Keywords:
Hyperplasia / Hypertrophy, Calcifications / Calculi, Arthritides, Education, Plain radiographic studies, MR, CT, Musculoskeletal system, Musculoskeletal soft tissue, Musculoskeletal joint
Authors:
B. Sharif, M. Khoo; Stanmore/UK
DOI:
10.1594/essr2018/P-0065
Imaging findings OR Procedure Details
Primary synovial chondromatosis (PSC) imaging findings:
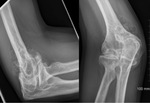
Plain radiograph
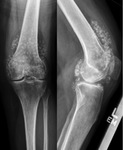
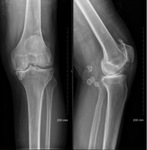
This is often abnormal in 70% of cases and may demonstrate the following features:
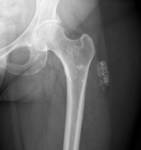
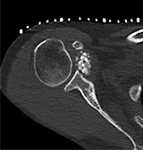
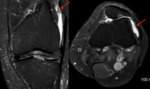
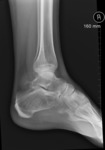
- Innumerable intra-articular calcifications of uniform size,
which are evenly distributed throughout the joint Fig. 1 (or less commonly tendon or bursa Fig. 5 Fig. 6).
Chondroid ring-and-arc pattern of mineralisation is common,
which can progress and undergo ossification.
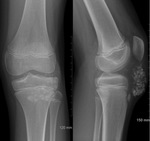
- In rare cases the chondral bodies can coalesce to form la arger,
conglomerate mineralised mass.
Fig. 4
- The joint space should be maintained,
however in chronic disease secondary osteoarthritis and joint space narrowing may develop.
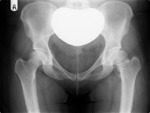
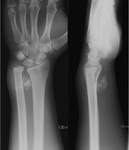
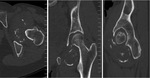
- Secondary periarticular erosions can be seen in up to 30% of cases,
which result from pressure effects.
These occur on both sides of the joint and range from well defined cortical defects to circumferential erosions resulting in an 'apple core' appearance.
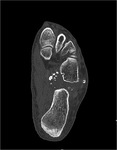
Erosions are more common in joints with a tight capsule such as the hip,
wrist and small joints of the hands and feet and less commonly in the knee or shoulder.
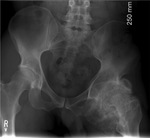
- Joint effusion. Fig. 3
Ultrasound
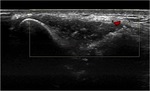
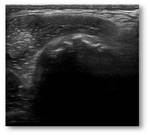
The loose bodies appear as heterogeneous avascular mass(es) containing echogenic foci surrounded by fluid.
Depending on the degree of mineralisation or ossification,
there may be secondary posterior acoustic shadowing. Dynamic ultrasound examination may demonstrate change in position of the the loose bodies. Fig. 7 Fig. 8
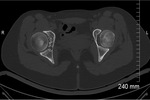
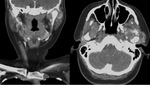
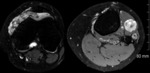
Computed tomography (CT)
- Synovial thickening +/- joint effusion.
- Ring-and-arc or punctate mineralisation of intra-articular bodies.
- 'Target' appearance may be seen - central fat density within intra-articular bodies representing central yellow marrow. Fig. 9
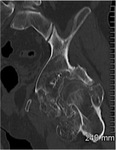
- Extrinsic bony erosion may be seen. Fig. 12 Fig. 14
- If intravenous contrast is given,
some loose bodies may demonstrate septal or peripheral enhancement.
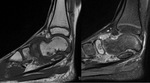
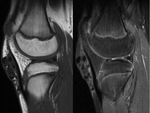
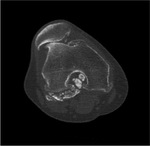
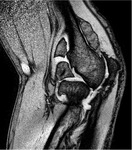
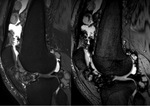
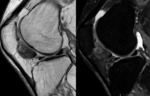
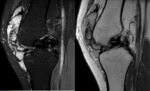
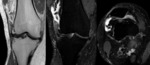
Magnetic resonance imaging (MRI)
There are three distinct patterns of the appearances of PSC on MRI (Kramer et al),
which correspond to Milgram's histopathological phases as described above:
- Intra-articular lobulated,
homogenous,
intermediate signal on T1 weighted images and high signal intensity on T2 weighted images.
This is the second most seen pattern.
Fig. 17
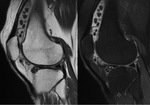
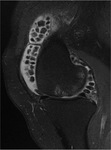
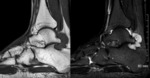
- As above but with areas of low signal intensity/signal void on all sequences (corresponding to calcification).
