The patient age,
localization of pain when possible,
length of time of symptoms,
previous history of trauma or infection,
signs of systemic illness such as fever and tachycardia,
and laboratory findings all help direct the focus of imaging.
Certain diseases are more common in certain age groups.
Transient synovitis of the hip and undiagnosed developmental dysplasia of the hip (DDH) should be considered in infants and toddlers presenting with refusal to weight bear or reluctance to use the limb.
Between 4 and 10 years of age transient synovitis,
Legg-Calvé-Perthes (Perthes’) disease,
and juvenile idiopathic arthritis (JIA) form important differentials.
In adolescents,
slipped upper femoral epiphysis (SUFE) should also be considered.
However,
important disease processes associated with significant morbidity and mortality,
such as septic arthritis,
osteomyelitis and neoplasm,
can all be seen in any pediatric age group.
If symptoms are transient,
and there are no concerns of infection or malignancy (the child is not clinically unwell) often no further imaging is required.
If symptoms persist,
conventional radiography is the initial investigation of choice.
Anteroposterior (AP) view of both hips are standard,
along with frog-leg lateral view of the pelvis (AP view with hips in abduction and external rotation) when the differential includes SUFE or Perthes’ disease.
Some disorders are bilateral,
although rarely symmetrical,
and comparison with the other hip may prove useful in detecting subtle subchondral changes.
Radiographs are sensitive for detection of fractures and benign and malignant lesions.
They will not detect joint effusions,
unless they are large,
resulting in displacement of fat planes or subluxation,
and are also inadequate at evaluating cartilage and soft tissue.
Ultrasound (US) is the most common imaging method for suspected hip effusion,
usually using a high resolution linear transducer with an anterior parasagittal approach.
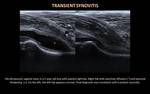
The normal hip joint capsule follows the contour of the neck of femur in a concave shape.
When an effusion is present,
the layers of joint capsule are separated by hypoechoic fluid,
causing the anterior layer to become convex in relation to the neck of the femur (figure 1).
Comparison with the normal side can be valuable in assessing small effusions and minor synovial thickening.
Hip capsules should be symmetric within 2 mm.
More than 2 mm of difference is consistent with an effusion.
US cannot confidently differentiate between sterile,
purulent or hemorrhagic effusion,
but it can be used to guide both diagnostic and therapeutic aspiration.
An infective process may display hyperaemia of the tissues around the area of infection evident on power or colour Doppler.
Magnetic resonance imaging (MRI) has very high sensitivity and specificity and is excellent for visualizing joints,
soft tissues,
cartilage,
and bone marrow.
Contrast enhanced MRI is useful for confirming osteomyelitis,
delineating the extent of malignancies,
identifying subtle stress fractures,
and diagnosing early Perthes’ disease or secondary avascular necrosis (AVN).
Bone scintigraphy has a role in localizing disease in the assessment of multifocal disease entities such as osteomyelitis and metastatic disease.
Computed tomography (CT) is limited to assessment of complex bone lesions or identification of a nidus in suspected osteoid osteoma.
INFLAMMATORY CAUSES
Transient synovitis (figure 1)
Most common nontraumatic cause of hip pain,
affecting children between 2 and 9 years of age.
Males are more commonly affected than females.
Previous history of a viral upper respiratory tract infection or mild trauma is common.
The child is usually systemically well with an acutely painful hip effusion.
When history is typical no imaging may be required.
The presence of bilateral joint effusions is suggestive of transient synovitis.
Absence of a hip effusion does not exclude transient synovitis in children with acute hip pain.
It is a self-limiting disorder.
Treatment is supportive,
including rest and anti-inflammatory medications.
Arthrocentesis should not be routinely performed in children with transient synovitis but it may allow rapid differentiation from septic hip while relieving capsular distension and consequent pain.
Juvenil idiophatic arthritis
Most common chronic arthropathy of childhood.
It is a diagnosis of exclusion characterized by arthritic symptoms lasting more than 6 weeks before the age of 16 years.
It affects the hip or sacroiliac joints and is frequently bilateral,
but may be unilateral.
MRI is more sensitive for soft-tissue changes and early diagnosis of disease,
often depicting synovial hypertrophy,
a joint effusion,
and bone marrow edema.
Plain radiographs are only of value in more advanced stages of the disease,
once osseous erosions and cartilage destruction have occurred,
showing joint space narrowing,
growth abnormalities,
and eventually ankylosis.
INFECTIVE CAUSES
Septic arthritis
Uncommon.
It may result from direct spread from adjacent osteomyelitis,
hematogenous spread,
or direct implantation related to penetrating trauma.
The most common causative organism is Staphylococcus aureus.
The infected hip joint should be emergently decompressed,
since the lytic enzymes within the infected fluid cause destruction of articular and epiphyseal cartilage and the increased pressure within the joint may lead to ischemia or infarction of the femoral head epiphysis.
The hallmark of septic hip arthritis is unilateral joint effusion.
Absence of fluid usually excludes septic arthritis.
