Imaging Findings
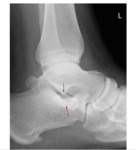
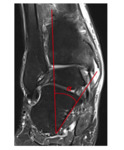
In patients with lateral hindfoot impingement plain radiographs may reveal bony contact between the lateral calcaneus and talus as well as sclerosis or cystic changes (figure 2).
Based on findings on plain radiographs,
in the context of clinical history and physical examination findings,
a CT scan or MRI can be ordered to help narrow the differential for etiology of symptoms.
CT scans can better identify cystic changes and sclerosis iwhen compared to plain radiographs.
In patients with calcaneal malunion,
CT scan reconstructed images are useful for determining the type of the malunion,
degree of degenerative changes in the subtalar joint,
the size and location of the lateral calcaneal exostosis and its relation to the lateral malleolus as well as the amount of bone resection necessary.
MRI can reveal morphologic alterations in the bones and soft tissues,
or direct contact at the opposing surfaces of the fibula and calcaneus (table 1).
Cystic changes,
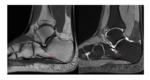
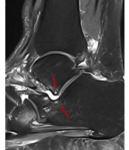
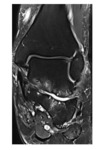
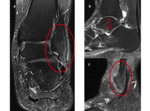
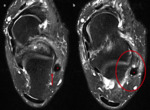
bone marrow edema and sclerosis at the angle of Gissane can be seen in the talocalcaneal impingement (figure 3,
4,
5).
Also the presence of hinfoot valgus (measured on the most posterior coronal image that includes both tibia and calcaneus) can also be seen and is graded as mild (7-16°),
moderate (17-26°) and severe (> 26°) (figure 6). As the MR images are not obtained during weight-bearing,
the measurement of the hindfoot valgus angle may underestimate the functional malalignment.
Furthermore,
the presence of a “neofacet” in the extraarticular anterosuperior aspect of the calcaneus (at the sinus tarsi level) can sometimes be seen in the more advanced cases,
associated with cortical remodelling due to mechanical overload in the inferior apex of the lateral talar process subsequent to talocalcaneal subluxation (figure 7,8).
Imaging features of subfibular impingement include extensive lateral soft-tissue thickening,
between the fibula and the calcaneus.
This thickening may be related to entrapment of fat and the calcaneofibular ligament between the two bones,
leading to fatty atrophy and fibrosis. The peroneus longus and brevis tendons pass directly beneath the tip of the fibula,
which can result in these tendons being also pinched between the two bones.
Furthermore,
multiple anatomical structures attach to the sinus tarsi region,
including the extensor digitorum brevis,
inferior extensor retinaculum,
cervical ligament,
calcaneonavicular ligament,
and calcaneocuboid ligament.
All these structures may be at risk for soft-tissue impingement as the talus,
calcaneus,
and fibula move closer to each other in the flatfoot.
Marrow edema in the distal tip of the fibula has also been reported,
though it is important to distinguish this from marrow edema resulting from fibular stress fractures.
In later stages osseous changes,
including subcortical cysts,
sclerosis,
and bony abutment can be seen.
In all cases there is hindfoot valgus malalignment,
as it is a requisite for the development of lateral hindfoot impingment.
Differential Diagnosis
The main imaging differential diagnosis for lateral hindfoot impingement is sinus tarsi syndrome.
It can be difficult to separate findings of sinus tarsi syndrome from those of lateral hindfoot impingement,
and some authors consider these to represent aspects of the same lateral subtalar impingement pathology.
The characteristic findings of sinus tarsi syndrome have been described as diffuse edema throughout the sinus tarsi,
sometimes with mild bone marrow edema extending along the subcortical region around the sinus tarsi,
also with indistinctness compatible with degeneration and scarring at the cervical and interosseous ligaments.
Marginal erosions associated with reumathoid arthritis may also mimic the bony changes of lateral hindfoot impingement but erosions and synovitis are generally also present elsewhere,
clarifying the diagnosis.
Also,
there is increased incidence of hindfoot valgus collapse in individuals with inflammatory arthropathy,
including rheumatoid arthritis and psoriatic arthropathy,
related to a higher risk of tibialis posterior tendon tear related to long-standing inflammation at the tendon sheath and adjacent joints.
Calcaneal intraosseous ganglion formation or prominence of vascular structures may mimic the calcaneal changes of lateral hindfoot impingement,
but no osseous abnormalities would be expected at the adjacent lateral talar process.
Treatment
Early detection of lateral hindfoot impingement has been demonstrated to improve patient outcome.
Treatment of subfibular impingement is aimed at halting the progression of deformity to prevent additional disability.
Early in the course of disease,
conservative treatment including rest,
nonsteroidal anti-inflammatory medications and activity modification,
physical therapy,
bracing,
and orthotics can be used to reduce the pain associated with synovitis.
Since symptoms often persist due to the difficulty to stabilize a valgus deformity of the hindfoot with conservative measures such as medial wedge inlays or orthotics, surgery is usually indicated.
Calcaneal osteotomy is usually required and may provide hindfoot realigment without the restriction of movement of a fusion.
Alternatively,
triple artrhodesis may be required to realign and provide pain free stability.