This is the most frequent pattern. Fig. 15 Fig. 16 Fig. 20
- As above but with high signal intensity foci relative to fat with a peripheral low signal rim.
This reflects ossification and is least frequently seen.
Other features on MRI:
- Synovial thickening
- Bone erosions
- Conglomeration of loose bodies
MRI is also useful for looking for:
- Bursal extension of intra articular disease.
- Marrow invasion in more aggressive disease.
Treatment/prognosis
- Can be self limiting,
conservative treatment e.g.
with non-steroidal anti-inflammatories.
- Surgical resection of intra-articular loose bodies,
if these are small,
by arthroscopic removal.
Arthrotomy is preferrable in larger lesions.
- Partial or full synovectomy for recurrent and persistent synovial metaplasia.
Complications
- Secondary degenerative change: this can make differentiation from secondary synovial chondromatosis difficult,
particularly in progressive disease. Fig. 16
- Recurrence post treatment: following synovectomy,
the incidence of recurrence is 3-23%.
Recurrence rate may be higher in tenosynovial chondromatosis.
Recurrence can occur from several months to several years after the index procedure.
- Malignant transformation to synovial chondrosarcoma: this is rare and occurs in 1-5% of cases.
It has only been described in intra-articular cases.
Evans et al (2014) found the median time from original diagnosis to malignant transformation to be 20 years.
Malignant transformation should be suspected in patients with multiple recurrences/aggressive recurrence,
evidence of aggressive features on MRI such as permeative or invasive bone erosions,
worsening pain and rapid increase in the size of a lesion.
Treatment is generally by amputation.
Differential diagnoses:
Secondary synovial chondromatosis (SSC)
- Can occur secondary to mechanical trauma of the hyaline cartilage and may be seen in the following circumstances: post trauma,
arthropathy (osteoarthritis,
rheumatoid arthritis,
arthritis post infection/inflammation),
osteochondral lesions (osteochondritis dessicans),
which cause intra-articular cartilaginous bodies.
- Patients with SSC tend to be older than patients with PSC.
SSC more commonly affects the knee,
hip and shoulder.
- Important differences between PSC and SSC: chondral bodies tend to be fewer in number and variable in size in SSC,
whereas they are numerous and of uniform size in PSC.
Concentric rings of growth may be seen within the calcified chondral bodies in SSC.
SSC chondral bodies do not demonstrate neoplastic qualities on histology. Fig. 21 Fig. 22 Fig. 23 Fig. 24
Pigmented villonodular synovitis (PVNS)
- Rare, benign proliferative synovial condition which can affect joints,
tendon sheaths (also known as giant cell tumour of the tendon sheath) and bursae.
It tends to present in the 2nd - 5th decades.
It is usually mono-articular and the most commonly involved joint is the knee,
although other joints such as the hip and ankle can be involved.
- Results in multiple intra-articular nodular lesions,
which have a villous appearance and tend to bleed,
resulting in characterstic haemosiderin deposits which are dark on all MRI sequences.
It is of low to intermediate signal on T1 and T2 weighted images,
of hyperintense signal on STIR and demonstrates blooming artefact on gradient echo sequences.
The lesions can also cause bone erosions. Fig. 25 Fig. 26
Synovial haemangioma
- An uncommon,
localised benign vascular tumour which can spread to joints or muscles and is most commonly seen in childhood/early adulthood.
They are most commonly found in the knee joint,
although may also be seen in the elbow,
ankle and wrist joints.
Patients typically present with pain,
which exacerbates and remits.
- On MRI,
this appears as a lobulated or diffuse intra-articular mass which is of intermediate signal on T1-weighted images.
It is markedly hyperintense on T2-weighted images,
with low signal intensity septations/vascular channels +/fluid-fluid levels.
Post gadolinium T1-weighted images demonstrate marked enhancement.
MRI appearances can mimic that of PVNS,
lesional biopsy and histological assessment may be required in some cases. Fig. 27 Fig. 28
Lipoma arborescens
- A rare,
benign condition characterised by diffuse replacement of the subsynovial tissue by mature fat cells,
giving rise to villous transformation of the synovium.
It affects joints,
although involvement of bursae and tendons sheaths has also been described.
Patients tend to present with joint pain and swelling.
- The typical MRI appearance is a large frond like mass arising from the synovium which is of fat signal on all pulse sequences.
A joint effusion may be present.
There is a distinct absence of haemosiderin.
Secondary effects such as bone erosions,
synovial cysts or degenerative change may also be present.
Fig. 29 Fig. 30
Synovial chondrosarcoma
- This is extremely rare.
The aetiology is often unclear if it arises from synvoial chondromatosis or de novo.
Similarly to PSC,
there is synovial metaplasia,
resulting in multiple intra-articular chondral bodies which may calcify/ossify.
It affects patients in the 4th-7th decades of life.
The knee and hip joints are most commonly affected.
It can be difficult to differentiate this from PSC on imaging (see complications section above). Fig. 31 Fig. 32