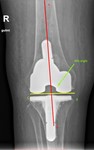
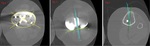
Femoral component varus/valgus alignment
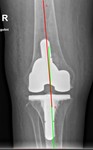
Femoral component varus/valgus alignment is determined by alpha angle (Fig.
1).
This is an angle between long axis of femur and a line tangential to articular surface of femoral condyles.
It should correspond to the angle between mechanical and anatomical femur axis and be between 3°-7° valgus.
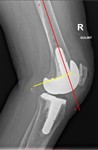
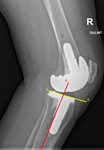
Femoral component flexion/extension alignment
Femoral component flexion/extension alignment is determined by gamma angle (Fig.
2).
This is an angle between long axis of femur and the most distal femoral fixation surface.
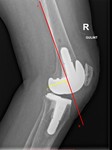
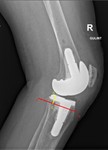
Posterior condylar offset
The posterior condylar offset is measured by distance between posterior border of femoral condyle and a line extended along posterior femur cortex (Fig.
3).
An excessive posterior condylar offset can lead to quadriceps weakness and an increase in posterior cruciate ligament tension.
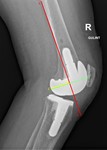
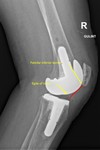
Posterior condylar offset ratio
The posterior condylar offset ratio is a ratio between posterior condylar offset and a line between anterior border and the tip of condyle’s dorsal aspect (Fig.
4).
It should be approximately 0,47 postoperatively.
Increased condylar posterior offset ratio can lead to a tight flexion gap and restriction of flexion.
Femoral component rotation
Femoral component is evaluated by comparing relationship of prosthesis and femur in axial plane.
There are two transepicondylar planes:
Surgical transpepicondylar axis corresponds to flexion/extension axis.
Difference between surgical and clinical axes is 3° internal rotation.
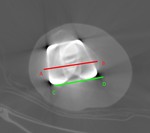
The femoral component rotation is an angle between dorsal condylar surfaces and transepicondylar axis (Fig.
5).
It should be 0-1° internal rotation (using surgical axis).
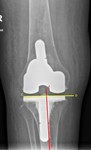
Femorotibial angle
It is an angle between tibial and femoral anatomical axes (Fig.
6).
It should be 4°-10° in valgus.
Tibial component varus/valgus alignment
Tibial component varus/valgus alignment is determined by beta angle (Fig.
7).
This is an angle between long axis of tibia and a line tangential to articular surface of tibial component.
It should be perpendicular to the mechanical axis.
Tibial slope
Tibial slope (sigma angle) is defined as angle in sagittal plane between anatomical axis of tibia and tibial component plane (Fig.
8).
Tibial slope stabilizes the knee in flexion.
It varies between different endoprosthesis,
but it should slope posteriorly approximately 10º.
Anterior slope should be avoided as it impedes posterior femoral rollback and leads to restricted knee flexion.
Tibial component rotation
Tibial component rotation is assessed by its relationship to tibial tuberosity (Fig.9).
A method offered by Berger is commonly used.
Firstly a geometrical center of tibial plateau is found by drawing a circle at bone borders - the center of this circle matches tibial center.
It should be “moved” to the level of tibial tuberosity.
Secondly a line perpendicular to the posterior border of tibial component is drawn and “moved” to the level of tibial tuberosity.
An angle between this line,
geometrical center of tibia and the medial third of tibial tuberosity is measured.
Correct component position should be approximately 18± 3° internal rotation.
An increase in internal rotation leads to patella maltracking and subluxation.
The level of joint line
The height of the joint line is a distance from the superior edge of tibial tubercle to the tibial component articulating surface (Fig.
10).
The level of joint line should not be altered 8 mm or more.
A tilted joint line may lead to postoperative pain.
Patellar height
Patellar height is defined as a distance from the inferior edge of patella/patellar component to the proximal edge of the insert (Fig.
11).
For good results it should be 10-30 mm.
Patellar tilt
Patellar tilt angle is an angle between a line tangential to anterior border of femoral component and a line connecting medial and lateral edges of patella (Fig.
12).
It may imply a tight lateral retinaculum,
a component malrotation or valgus alignment of the extensor mechanism.