Congress:
EuroSafe Imaging 2019
Keywords:
Action 2 - Clinical diagnostic reference levels (DRLs), Action 6 - Clinical audit tool for imaging, Action 3 - Image quality assessment based on clinical indications, Radioprotection / Radiation dose, Management, CT, Diagnostic procedure, Quality assurance, Dosimetric comparison
Authors:
H. Brat, M. Hussenot, M. Laurent, V. Leduc, J. Helal, N. Correia, J. Favre, P. Bosson, M. Eric
DOI:
10.26044/esi2019/ESI-0044
Description of activity and work performed
1.
Anticipation of major challenges
Before starting such a project,
anticipation of needs and difficulties are a prerequisite.
- Occupational:
- Allocating resources and time to setup a quality project in a private multicentre setting
- Creating a dose team in each centre to ensure continuous follow-up of an ongoing quality process
- Transforming anatomy-based radiology to patient based specific clinical imaging
- Empowering radiographers towards a more clinical approach
- Defining what is optimum: dose optimization means ALARA (less image quality,
but sufficient for diagnosis)
- Integrating stakeholders such as a MPE and industry
- Levelling up new team members to the local standards
- Technological:
- Implementing a dose management software
- Dealing with CT scanners of different generations
- Automatically integrating dose report in examination report
- Succeed with expansion: Groupe 3r comprised 7 imaging centres with 7 CT scanners of different generation from 3 manufacturers in 2015,
10 centres with 5 new CT scanners in 2018.
- Human:
- Introducing a radiation protection quality project as a primary concern in private practice
- Dealing with resistance to change
- Bringing onboard 22 Radiologists (32 in 2019) of different generations,
from different medical schools,
with different professional routines
- Improving professionalism of 40 Radiographers (>50 in 2019) towards patient-specific imaging.
2.
Initial multicenter CT scanner data analysis
A dose management software (Dosewatch™,
GE,
Milwaukee) was installed to collect data from all scanners and compare practices.
Initial data analysis in Groupe 3r identified:
- large dose variations,
- protocol nomenclature and parameters inhomogeneities,
- lack of staff training uniformity.
This first step supported awareness of strong standardization and optimization needs.
3.
Dose Excellence Program
A. Organization
Based on this initial picture and in order to comply with the European Directive,
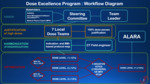
the task-force designed a dose excellence program at the level of the group ( Fig. 1 )
- A steering committee was created in close relation with stakeholders such as a medical physics expert,
CT manufacturers and the Dosewatch experts in order to help us managing the collected data.
- A local dose-team was set-up in each centre,
consisting of a radiologist and a radiographer,
a CT field engineer,
and a physicist.
They were responsible for implementation of standardized protocols,
local dose optimization while maintaining image quality according to CT technology,
local training,
dose record verification,
dose excess investigation and 100% of dose excess justification.
- Workshops ( Fig. 2 ) built a clear vision of the project,
defined by “The right dose for the right diagnosis” ( Fig. 3 ).
B. Implementation
The steering committee implemented a 2-step strategy based on Harmonization and Optimization without impairing the image quality.
Step 1: Protocol Harmonization (June 2015 - January 2016)
- A clinical indication-based protocol map was defined by a senior radiologist with two categories of patients for each protocol according to body mass index (BMI<25 for non-overweight and BMI≥25 for overweight patients) ( Fig. 4 ).
- Each protocol was mapped into a dose monitoring system (DoseWatch®,
GE Healthcare) to the RadLex playbook.
- In parallel,
acquisition and reconstruction parameters were harmonized per clinical indication among CT scanners.
Protocols were adapted to remain close to the Swiss P25 NDRL (5) for BMI<25 patients and the P75 NDRL for BMI>25 patients.
Step 2: Protocol Optimization (January 2016 - January 2017)
- Optimization methodology was based on a 12% step-wise mAs reduction for all protocols with continuous diagnostic-based image quality assessment.
- After 50 examinations of the same indication without negative voting,
an additional 12% of dose reduction was applied.
After 50 examinations of the same indication without negative voting,
an additional 12% of dose reduction was applied.
- In case of 3 negative voting for one type of protocol,
each confirmed by a second reader,
dose was increased back by 12% to reach previous accepted dose level,
representing the “right dose for the right diagnosis” ( Fig. 1 ).
C.
Quality Assurance
- Image quality was assessed using adapted European image quality guidelines (2) through a contextual call in the PACS,
to fit with the clinical workflow and with an electronic image quality voting button in the dose tracking software ,
used by the radiologists during their routine work (binary task,
0 = non-diagnostic image; 1 = diagnostic image) ( Fig. 5 ).
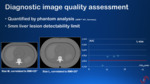
- During both phases,
image quality and low contrast lesion detectability were assessed by our medical physics expert,
using a liver tumour follow-up protocol on an anthropomorphic phantom and a quantification with a CHO model observer (3) ( Fig. 6 ).
D. Results
Protocol Harmonization enabled:
- RadLex mapping
- Elimination of redundant protocols
- Benchmarking of comparable data
- Systematic dose record analysis
- Consensual good practice standardization
- Less dose variations
- Tracking abnormal events
- 100% of dose excess justification
- Increased diagnostic quality
- Less time to plan examination protocols
- More time for image reading and education
- Improving teleradiology
- Maintaining diagnostic image quality
- Reducing dose globally by 6% for chest and 7% for abdomen
Protocol Optimization enabled:
- Significantly lower dose levels than existing DRLs (4)
- Determination of local clinical DRLs
- Additional dose reduction of 26%
- Low contrast resolution limit determined by phantom measurements
- Clinical research ahead of legal requirements
The Dose Excellence Program initiated in 2015 also enabled:
- Access to the Eurosafe Initiative 5* label for each centre of the group
- European leadership in terms of patient-specific dose management
- Fertilizing other quality projects such as patient-specific contrast media optimization
- Driving quality and science in private practice
- Building a corporate culture based on excellence
E.
Pitfalls to avoid
- Lack of Leadership: such a systemic project implementing a dose culture based on “diagnostic image quality” (clinical DRLs) instead of “beauty of images” need a strong leadership
- Lack of communication: regular communication based on project and (intermediate) results explanation in mandatory
- Speeding: let time play its role for human adaptation
- Hearing and discussing the unsatisfaction
- Use of national DRL only for comparison.
They represent national practice but local DRLs represent a better benchmark for optimization.
Local optimization processes are faster and more flexible in order optimize exposure parameters in accordance with local CT technology.
- Protocol harmonization without taking into account technology generation of CT (heterogeneity)
- Don’t rely on image look for optimization (IR make nice images)
- Underdosing: non-diagnostic scan due to excess of dose reduction.
Use a gold standard for IQ (phantom)
F.
Keys to success
- Strong leadership
- A clear roadmap
- Teamwork with team building during kick-off workshops,
empowerment of local dose teams with support from leader and MPE
- Collaboration between radiologists,
radiographers,
medical physics experts and industry
- Quality insurance with prospective diagnostic image quality evaluation and phantom measurements
- Follow-up meetings after each step of harmonization and optimization,
seeking consensus in order to adopt best practice protocols and homogenize dose per clinical indication
- Dashboards to present results of harmonization and optimization steps
- Communication adapted to audience (radiologists,
radiographers),
repeating expectations and benefits,
using informative and educative tools
- Recognition by scientific organizations: Eurosafe 5* status,
abstract presentations,
publications.