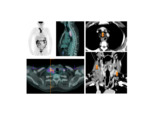
8th edition TNM clinical staging - N-category
A multimodal approach to staging,
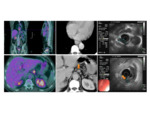
with the combined use of PET–CT and EUS imaging,
allows for a more detailed and accurate assessment of lymph node involvement in patients with esophageal cancer as compared to CT alone.
EUS is used to evaluate size,
shape,
border,
and internal echocardiographic characteristics of regional lymph nodes.
Larger,
more rounded,
well demarcated hypoechoic lymph nodes are most likely to contain metastasis.
In patients with a 60% prevalence of pN+,
using EUS criteria of >5 mm,
round borders,
smooth shape,
and hypoechoic center for cN+,
EUS was only 20% specific for N+,
resulting in overstaging in 80% of pN0 cancers.
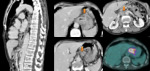
An enlarged lymph node on CT suggests nodal metastasis.
The short axis of nodes is easily measured; intrathoracic and abdominal lymph nodes >1 cm are considered enlarged.
Sources of false-negative examinations are normal-sized nodes that contain metastatic deposits,
and metastatic nodes in direct contact with the cancer that may be indistinguishable from it.
Similarly,
false-positive examinations result from non-malignant nodal enlargement as seen in inflammation.
In a recent review,
CT was 50% sensitive and 83% specific in cN assessment.
Metabolic evaluation of esophageal cancer by FDG PET-CT relies not only on metastatic deposit size but also on intensity of FDG uptake and decay.
Theoretically,
it is possible to identify microscopic metastases if glucose metabolism is sufficient to concentrate large quantities of FDG.
FDG-PET N categorization was 57% sensitive and 85% specific.
Because of its relatively good specificity,
the main role of PET is confirmation of cN0.
Adding CT to FDG-PET increases accuracy,
sensitivity,
specificity,
and negative predictive value (NPV) minimally; however,
its biggest impact is in positive predictive value (PPV),
with an increase from 69% to 82%.
These imaging modalities have remarkably similar performance in cN assessment: accuracy is reported to be 66% for EUS,
63% for CT,
and 68% for PET,
sensitivities 42%,
35%,
and 35%,
respectively,
and specificities 91%,
93%,
and 87%,
respectively.
Pathways of Esophageal Lymphatic Spreading
The upper mediastinal and perigastric areas are the most common areas for lymph node metastasis in EC.
However,
lymph node metastasis in different areas may vary with the location of the primary tumor.
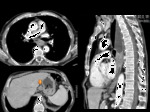
For upper thoracic EC,
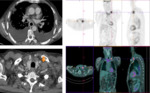
tumor cells usually spread upwards to upper mediastinal (Fig. 4) and cervical nodes(Fig. 5, Fig. 6).
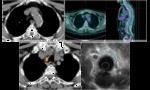
As for middle thoracic EC,
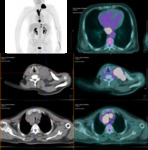
lymphatic flow drains primarily both up and down into the cervical (Fig. 7),
upper mediastinal,
periesophageal and perigastric nodes (Fig. 8)
With regard to lower thoracic EC,
the perigastric area is the most important (Fig. 9,
Fig. 10).
If the tumor reaches the muscularis propria,
the rate of periesophageal lymph node metastasis will increase rapidly for the middle and lower thirds of the mediastinum.
The lymph flow of the thoracic esophagus can both run upward to the neck and downward to the celiac area and allows the development of ‘‘skip’’ metastases to nodes at other levels.
In addition to the location,
the tumor histological type and invasion depth may be worth considering,
well known as influencing factors on the prognosis for EC.
In contrast to esophageal squamous cell carcinoma with lymphatic spreading more widely,
the lymphatic flow of esophageal adenocarcinoma is primarily into the lower posterior mediastinum,
the pericardial region and along the lesser gastric curvature.
Distant metastasis is rarely found.