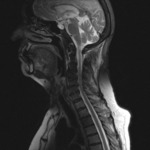
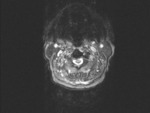
At Clinic of traumatology in Zagreb,
trauma patients with “some” degree of weakness according to ASIA impairment scale underwent MRI,
after evaluation of the spine with X-ray (three standard projections) and possible CT exam ( CT is needed for all moderate to severe spine trauma when the point of interest is imaging bony anatomy / type of fracture,
acute blood,
and calcified tissues).
MRI was obtained in patients whose CT scan showed a potentially unstable injury,
patients who coud not localize symptoms,
and those with neurological symptoms,
or with progression of symptoms.
The SCIWORA scenario (Spinal Cord Injury WithOut Radiographic Abnormality) is also an indication for MRI.
The SCIWORA is defined as the presence of neurologic symptoms in the absence of radiographic (X-ray) findings. This is classically seen in patients with symptoms ranging from transient neuropathy to complete cord lesion. Often a transient neuropathy will have a lucid interval only to return hours to days later.
The presentation in adults ranged from central cord syndrome to complete paralysis. Treatment is based on MRI findings.
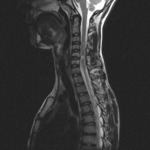
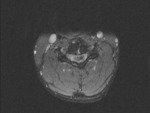
Our MRI protocol includes: sagittal and axial T1-weighted (T1WI),
T2-weighted (T2WI) images and sagital short-tau inversion-recovery (STIR) sequences (3 mm thick) or T2WI with fat saturation ,
as well as an coronar T2WI,
without contrast.
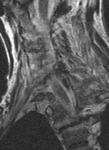
T1 and T2 -weighted images,
STIR or T2 with fat saturation,
offer a good anatomic overview and visualiation of possible traumatic injury of the bone: vertebral body,
posterior elements (pedicles or fasets fractures,
fracture dislocation or subluxation),
spinal canal stenosis (traumatic disc herniations,
epidural collections/ haematoma) as well as potential spinal cord and soft tissue injury (ligamentous injury,
spinal cord swelling/ edema and hemorrhage,
contusion or compression).
We retrospectively reviewed 36 patients diagnosed with traumatic cervical spine injury who had MR imaging performed within 96 hours of trauma.
Data regarding ligamentous injury,
disk injury,
the exten to the spinal cord injury and intraspinal / extramedullary hematoma was collected,
as well as data about bony trauma / fracture.
Ligamentous injury : indicator of unstable lesions
Daffner et al described 5 radiographic signs that are suggestive of instability:
displacement of a vertebral body by 2mm,
widening between the spinal lamina by 2mm,
abnormalities involving the facets,
injury involving the posterior portion of the vertebral body and
an increased interpediculate width of 2mm.
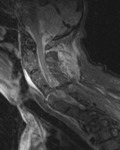
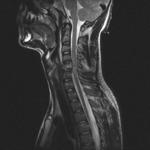
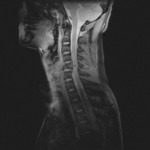
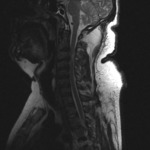
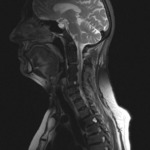
MRI can direct visualize injured anterior (ALL) and posterior (PLL) logitudinal ligaments.
An area of discontinuity indicates a disruption (figure 1).
The ligament can also be avulsed,
which is indicated by separation from bony structures.
This is exhibited as increased T2 and STIR signal deep to the ligament /bone marrow edema.
"Thinning" or "stretching" of the ligament may indicate injury.
The posterior ligamentous complex (PLC) acts to stabilise the vertebral column and is made up of the following structures: facet joint capsule,
ligamentum flavum,
interspinous ligament and supraspinous ligament.
Because the PLC is not as well defined as other ligaments,
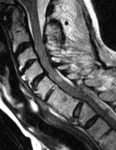
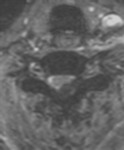
one can identify injury as increased T2 or STIR signal within the complex (figures 1 and 2).
Spinal cord injury
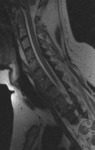
MRI is the only imaging modality for evaluation of the spinal cord.
The cord may be directly damaged by a traumatic event or by impingement of an associated injury,
such as a traumatic herniated disk (figures 11 and 12).
MRI can identify the level of cord injury and the associated soft tissue injuries.
Because of this,
it can assist in preoperative planning.
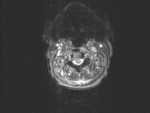
Injury of the cord is revealed by the presence of high T2 signal,
which indicates edema or contusion (figures 2, 4 and 10),
as well as by signal changes that are indicative of intramedullary hemorrhage (figures 1,
5,
6 and 7) or cord infarct.
Extramedullary hemorrhage
Posttraumatic epidural hematomas (figures 8 and 9),
which are thought to be venous in origin,
most often involve the cervical or thoracic spine.
Usually,
they are dorsal to the thecal sac,
as the PLL is firmly adherent to the dura anteriorly.
Subdural hematomas are most often ventral to the cord.
These collections can be clinically significant if there is cord compression.
MRI can provide an early diagnosis,
leading to prompt treatment.