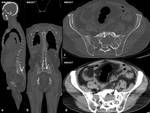
In the study were included patients with MM diagnosed (were selected patients in the third stage of the disease,
known with plasmacytomas confirmed by biopsy,
symptomatic and during treatment,
at which imaging controls are performed at about 6-12 months) who were evaluated by WBLDCT exam,
in a single spiral acquisition covered the skull to the femoral bones,
followed by processing in sagittal and coronal reconstructions in a bone and soft tissue windows and of course,
image analysis.
Issues
Typical features of MM were analyzed on WBLDCT images and qualitatively compared with the standard CT findings in order to define the most important potential ways of increasing accuracy (2).
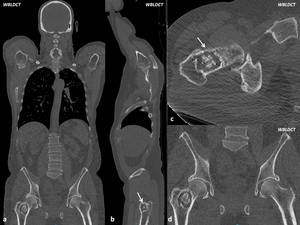
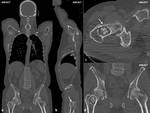
Fig. 1: Male, 67 yo. Lytic lesion (arrows) with osteoclerotic center and ring developed on right femoral neck. DLP: 394 mGy*cm.
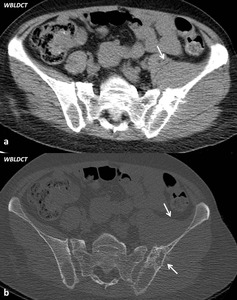
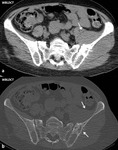
Fig. 2: Female, 59 yo. A bulky tissue mass developed in the thickness of the iliac, middle gluteal and left spinal erector muscles (arrows), associating bone destruction in the left iliac wing. DLP: 920 mGy*cm.
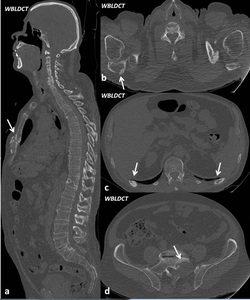
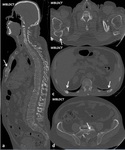
Fig. 3: Male, 66 yo. Numerous lytic lesions with bone destruction associated, having the following topography: at the right scapula, at the sternal manubrious with fracture associated, in the IX and XI right posterior costal arches, respectively, at the IX-XI left posterior costal arches and at the vertebral bodies, the most significant being the osteolytic lesion from the L5 vertebral body with extension to the medullary canal and at the left sacral wing. DLP: 416 mGy*cm.
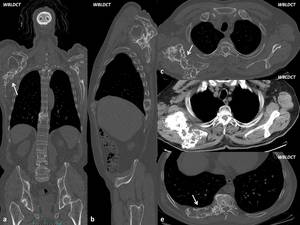
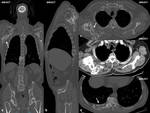
Fig. 4: Male, 63 yo. Myeloma tumorous lesions developed to the right scapula and to the X right posterior costal arch extended to 10 thoracic vertebra. DLP: 502 mGy*cm.
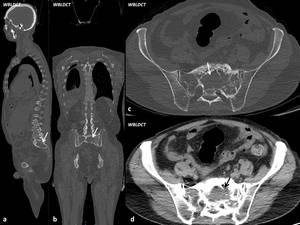
Fig. 5: Male, 65yo. Myelomatous lesion developed at S1-S3 vertebrae extended in the anterior sacral holes, as well as in the left iliac wing. DLP: 449 mGy*cm.
Discussions
Conventional CT gives an improved sensitivity in detecting lytic lesions,
especially the small one (<5 mm that can be missed on x-ray),
offers a high resolution three-dimensional CT images that can provide a detailed evaluation of the bone,
allows a good visualising soft tissue involvement,
assess spinal fracture stability,
can detect spinal cord and cauda equina compression (although MRI is superior for this),
is useful in guiding needle biopsies and surgical interventions and also in planning radiotherapy.
Despite a number of advantages,
conventional CT uses higher doses of radiation (from 920-3080 mGy in these cases for CT of the head,
neck,
chest,
abdomen and pelvis).
For this reason,
WBLDCT has begun to be the most widely used imaging method in patients diagnosed with MM,
because uses a lower tube voltage (kV) and current (mAS) to reduce the energy delivered to the patient to an effective dose of approximately 320-1038 mGy (in the cases from this study).
The reduction of the dose comes with a reduced image resolution,
but this can be partly offset by reconstruction techniques so that WBLDCT can now be performed at a similar dose to skeletal survey.
So nowadays,
the European Myeloma Network guidelines recommend as first-line imaging investigation the WBLDCT,
because this method accurately assess the extent of bone destruction and remains more sensitive than plain x-rays.
Recommendations
WBLDCT is recommended:
- like an alternative to bone skeletal assessment (where facilities exist);
- in the initial screening of lytic lesions in MM;
- in demonstrating extramedullary disease (although MRI is superior for this);
- if the MRI examination is not feasible,
for evaluating patients with suspicion of MM that remain symptomatic despite the fact that no lytic lesion has been identified in WBRX;
- to clarify the results of ambiguous radiological examinations such as fractures,
medullary compression,
or lytic lesions,
especially in parts of the skeleton that are difficult to visualize on the plain x-rays,
such as the sternum and the scapula,
or to delimit the nature and extent of soft parts lesions;
- in patients with unsupported MRI metallic implants;
Advantages
The advantages of WBLDCT are the following:
- detects small lytic bone lesions;
- reveals soft lesions;
- allows estimation of fracture risk and fracture outcomes;
- excellent in radiotherapy planning,
as well as in surgical therapy.
Limits
As limitations of WBLDCT must also be recognized the following:
- reduced detection of lytic lesions in patients with marked osteopenia;
- can not make appreciations about the morphology and structure of the medullary cord and spinal roots;
Protocol
Low dose CT is given without IV contrast,
and its a unique spiral acquisition including the skull,
cervical compartment,
the thoracic,
abdominal and pelvic regions,
proximal humerus,
and femoral bones,
with a field of view (FOV) set at about 400 mm (adjusted to individual patients during examination planning).
The diagnostic images can be achieved with parameters such as 120 kV,
<70-90 mAs,
dose modulation,
and iterative reconstruction.
Slice thickness was set at 1mm and slice increment at 0.8mm (slice increment smaller than thickness was used to avoid step artifacts on secondary coronal/sagittal reconstructions).
Two sets of axial images were reconstructed from the raw data obtained during scanning: for bone assessment using sharp kernel and for soft tissue assessment using soft kernel.
From every set of axial images,
secondary coronal and sagittal reconstructions were generated using slice thickness of 1mm and slice increment of 1mm.
WBLDCT features
Typical aspects of bone structures in MM:
- lytic bone lesion,with osteosclerotic ring or cortical damage (Fig.1);
- important areas of bone destruction (Fig.2);
- osteopenia;
- extraosseous involvement.
Structured report
The outcome of the WBLDCT examination should contain the following information:
- the topography of lesions;
- number of lesions to determine the stage of the disease (if it’s the first imagistic exam);
- the semiological features of the lesion;
- the locoregional extension of the lesion process;
- the complications of lesions (if they associate medullary or radicular compression,
fractures).