Bone Tumours and Tumour like Conditions
The vast majority of the pathological fractures we encounter in our department involve benign bone lesions.
X-rays,
MRI and occasional CT scans are obtained in our institution.
As a DGH,
unless there is an obvious simple cyst or a known predisposing condition,
advice is usually sort from the Paediatric bone tumour unit in Birmingham,
as to diagnosis and management of these lesions.
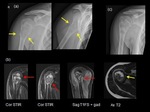
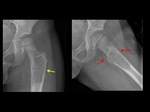
Unicameral bone cyst (UBC):
A unicameral bone cyst (UBC) represents about 3% of all primary benign bone tumours and approximately 85% are found in patients aged < 20 years (1).
Approximately 75% of patients with a UBC present with a pathological fracture.
(Fig.
1) A UBC is usually the most common cause of pathological fracture in children with a bone lesion (2).
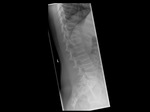
The most common sites of pathological fractures due to UBC are the proximal humerus followed by the proximal femur (3)(Fig.
2).
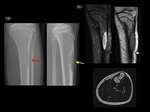
The radiological appearance of a UBC is of a well-defined,
centrally-located metadiaphyseal radiolucent lesion,
with or without medullary expansion.
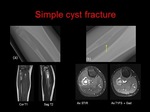
The “fallen leaf” sign can be seen on radiographs,
CT scans and MRI,
demonstrating the true cystic component of the lesion,
with a cortical fragment from a fracture in the central aspect of the cyst.
(Fig 3&4)
Occasionally the lesions appear slightly more complex on imaging and the exact diagnosis is only made after biopsy or curretage.(Fig.5)
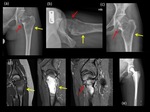
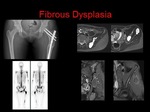
Fibrous dysplasia (FD):
Fibrous dysplasia is a non-hereditary condition in which a normal bone is replaced by fibrous tissue and islands of immature woven bone.
FD can be monostotic or less commonly polyostotic and it represents 5 to 7 % of benign bone tumours (4).
FD can occur in the epiphysis,
metaphysis or diaphysis of the bone,
with a predilection for the long bones,
ribs and craniofacial bones.
Lesions are typically discovered due to local pain and/or swelling at the site of the lesion,
incidentally or due to a pathological fracture (4).
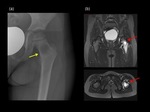
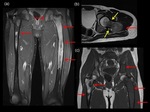
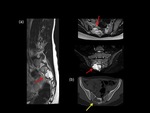
Pathological fractures can occur in 50 % of the monostotic FD in the proximal femur. (Fig.6&7)
The radiological appearance of FD varies from the classical lytic,
ground-glass appearance and sharp margins to more mature sclerotic lesions.
Polystotic disease can be associated with endocrine dysfunction and café-au-lait spots (McCune-Albright syndrome,
Fig.8&9) or muscular myxomas (Mazabraud syndrome,
Fig.10).
Very rarely,
FD lesions can undergo malignant transformation.
The polystotic variety can result in deformity such as coxa vara,
shepherd’s crook deformity of the proximal femur and bowing of the tibia.
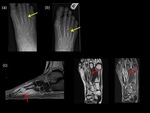
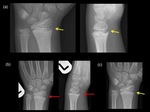
Non-ossifying fibroma (NOF):
NOF,
also known as fibrous cortical defects or non-osteogenic fibromas,
are the most common benign bone lesion in children.
It is estimated that between 30% and 40% of people aged < 20 years have a NOF,
and these are mostly asymptomatic (5).
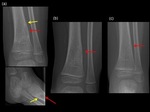
The radiological appearance of an NOF is a lytic,
well-defined lobulated and eccentric lesion in the metaphysis.
Multi-locular appearance,
ridges in the cortical wall,
sclerotic scalloped borders and erosion of the cortex are frequent findings without periosteal reaction in the absence of fracture (6).
NOFs are not typicallyassociated with pathological fractures (6),
however,
when fractures do occur,
it is usually in larger NOFs and almost always in the lower extremity.(Fig.