Radiographs are insensitive for detection of early inflammatory change,
but they can provide clues to the presence of underlying joint effusion:
- increased distance of the femoral epiphysis from the lateral margin of the Köhler’s teardrop;
- asymmetric widening of the hip joint;
- bulging of the hip capsule.
Late manifestations of the disease such as osteoporosis,
epiphyseal enlargement,
erosive change,
and advanced degenerative change are radiographically apparent.
US demonstration of joint effusion in an unwell child with raised inflammatory markers is highly suggestive of septic arthritis.
The patient may require ultrasound-guided aspiration or proceed straight to surgical joint wash out.
Absence of fluid usually excludes septic arthritis.
MRI is rarely needed,
but has a role in assessing associated osteomyelitis.
Common MRI findings suggestive of septic arthritis are joint effusion,
synovial thickening with enhancement of the affected side,
associated intraosseous or soft tissue fluid collection,
and marrow and soft tissue inflammatory changes; there may be decreased enhancement of the femoral head epiphysis.
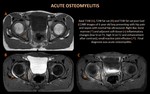
Osteomyelitis (figure 2)
Uncommon.
It has a higher prevalence in boys than girls,
and more than 50% of cases arise in children less than 5 years of age.
Osteomyelitis usually affects the metaphyses of long bones,
but can extend to involve the epiphysis in young children as a consequence of vessels crossing the growth plate.
Staphylococcus aureus is the most common pathogen implicated.
Salmonella infections are more common in children with sickle-cell anemia.
In children bellow 4 years of age are attributed to Kingella kingae.
Conventional radiography is insensitive to early disease,
showing subtle soft tissue stranding with no discrete bony abnormality.
Periosteal thickening,
osteopenia,
or loss of normal architecture usually does not become apparent for at least 7 to 10 days.
US is unable to visualize the bone marrow,
nevertheless it plays a role in the assessment of soft tissues and joints adjacent to infected bone,
being able to visualize soft tissue abscesses,
cellulitis,
subperiosteal collections and joint effusion,
and guiding diagnostic procedures such as fluid aspiration.
Although joint aspiration excludes septic arthritis,
a sterile effusion may be present as a sympathetic effusion secondary to osteomyelitis.
MRI is the imaging technique of choice for diagnosing osteomyelitis due to its high sensitivity and specificity for the detection of early bone marrow change,
abscess formation,
soft-tissue extension or other complications.
Bone scintigraphy,
positron emission tomography and whole-body MRI may identify and characterize multifocal or clinically occult disease.
DEVELOPMENTAL CAUSES
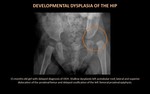
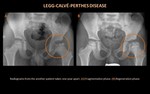
Developmental Dysplasia of the Hip (figure 3)
DDH is usually diagnosed in early infancy,
but patients may present late.
There may be associated hip dislocation,
dysplasia of the acetabulum and femoral head,
and deformity with leg length discrepancy.
Screening with US should generally be performed at 4 to 6 weeks of age.
In patients with DDH,
the α angle measures <50 degrees,
the bony rim of the acetabulum will be abnormally rounded or flattened and the femoral head may be normally situated within the acetabulum,
subluxed,
or dislocated on static images.
As the femoral heads begin to ossify,
generally around 3 months of age,
evaluation with ultrasound becomes limited.
After 4 months of age,
radiographic evaluation is indicated,
with the frog-leg lateral view important for evaluation of reducibility.
In DDH,
the acetabulum will appear shallow,
the ipsilateral femoral head ossification center will be small compared with the normal hip,
there may be subluxation and dislocation,
which carry a worse prognosis with a greater risk of early degenerative change.
VASCULAR CAUSES
AVN is a condition induced by compromised blood supply resulting in progressive destruction of bone.
It is most commonly idiopathic (Perthes’ disease),
but may be seen following trauma,
infection,
steroid treatment,
and in association with haematological diseases,
such as sickle cell anaemia.
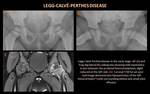
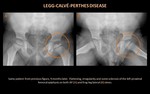
Legg-Calvé-Perthes Disease
Usually affects children between 4-10 years of age,
and is more common in boys.
Bilateral disease occurs only in 10-20%,
usually in an asynchronous fashion.
During childhood,
the proximal femoral epiphysis receives its blood supply via the lateral epiphyseal vessels.
Interruption to this blood supply results in ischemia and infarction.
The disease is self-limiting because the blood supply is eventually restored via recannulation of the existing vessels or neovascularization.
1.
Initial stage (figures 4 and 5)
- Femoral head epiphysis appears dense and sclerotic.
- Subchondral fracture line may be seen (subcondral radiolucency in the anterolateral epiphysis,
the “crescent sign”),
demarcating the extent of the infarction.
- Late in this phase,
the epiphysis begins to flatten,
losing height.
- These changes can be subtle and are often better demonstrated on frog-leg lateral view.
The acetabulum and femoral metaphysis may appear osteopenic due to disuse and local hyperemia.
