Institution
As the largest provider of health services in Turkey,
the Ministry of Health is segmented into multiple hospital associations including the 2nd Healthcare Region of Istanbul Province (a.k.a. Anatolia North, which consists of 13 hospitals and 6 dental hospitals/centers.
In Anatolia North 3 million residents are being served; 11.1 millions outpatient admissions and 250 thousands surgical operations are being performed annually.
The annual number of radiologic procedures in Anatolia North are more than 4 milion and roughly represents 1/1.000th of world radiological services.
FSM is a mid-size receiver hospital.
Although it is serving to a core population of circa 400.000,
many patients from oether hospitals and districs also prefer or are referred to this institutuion.
FSM was determined as the pilot (model) site within the larger Anatolia North’s radiology organization,
in which people can develop,
practice and improve the components of the high-performance clinical,
operational and financial radiology management models through outcome-based experiments. The facility is a center that has been acknowledged for its supreme operational efficiency.
To give an example,
FSM was performing much above international benchmarks on CT with 94% room utilization,
2x higher scan volumes,
and 99.47% uptime performance rate.
Annual number of CT examinations have exceeded 100.000 in 2008 ( Fig. 4 )
Why to Establish a Dose Excellence Center?
FSM Hospital,
on that context, was the first institution in Turkey,
where a comprehensive dose management system was implemented,
and modern dose surveillance IT applications were used. FSM was designed to comply with highest standards and provide a framework to assist other centers develop the required dose management infrastructures according to relevant IAEA guidelines (6).
Such center of competence (CoC) was required in order to be utilized as initial host institution for fellows that need to be trained within the Anatolia North,
and to be a reference center that other hospitals in Turkey can duplicate in order to develop quality assurance practices.
The compliance of the facility with the established criteria was verified through a process of systematic and critical analysis of the quality of radiological services to allow comparison of trainees/observers’ practices of service against established standards of good practice.
Basic Guidelines and Criteria for CoC
The facility fulfills all the guidelines and criteria set by IAEA to establish for regional Centers of Competence for QA/QC in diagnostic and interventional radiology (6).
Accordingly,
(1) objective of the facility; (2) access to institutional/industry funds for the sustainability; (3) infrastructure, i.e. technical (equipment) resources,
inventory control (asset management system), number of examinations and procedures (demand) to correspond to the scope of the facility to be a centre of professional education and training regarding the establishment of quality assurance/quality control in radiology; (4) human resources,
and (5) quality processes were set to support the duty explained above.
Key Elements of a Dose Excellence System
Lowering dose requires more than technology.
An effective dose management approach requires a wing to wing approach from the justification of the examination (i.e.
performing the appropriate procedure) to the optimization of the exposure (i.e.
performing the procedure appropriately) (7) ( Fig. 2 ).
In that context,
basic steps and goals of a dose management strategy are as follows:
- Transforme dose awareness from an act to a habit
- Educate personnel
- Justify high dose examinations
- Standardize protocols and practices
- Optimize protocols and practices
- Communicate message to stakeholders
- Promote best practices and be safe
To meet above mentioned goals FSM (or any CoC) has to have below mentioned infrasturucture and proceses ( Fig. 2 ):
- Access to prior exams: FSM has access to patient’s past radiological exams through national teleradiology system,
connectiing all Turkish hospitals,
public and private.
- Appropriateness: Electronical clinical decision support system, embedded in hospital information to assist referring physicians in selecting the most appropriate examination based on the patient’s clinical presentation. This ensuresthat patients are referred for the “right” imaging study, prevent over-utilisation of imaging,
and will prevent unnecessary exposures.
- Eqipment quality: All CT equipment should meet XR-29 lower dose criteria. Availability of modern dose reduction algoritms (i.e.
statistical iterative reconstruction) is preferred.
- Standardization: Mapping local imaging procedures with standard procedures to obtain uniform scanning and facilitate data analysis.
This step includes the asignement to site protocols a specific ID.
(i.e.
RadLex v.1.2).
In FSM, 65 standartized protocols are currently used. The use of nonstandartized protocols are not permitted,
unless clearly justified and only exceptionally.
Standardization allows to compare protocols/technologies/radiographers,
and assists in tracking of examinations and in making comparisons between same protocols of same CT systems.
Development and implementation of standardized imaging has also been shown to lead to better results by means of quality imaging and high patient throughput.
- Continuous education: (1) Technologists orientation training programs to deliver imaging quality training solutions to contribute the transformation in radiology department to shift technicians autonomy from the individual to the professional level.
(2) Technical conferences and workshops to apply advanced capabilities of devices into practice making the full use of the systems.
- Centrally managing and tracking compliance to standartized imagingprotocols: An essential component of protocol management,
a feature embedded dose tracking software.
- Availability of diagnostic reference levels (DRLs):These are values which are usually easy to measure and have a direct link with patient doses.
They are therefore established to aid efficient dose management and to optimize patient doses.
DRLs should not to be exceeded for standard procedures when good and normal practice is performed.
If patient doses are found to exceed consistently the corresponding reference level,
investigation and appropriate corrective action should be taken,
unless the unusually high doses could be clinically or technically justified.
As a part of proper radiation protection program,
and according to Radiation Protection 109 (EC 1999),
Guidance on Diagnostic Reference Levels (DRLs) for Medical Exposures (8),
these levels should be established,
have to be revised periodically,
and be specific to a country or to a region because published DRLs values from other countries (with potentially different imaging practices and technology) may not be relevant to other countries’ particular circumstances.