11)
The natural history of the NOF is to gradually regress within years.
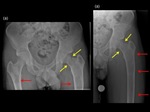
Enchondroma and Enchondromatosis:
Enchondromas are benign cartilaginous neoplasms that are usually solitary intramedullary bone lesions occurring most commonly in small bones of the hands and feet.
The distal femur and proximal humerus are other,
less common locations.
Enchondromas constitute 3-10% of all bone tumours and 12-24% of benign bone tumours.
They are the second most common benign tumour,
after osteochondroma and usually observed in 10 to 30 years of age and discovered incidentally in the vast majority of cases (7).
The lesions likely arise from cartilaginous rests that are displaced from the growth plate,
replacing normal bone with mineralized or un-mineralized hyaline cartilage and producing a lytic pattern on radiographs,
typically containing rings and arcs of chondroid calcifications.
Pathological fractures (Fig.12) and malignant transformation into chondrosarcoma are the most significant complications.
Enchondroma can be multiple such as in Ollier’s disease,
and associated with soft tissue haemangiomas in Muffucci syndrome.
Aneurysmal bone cyst (ABC):
Aneurysmal bone cyst (ABC) is a benign but locally aggressive tumour.
The prevalence of primary ABC is about 2% of all benign tumours of bone.
A total of 80% of cases will be diagnosed in patients younger than 20 years of age (8).
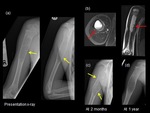
Patients usually present with local pain that has been present for several weeks or months,
or a pathological fracture.
(Fig.13) Rapid growth of the lesion can occur,
mimicking a malignancy.
Radiographically,
an ABC is an expansile,
lytic lesion that elevates the periosteum,
contained by a thin shell of cortical bone (9).
It can have well-defined margins or a permeative appearance,
resembling a malignancy (10).
Common locations include the femur,
tibia,
fibula,
humerus and the spine.
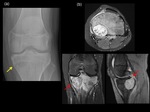
MRI,
typically,
will show a fluid-fluid level,
depicting the multi-loculated cavities filled with fluid.(Fig.14)
ABCs can sometimes be secondary to other primary benign lesions or malignant bone tumours.
Approximately 36% of patients will present with a pathological fracture,
which are usually in active lesions (10).
In most cases,
when an ABC is diagnosed,
surgical treatment is recommended.
Chondroblastoma:
Chondroblastoma has a prevalence of only 1 to 2% of primary bone tumours.
It commonly arises in the epiphyses and apophyses of long bones in adolescents and young adults,
typically before the second decade and prior to the closure of the growth plates (11).
On radiograph,
Chondroblastoma is typically well defined lucent lesion with sclerotic rim and associated chondroid matrix (11).
(Fig.
15)
Generalised lymphangiomatosis (GL):
GL is a rare multi-systemic disorder arising from the lymphatic system.
It is thought to be a progressive proliferation of lymphatic channels and increase in the number of complex anastomoses forming between them during intrauterine life (12). The end product is a continuous dilation of these interconnected thin- walled lymphatic vessels,
containing benign endothelial cells.
Lymphangiomatosis may be categorised macroscopically as either localised or systemic.
The localised form of the disease is isolated to a single anatomic location,
classically bone,
and have a good prognosis.
Seventy-five percent (75%) of cases in the systemic form include skeletal manifestations,
the occurrence of multifocal lymphangiomas involving the gastrointestinal tract,
lung,
and pleura creates additional management challenges.
Most cases of skeletal involvement are found incidentally on plain radiographic imaging,
or as a pathological fracture,
a consequence of an internally weakened bone structure (13).(Fig.
16)
The radiographic appearances are similar to those of solitary hemangioma,
with osteolytic lesion,
and usually a fine peripheral sclerotic rim.
The differential includes metastatic disease,
histocytosis X and Gaucher’s disease.
Neuroblastoma Metastasis (NBL):
Neuroblastoma along with ganglioneuroblastoma and ganglioneuroma constitute a group of tumours of ganglion cell origin that derive from primordial neural crest cells,
which are the precursors of the sympathetic nervous system (14).
Neuroblastoma is the most common solid abdominal mass in infancy and the third most common overall malignancy,
following Leukaemia and CNS tumours in children.