2.
Fragmentation phase (figure 6A)
- Fissures appear within the dense physis,
running perpendicular to the articular surface.
- The anterolateral femoral head may come to lie outside the acetabulum due to hypertrophy of the articular cartilage of both the femoral head and acetabulum (phenomenon called “extrusion”).
- Metaphyseal cysts may appear.
3.
Regeneration phase (figure 6B)
- Mature lamellar bone replaces the necrotic bone.
- Development of neovascularity across the physis may result in early physeal closure.
- If the femoral head remains extruded during this phase,
it will result in chronic deformation of the femoral head (it becomes larger and flatter) with amixed lytic-sclerotic appearance and fragmentation,
and femoroacetabular incongruence.
4.
Healed stage
- Most hips heal without significant residual deformity.
Factors associated with poorer prognosis are obesity,
progressive loss of hip motion,
adduction contracture,
and longer duration from symptom onset to healing phase.
Radiographic findings also have prognostic implications: lateral subluxation of the femoral head,
lateral epiphyseal calcification,
a V-shaped defect in lateral epiphysis,
metaphyseal cyst,
and horizontally oriented growth plate are associated with a poor prognosis.
In the early stages,
MRI provides more precise localization and extent of involvement and has the highest sensitivity in diagnosing and detecting bony infarction,
when radiographs are still negative.
On follow-up examinations,
enhancement of the femoral head epiphysis can be seen,
owing to revascularization.
Signal intensity of the femoral head typically returns to normal after 6 years.
US and CT have limited utility.
Bone scintigraphy shows photopenia in keeping with total avascularity of the proximal femoral epiphysis.
MECHANICAL CAUSES
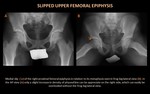
Slipped Upper Femoral Epiphysis (figure 7)
SUFE (or slipped capital femoral epiphysis (SCFE)) is the commonest adolescent hip disorder and results from the posteromedial displacement of the femoral epiphysis from the metaphys,
being essentially a Salter Harris type 1 fracture through the proximal femoral physis.
Idiopathic condition usually affecting boys,
between 12 and 15 years,
and frequently taller or overweight,
which causes increased shear stress across the physis leading to repetitive microtrauma.
It may be bilateral in 20 to 30% of cases,
but is rarely symmetrical.
Presentation may be acute,
with radiographic findings that can initially be subtle,
making it essential to perform both AP and frog-leg lateral views for full assessment.
Typical appearances include:
- widening and blurring of the growth plate (Bloomberg’s sign) with apparent reduction of the height of the epiphysis;
- visible medial slip;
- the “metaphyseal blanch sign” that implies an increase in radiographic density at the upper medial femoral neck secondary to the posteriorly projecting femoral head;
- loss of “Klein’s line” (a tangent drawn along the lateral cortex of the femoral neck on the AP view that should intersect the lateral epiphysis in the normal hip).
In early SUFE,
US can show a step-off between epiphysis and metaphysis due to the posterior slipping of the epiphysis,
and hip joint fluid with capsular distension.
MRI may reveal abnormal asymmetric widening and edema of the proximal femoral physis,
as well as joint effusion and periphyseal and adjacent metaphysis marrow edema.
It can also depict femoral head vascularity.
CT has very limited utility.
Bone scintigraphy shows increase metaphyseal uptake,
but is not routinely performed.
More chronic cases may present with complications or long-term sequelae such as AVN,
hip deformity,
or early osteoarthritis.
The treatment is surgical fixation to prevent further slippage.
NEOPLASTIC CAUSES
Uncommon.
Includes both benign and malignant entities,
such as osteoid osteoma,
aneurysmal bone cyst,
simple bone cyst,
chondroblastoma,
exostosis,
osteoblastoma,
chondroblastoma,
Langerhans cell histiocytosis,
leukemia/lymphoma,
osteosarcoma,
and neuroblastoma.
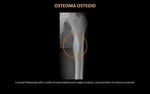
Osteoid osteoma (figure 8)
One of the commonest benign skeletal neoplasms.
It predominantly occurs in the long bones of the lower extremity in children and young males between 5 and 30 years of age.
Most cases are cortically based with a characteristic radiolucent nidus and surrounding area of dense reactive sclerosis.
Intramedullary osteoid osteoma are comparatively less common,
with the hip being the commonest site involved.
CT has higher sensitivity for nidus detection (sclerosis with a lucent nidus and central sclerosis) and may be required in difficult cases.
Osteosarcoma and Ewing’s sarcoma
The commonest primary malignant bone tumours in children.
Osteosarcomas are predominantly sited within the metaphysis of long bones,
affecting slightly older children,
whereas Ewing’s sarcoma more commonly affects the diaphysis and flat bones of pelvis,
and tends to occur in a younger age group.
Radiographic features are usually suggestive of a malignant or aggressive process (destructive lesion with permeative and moth-eaten appearance).
MRI is the technique of choice for assessment of tumour size,
bone destruction,
local staging,
and assessing soft-tissue involvement.