For Turkey,
these levels were not established,
and Anatolia North’s median DRLs are generally used to fulfill the gap.
For Anatolia North itself,
and for FSM in particular unified pan-European DRLs of our CT service provider,
Affidea was initially used.
These were determined afer median DRLs published from several European countries (Switzerland,
Belgium,
Finland,
Norway,
France,
Germany,
Poland,
UK) from 2010 onwards (9).
- Dose data acquisition,
registry and analysis system: In FSM a commercial software(Dosewatch,
GEHC) is being used.
This web-based vendor-neutral solution captures,
tracks and reports radiation dose directly from the medical devices.
It monitors and analyzes high dose alerts and patient cumulative dose,
includes quality metrics to assess the technical factors,
has data consolidation and statistical analysis tools for protocol optimization and dose reduction by optimizing dose levels.
In that system if the DLP or CTDIvol for a scan is equal or more than [median x 2],
an alert is triggered.
Alert thresholds are moving targets; so as technicians got better,
dose thresholds become tighter.
- Justificaton: Cases for whom overdose alert is triggered had to be justified on the dose tracking software by responsible technician to assist finding root causes of overdoses.
These justifications might point to patient-related (e.g. obesity, incooperative movements),
technician related (e.g.
choosing wrong protocol,
por iso-centering),
or procedure related (e.g.
difficult procedure,
over-length scanning) factors.
- Systematic image quality assessment:FSM has an embedded module in its teleradiology system,
allowing radiologists to evaluate the image quality.
Quality scores are tracked on-lineto maintain balance between low doses and clinically useful image quality.
- Periodical assessments: Meetings to assess the standartization,
justification and optimization goals.
These meetings also permit detection and retrospective evaluation of severe over-exposures to be analysed by experts in the presence of responsible technologists.
- Optimization: Distances of hospital DLPs to the initial DRLs (unified pan- European DRLs) that were determined after published data from several European countries (Switzerland,
Belgium,
Finland,
Norway,
France,
Germany,
Poland,
UK) from 2010 onwards (9).
- Patient education: Posters,
banners,
booklets and audiovisual materials on dose-awareness to be disseminated at imaging facilities.
- Creating public awareness: Generated a lot of interest across the Anatolia North,
nationally broadcasted through TVs,
and found place in social media and national press.
This interest has created a dose awareness throughout the country.
- Internal/independent audits: To measure current state,
identify process gaps and areas to bring more optimization.
Dose Optimization Achievements
For current dose levels,
data set was from 01.01.2018 to 17.12.2018.
In that period , 102.160 individual standartized sequences for adults covering wide range of clinical indications were available to analysis.
The sequences were acquired with a 128-slices scanner that had statistical iterative reconstruction algorithms,
and we have calculated DRLs for this scanner before successful implementation of dose management sytsem and after subsequent dose optimization.
All patients were measured for length and weight before the study.
For pediatric patients Broselow-Luten System for color coded protocols was used where appropriate (10).
This procedure was necessary to calculate size specific dose estimates (SSDE) and to perform size-based CT dose optimization (11).
Conventional dose data (CTDIvol and Dose Length Product) were recorded or calculated.
Basic dose statistics based on protocol (DLP,
minimum,
P25,
mean,
P75,
maximum), were automatically determined using all available patients. Detailed dose information such as SSDE,
effective dose,
and detailed protocol parameters were also recorded or calculated. Off isocenter shift to identify how the patient was positioned in the bore of the CT and mA modulation to visually observe how dose was optimized along the patient scan length were also presented graphically and observed to determine the optimality of technical parameters.
The current paper simplifies the study,
and aims to provide the existing CT dose levels for five basic and most used protocols (i.e. Abdomen/pelvis follow up max 1 phase,
RPID 860; General head helical,
RPID 213; Lumbar spine herniation helical,
RPID 1527; Renal stone,
RPID 343; Chest follow-up,
RPID 16).
Dose levels before (01.05.2015 to 01.08.2015,
N=5.283 exams) and after optimization (01.01.2018 to 17.12.2018,
N=89.587 exams) were presented.
Before and after optimization comparisons with unified pan-European DRLs were made.
During preoptimization period,
all doses were significantly higher than pan-European unified DRLs.
Same protocol was used for different purposes; hence unoptimised dose levels (i.e.
high median doses with large variability) and inconsistent image quality (as reported by radiologist from IQ feedback module of teleradiology system) were common to observe.
After appropriate trainings and technical optimizations by vendors, physicists and radiologists median and standard deviations improved significantly.
For five basic protocolsmedian dose levels decreased significantly below unified DRLs and standard deviations dropped 2 to 6 fold ( Fig. 5 ).
To give an example,
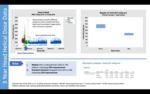
median DLP (mGy.cm) for head protocol was 1246±337 during preoptimization,
and improved to 724±158 after the optimization.
These values represent an improvement of 42% in median dose level and an improvement of 53% in standart deviation ( Fig. 6 ).
Similar improvements were observed for all remaining protocols. For example, median DLP (mGy.cm) for thorax protocol was 291±647 during preoptimization,
and improved to 168±82 after the optimization.
These values represent an improvement of 42% in median dose level and an improvement of 87% in standart deviation ( Fig. 7 ).
The most important observation was the sutainability of the improvements over three years.