Most children with NBL present between 1 and 5 years of age,
median age 2 years,
with a palpable abdominal mass.
This may be an incidental finding in an otherwise healthy child or in a child clearly unwell from metastatic spread of the tumour (14).
Distant metastatic disease at presentation is encountered in 60%–70% of children with abdominal NBL,
with the most commonly affected sites being the bone marrow,
followed by the lymph nodes,
the liver and skin(14).
Skeletal metastases on radiograph show ill-defined lucencies and aggressive pattern of periosteal reaction.
Sclerotic metastases are uncommon.
(Fig.
17)
Metastatic disease may also be depicted as lucent metaphyseal zones that mimic leukaemic infiltration.
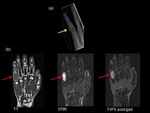
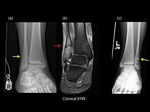
Stress and Insufficiency fractures:
Stress fractures are the result of repetitive forces on the musculoskeletal system that has not had sufficient time to recover (15).
In children,
factors such as weaker osteochondral junctions,
thinner cortices,
hormonal changes,
and decreased mineralization predispose to stress fractures (16).
This is further compounded by participation in sports with demanding schedules which may not allow adequate time for the child to recover.
The physis and the apophysis,
which are among the weaker parts of the bones in children,
are common sites for stress fractures.
(Fig.
18)
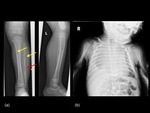
Only 10 to 25% of Stress fractures are visible radiographically at the time of initial presentation.
Positive radiographic findings may lag 2 to 12 weeks behind the onset of pain (17).
(Fig.
19)
On radiograph,
cortical irregularity,cortical resorption and periosteal reaction may be the initial finding.
Cancellous lesions will manifest initially as a line of sclerosis perpendicular to the trabeculae.
Care should be taken not to mistake delayed presentation of stress fractures or healing avulsion injuries for infection or neoplasm as their appearances can overlap.
The characteristic location of stress related injuries and clinical history are helpful in differentiating them from infectious or neoplastic processes (18).
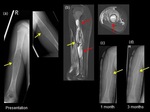
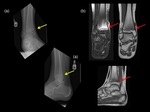
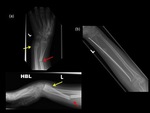
It has been noticed that following immobilization of a lower extremity for a conventional traumatic fracture,
children are more susceptible to developing stress fractures more distally in the same leg.(19) (Fig.
20)
Insufficiency fractures occur as a result of normal or physiological stresses on abnormal or weakened bone.
Insufficiency fractures often occur in children with osteoporosis (Fig 21) of varied aetiology,
those with osteogenesis imperfecta or other metabolic derangments.
Also known as “brittle bone disease”,
Osteogenesis Imperfecta (OI) is a genetic disorder characterised by increased bone fragility and low bone mass density due to quantitative and/or qualitative abnormalities of type I collagen (20).
The main radiographic features are osteopenia,
bone fractures and bone deformities.(Fig.
22) Non-accidental Injury (NAI) should always be considered in the differential diagnosis and can be difficult to distinguish in mild forms of OI.
Other disorders such as copper deficiency,
Menkes disease (a genetic disorder of copper metabolism,
also known as kinky hair disease),
scurvy and vitamin D deficiency rickets may also cause diagnostic difficulties in children with unexplained fractures.
In copper deficiency and Menkes disease,
fractures are usually noted within the first 6 months of life; they are associated with hypopigmented,
and brittle hair and progressive neurologic deterioration in Menkes disease (21).
Typical radiographic findings include osteopenia,
bone age retardation,
increased density of the provisional zone of calcification and symmetrically distributed metaphyseal abnormalities (cupping and fraying).
In scurvy,
there is no cupping or fraying of the metaphyses,
but radiography shows evidence of radiolucent metaphyseal bands beneath the increased density of the provisional zone of calcification and/or periosteal reaction (21).
In rickets,
metaphyseal abnormalities similar to copper deficiency are seen on radiographs but with decreased density of the provisional zone of calcification and increased width of the growth plate (21).