40 patients (BTB-20,
ST-20) were examined 1,
3 and 6 months after arthroscopic reconstruction of ACL,
having been operated on at the R.R.
Vreden Russian Scientific Research Institute of Traumatology and Orthopedics,
Saint Petersburg,
during 2005-2009.
In all patients,
in accordance with the type of transplant and the method of its fixation,
the standard arthroscopic single-bundle transtibial reconstruction of ACL was used.
Random systematic sampling was used in grouping of patients.
The studied groups were comparable in age,
sex,
level of physical activity,
combined injuries and severity of osteoarthritis of the knee joint (P>0.05) (table 1).
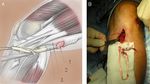
The BTB graft was formed through two horizontal incisions with subcutaneous excision of the patellar ligament and removal of its central third.
Bone fragments were taken from the lower pole of the patella and the tuberosity of the tibia.
To prevent shortening of the ligament and formation of the patella infera,
the defect in the middle part was not sutured (only the paratenon was sutured),
and the edges at the bone ends were brought together by two pairs of seams (Fig.
1).
The diameter of the graft was 10-12 mm,
that of the bone blocks 10-12 X 25-30 mm.
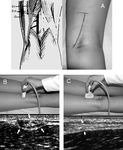
The tendons of the semitendinosus muscle of the thigh were isolated through a vertical incision 5 cm medially to the tuberosity of the tibia 3 cm below the articular slit of the knee joint.
The proximal fragments were taken using the tendon extractor with intersection of the muscular and tendon parts,
the distal ends being cut off along with the periosteum (Fig.
2).
After the operation,
immobilization was carried out up to 7-10 days with a plaster bandage; rest was recommended,
as well as walking with crutches,
isometric contraction of the quadriceps femur muscle,
relief of aseptic inflammation and pain syndrome.
From the second week,
knee joint fixation with semi-rigid orthosis with hinges was used; movements and dosed load on the operated limb were allowed.
Subsequent outpatient rehabilitation procedures were performed at the place of residence.
The sonography of the knee was performed on the "Siemens" apparatus with linear transducer 5-10 MHz in real time using the grey-scale image visualization.
The donor site was investigated on poly-positional mode in two mutually perpendicular section planes with simultaneous comparison with a healthy limb.
The donor patellar ligament was assessed from the anterior approach upon bending the tibia in the knee joint by 30°.
While cross-scanning,
the state of the place in the sites of bone tissue removal on the patella and tuberosity of the tibia was investigated.
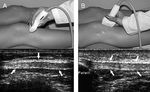
The remaining part thickness of the ligament and the width of the defect were estimated at the distance of 2 cm distally to the lower pole of the patella (Fig.
3).
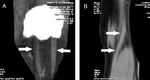
The emerging scar tissue at the site of anatomical location of the semitendinosus muscle tendon was studied from the posterior medial access on the lower third of the thigh (Fig.
4). When cross-scanning in the projection of anatomical location of the tendon-muscular part,
the regenerate thickness was measured,
setting the sensor proximally 10 cm above the articular slit of the knee joint.
Longitudinal scanning assessed the structure and echogenicity of the scar tissue (Fig.
4).
The obtained data were compared with CT-study.
Computer tomography of the knee joint was performed on the apparatus “Hi Speed” (J.
Electric) at x-ray radiation collimation of 2.5 mm in the spiral scanning mode in increments of 1.5 mm at a slice thickness of 3 mm,
pitch 1.5. The radiation load was less than 0.1 mSv. The structure of the tissues was determined visually and by densitometric parameters (Fig. 5).