Bonn Call For Action:10 proposed actions
Note the ICRP publications and task groups (TG) that may contribute to the Bonn Call For Action items.
The bolded items are the focus of further focused discussion after a general introduction of the work of ICRP.
- Enhance the implementation of the principle of justification (P84,
P103,
P105)
- Enhance the implementation of the principle of optimization of protection and safety (P84,
P102,
P107,
P120,
P121,
P127,
P128,
P129,
P135,
TG108)
- Strengthen manufacturers’ role in contributing to the overall safety regime
- Strengthen radiation protection education and training of health professionals (P113,
P139)
- Shape and promote a strategic research agenda for radiation protection in medicine (P118,
TG111)
- Increase availability of improved global information on medical exposures and occupational exposures in medicine (P135,
P139,
TG36,
TG89,
TG101)
- Improve prevention of medical radiation incidents and accidents (P112,
P127)
- Strengthen radiation safety culture in health care (P138)
- Foster an improved radiation benefit-risk-dialogue (ICRPaedia)
- Strengthen the implementation of safety requirements globally
Our values in our Code of Ethics ( http://www.icrp.org/admin/ICRP%20Code%20of%20Ethics.pdf) include:
http://www.icrp.org/admin/ICRP%20Code%20of%20Ethics.pdf) include:
-A Commitment to Public Benefit:
ICRP acts to protect humans and the environment from the harmful effects of radiation
-Independence:
ICRP acts independently of governments and organisations,
including industry and other users of radiation
-Impartiality:
ICRP acts impartially in its development of recommendations and guidance
-Transparency:
ICRP engages stakeholders and strives to be transparent in its actions and judgements
-Accountability:
ICRP is accountable to the framework that governs the activities of a charity
Each of these values has statements describing examples of what it means to act to fulfill them.
Further the guidance policies and programs as well as the liaison outreach that the ICRP carries out furthers its mission as described below.
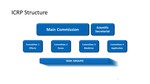
We focus on the Committee on Medicine.
Committee 3,
Medicine: What we Are Doing To Further the Bonn Call For Action
Each ICRP committee is responsible for a work packet that produces task groups,
documents published in the Annals of the ICRP,
and other publications.
These task groups may meet with other scientific and medical bodies to seek input to develop their reports.
[BCA Actions 8 and 10] Further,
the committee invites special liaison organizations (SLOs) to attend their annual meetings.
The SLOs are also invited to an annual meeting for shared radiation protection discussions and the biennial ICRP symposia [see slide for Adelaide symposium].
ICRP C3 members liaise with a number of medical and medical physics organisations in Europe to strengthen radiology and radiation oncology RP guidance.
To promote an inclusive web site for all stakeholders,
the ICRP has launched ICRPaedia [http://www.icrpaedia.org/index.php/Main_Page] to provide lay language materials regarding ionizing radiation information on medicine and other sources [BCA Action 9].
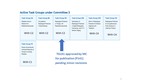
To provide guidance on the medical imaging and radiation therapy radiation protection of the patient,
the worker,
and the public,
committee 3 is currently working on a number of task groups and working parties.
In addition there are 2 recent publications with a wealth of practical information that may be applied across the range of resource-heavy or resource-limited situations.
The first is publication 135 ‘Diagnostic Reference Levels in Medical Imaging’ (2018),
which advances our understanding of the role of diagnostic reference values (DRLs) and how to go about their development and ongoing updates for them for imaging optimisation.
Abstract: The International Commission on Radiological Protection (ICRP) first introduced the term ‘diagnostic reference level’ (DRL) in 1996 in Publication 73.
The concept was subsequently developed further,
and practical guidance was provided in 2001.
The DRL has been proven to be an effective tool that aids in optimisation of protection in the medical exposure of patients for diagnostic and interventional procedures.
However,
with time,
it has become evident that additional advice is needed.
There are issues related to definitions of the terms used in previous guidance,
determination of the values for DRLs,
the appropriate interval for reevaluating and updating these values,
appropriate use of DRLs in clinical practice,
methods for practical application of DRLs,
and application of the DRL concept to newer imaging technologies.
This publication is intended as a further source of information and guidance on these issues.
Some terminology has been clarified.
In addition,
this publication recommends quantities for use as DRLs for various imaging modalities,
and provides information on the use of DRLs for interventional procedures and in paediatric imaging.
It suggests modifications in the conduct of DRL surveys that take advantage of automated reporting of radiation-dose-related uantities,
and highlights the importance of including information on DRLs in training programmes for healthcare workers.
The target audience for this publication is national,
regional,
and local authorities; professional societies; and facilities that use ionising radiation for medical purposes,
and responsible staff within these facilities.
A full set of the Commission’s recommendations is provided.
The second publication is P139 ‘Occupational radiological protection in interventional procedures’ (2018) which provides practical guidance and rationale behind its statements for interventional fluoroscopy and cone beam CT.
Abstract: In recent publications,
such as Publications 117 and 120,
the Commission provided practical advice for physicians and other healthcare personnel on measures to protect their patients and themselves during interventional procedures.
These measures can only be effective if they are encompassed by a framework of radiological protection elements,
and by the availability of professionals with responsibilities in radiological protection.
This framework includes a radiological protection programme with a strategy for exposure monitoring,
protective garments,
education and training,
and quality assurance of the programme implementation.
Professionals with responsibilities in occupational radiological protection for interventional procedures include: medical physicists; radiological protection specialists; personnel working in dosimetry services; clinical applications support personnel from the suppliers and maintenance companies; staff engaged in training,
standardisation of equipment,
and procedures; staff responsible for occupational health; hospital administrators responsible for providing financial support; and professional bodies and regulators.
This publication addresses these elements and these audiences,
and provides advice on specific issues,
such as assessment of effective dose from dosimeter readings when an apron is worn,
estimation of exposure of the lens of the eye (with and without protective eyewear),
extremity monitoring,
selection and testing of protective garments,
and auditing the interventional procedures when occupational doses are unusually high or low (the latter meaning that the dosimeter may not have been worn).