINGERS:
The important ligamentous structures of fingers are the collateral ligaments,
the volar plates,
and the sagittal bands.
The collateral ligaments are the main stabilizers of the MCP,
PIP,
and DIP joints.
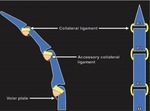
There are two proper collateral ligaments and two accessory collateral ligaments per joint.
The volar plates are quadrangular shaped fibrocartilaginous structures present at the MCP,
PIP,
and DIP joints(11).
The volar plates are attached to the volar aspect of phalanges,
collateral and the accessory collateral ligaments,
at MCP to the deep transverse metacarpal ligaments and the sagittal bands (Fig 14).
MRI Anatomy of Collateral Ligaments
The proper collateral ligaments of the MCP joints attach proximally to the side of the metacarpals and phalyngeal head.
The proper collateral ligaments courses distally and slightly obliquely to attach to the volar one third of the base of the phalanges.
The distal attachment is slightly broader than the proximal attachment (7,8).
The proximal attachment of accessory collateral ligaments is volar to the respective proper collateral ligament.
The accessory collateral ligaments fan out distally and volarly and attach to the volar plate (Fig 15).
MRI Anatomy of Volar Plates
On MRI,
the volar plates consist of a relatively
Normal 0 false false false EN-US JA X-NONE
thick fibrocartilaginous portion distally and a thinner membranous portion proximally(23).
At the PIP joints,
there are thin proximal expansions on either side of the volar plate called checkrein or check ligaments.
These attach to the volar surface of the proximal phalanx.
The checkrein ligaments are not well seen on MRI (Fig 16).
Finger Ligament Injuries
The most common ligament injuries of the finger occur at the PIP joint,
which can dislocate in dorsal,
volar,
or lateral directions (21).
· Dorsal dislocations are often associated with volar plate tears and avulsion fractures.
If a fracture fragment is involving greater than 40% of the articular surface,
it result in an unstable fracture-dislocation.
· Dorsal dislocations leave the collateral ligaments intact however become irreducible if there is tears of the proximal attachment of the volar plate and intraarticular entrapment of the volar plate fibers (24).
· Lateral dislocations are often associated with collateral ligament tears and at least partial tears of the volar plate.
· Volar PIP joint dislocations can produce a tear of the central slip.
· Dislocations of the DIP joints are relatively uncommon because of greater stability.
Dorsal dislocations result from a hyperextension injury and most commonly involve the index finger.
The other complications are same as those of PIP joint (Fig 17).
MRI of Finger Ligament Injuries
On MRI,
collateral ligament tears are typically seen at their proximal attachment(Fig 18).
In contrast,
volar plate tears typically involve their distal attachment(22).
Radial collateral ligament results from forced ulnar deviation at the metacarpophalangeal however isolated tears of the ulnar collateral ligaments at the metacarpophalangeal joint are relatively rare (Fig 19).
Sagittal band tears may be associated with extensor tendon dislocation.