Keywords:
Infection, Education and training, Diagnostic procedure, Ultrasound, Plain radiographic studies, MR, Paediatric, Musculoskeletal system
Authors:
N. Larkman1, A. White1, C. Davies2, K. A. Kingston2; 1Leeds/UK, 2York/UK
DOI:
10.1594/essr2016/P-0129
Background
A limp is a deviation from normal age appropriate gait pattern and incidence is quoted as 1.5-3.6/1000 <14 years. Causes of atraumatic limp in a child range from innocuous pathology such as transient synovitis through to paediatric orthopaedic surgical emergencies such as joint sepsis and slipped upper femoral epiphyses.
Prior to any investigation a thorough history,
clinical examination,
including gait assessment and baseline blood investigations,
including CRP and wbc, will ensure best use of the radiology department.
It will help triage patients likely to have self limiting pathology from those with significant disease.
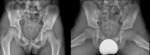
Infection can affect children of all ages Fig. 1 ,
occuring at any location in comparison to the non infective commonly encountered atraumatic causes: Transient Synovitis (4-10 years); Developmental Dysplasia of the Hip (0-4 years); Perthes disease (4-10 years) and Slipped Upper Femoral Epiphysis (adolescents usually>10 years) which are hip joint pathologies associated with children in specific age groups.
Radiological Investigations:
- Radiographs - Plain Radiograph of the area of clinical concern may be the only imaging performed.
Pelvis AP and Frog Leg lateral are the most commonly requested in our institution with images reviewed by a Radiologist prior to the patient leaving the department. Fig. 1
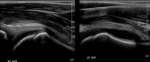
- Ultrasound - Good spatial resolution and good sensitivity for joint effusions Fig. 2 and collections which is particularly relevant when assessing for potential sepsis.
However, unable to differentiate between septic or reactive effusions unless able to demonstrate ancillary signs such as cortical bone/cartilage destruction.
- CT - High radiation dose - limited application in initial diagnosis Potentially useful for surgical planning and to rule in/out specific osseous differential diagnosis i.e.
osteoid osteoma.
- MRI - Best available imaging test for assessing for osteomyelitis,
spinal infection and sacroileitis, however,
in paediatric population may require general anaesthesia with associated risks and waiting time.
- Bone Scintigraphy - High radiation dose - sensitive but non specific.
Useful to assess for multiple sites of bone involvement i.e.
CRMO or metastases.