A retrospective review of 15 patients with FD and 1 patient with OFD was conducted.
Radiographs were available in 11 patients,
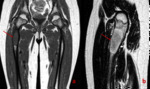
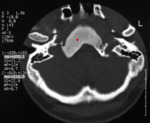
MRI in 5 patients and CT in 3 patients.
M-FD was found in 11 patients,
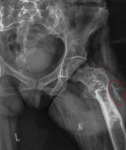
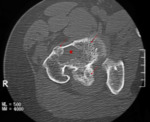
involving the pelvic bones (3 patients),
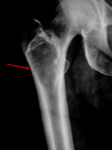
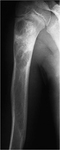
the humerus (2 patients),
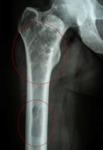
the femur (2 patients),
the fascial bones (2 patients),
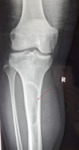
the tibia (1 patient),
and the ribs (1 patient) [Fig.
1,
2,
3,
4].
P-FD was found in 4 patients.
In one of them,
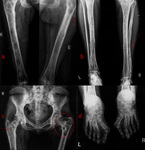
the ipsilateral femur and tibia were affected whereas in the remaining three,
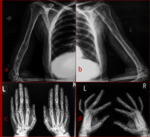
multiple long and small tubular bones,
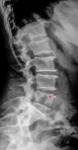
the skull and spine were involved.
The spine is a quite uncommon site of P-FD,
being involved in about 15% of the cases.
Among patients with P-FD,
one suffered from MAS [Fig.
14,
15,
16],
another had multiple coexisting exostoses [Fig.
10],
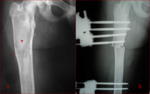
while malignant transformation of a femoral site of P-FD was seen in a third patient [Fig.
9].
The variability of the FD appearance,
in some cases required differentiation mostly from Paget’s disease of the bone,
due to common radiological characteristics,
mostly in case of mixed regions of sclerosis and lucency.
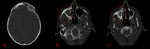
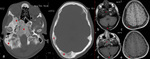
The key to the differential diagnosis in craniofacial FD is that the inner diploic table is typically spared (not displaced),
in contrast with Paget’s.
Furthermore,
Paget disease has a predilection for the skull vault and usually spares the facial skeleton.
In the long bones,
it usually begins as a subchondral area of lucency.
In addition,
the classical appearance in Paget disease is expanded bone with a coarsened trabecular pattern,
with sclerotic changes occuring much later in the disease process.
In most of our patients,
the diagnosis of FD was based on the typical pattern of ground-glass lesion with surrounding sclerotic rim.
Demographics and lesion location are also different in case of Paget’s disease.
It can be intricate to distinguish a malignant lesion from malignant transformation of an FD lesion.
In our case,
imaging revealed no well-defined osteolytic lesion within the ‘‘ground-glass’’ matrix and only minimal periosteal reaction.
The presence of extended ossification in the adjacent soft-tissue made the diagnosis unclear.
The most consistent radiographic feature of FD-related malignancies in patients who have not been subjected to surgery is an ill-defined,
mineralized,
osteolytic lesion within or near areas of ‘‘ground-glass’’ opacity,
associated with cortical destruction.
It is to be noted that demonstration of mineralization is not a specific sign of osteosarcoma associated with FD,
and definite diagnosis should be based only on histology.
FD was an incidental finding in all but three patients.
The most common symptom among symptomatic patients was rapidly increasing pain at the site of involvement,
while one presented with endocrine disorders due to MAS.
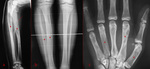
Radiographic appearance varied from lucent/ground glass,
mostly in younger patients [examples in Fig.
1,
3,
13] to mixed/sclerotic [Fig.
2,
5,
9],
with or without the presence of calcification.
FD lesions caused Shepherd Crook’s deformity in long bones [Fig.
7] and bone expansion in all affected bones,
most striking in cases of craniofacial FD [Fig.
8,
13].
Lesions surrounded by a layer of sclerotic reactive bone (rind sign),
were indicative of fibrous dysplasia [Fig.
1,
3,
7,
16].
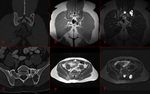
CT and MRI were more sensitive for fascial and pelvic FD but not satisfactory enough for lesions of long bones.