Keywords:
Musculoskeletal joint, Musculoskeletal system, MR, MR-Diffusion/Perfusion, Diagnostic procedure, Inflammation
Authors:
S. Ciuk1, I. Kucybała2, W. Wojciechowski3, A. Urbanik3; 1Wroclaw/PL, 2Cracow/PL, 3Krakow/PL
DOI:
10.26044/essr2019/P-0177
Results
Characteristic of the group
In general,
46.9% (n=23) of the study group fulfilled the imaging arm of ASAS axSpA criteria.
There was not any statistically significant difference in age (p=0.195) and gender (p=0.130) between group fulfilling the imaging arm of ASAS axSpA criteria and the group without the diagnosis of axSpA.
Diagnostic performance of DWI/ADC and DCE sequence vs.
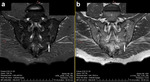
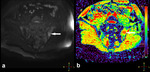
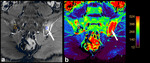
STIR sequence The performance of the visual assessment of DWI sequence combined with ADC map and DCE sequence was compared to the STIR sequence with regard to the detection of active sacroiliitis fulfilling ASAS criteria for axSpA.
DWI sequence with ADC map has slightly higher sensitivity and markedly lower specificity than DCE sequence in the detection of active sacroiliitis.
Accuracy and PPV is slightly higher for DCE sequence than for DWI sequence with ADC,
contrary to the NPV,
which is higher for DWI sequence with ADC map.
Inter-observer agreement
The level of agreement was compared between the both observers.
The highest inter-rater agreement was achieved for STIR sequence,
which was almost perfect (κ=0.888).
The level of agreement was similar both for DWI sequence with ADC map (κ=0.674) and DCE sequence (κ=0.773),
with a slight advantage of the DCE sequence.
Remaining active sacroiliitis symptoms vs.
ASAS axSpA diagnosis
In the last step,
the diagnostic performance of active sacroiliitis additional signs to the identification of patients fulfilling imaging arm of the ASAS axSpA diagnostic criteria was assessed.
Signs of synovitis were present in 18.4% (n=9) of all patients,
capsulitis in 16.3% (n=8) and enthesitis 10.2% (n=5).
Synovitis (34.8% with axSpA vs.
3.8% without; p=0.008) and capsulitis (34.8% with axSpA vs.
0.0% without; p=0.001) were significantly more frequently present in patients with axSpA,
in comparison to the cohort without axSpA.
Similar correlation was not detected for the presence of enthesitis (17.4% with axSpA vs.
3.8% without; p=0.173).
Although all these signs achieved high sensitivity to the identification of patients with axSpA,
the specificity was very poor.