The 3-point ID check and examination confirmation is performed prior to scanning by the radiographer. It is hospital policy to correctly identify a patient prior to any exam or procedure using at least 3 points of information. Generally, it is confirmed by asking the parent or guardian to state the patient’s name, address and date of birth. This ensures the correct patient is present and has been referred for an appropriate CT exam, and the proper age / weight matched protocol is being applied.
After the scan has been completed, the radiographer completes the LDRL check. The LDRL check compares the dose length product (DLP) of the performed CT examination against the established LDRLs.
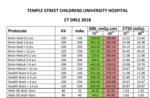
In this CT department, LDRLs are produced and reviewed annually, based on audits performed within the department. These audits review the DLP’s from CT examination undertaken in the previous 12 months. They are broken into exam type and then further by patient age or weight. Following national guidelines [1], the 75th and 90th percentile for each aged / weight-based protocol are established. Upon approval from the local Radiation Safety Committee, there are then used as the LDRLs (Figure 2).
These LDRLs are available within the CT Dept. Once the scan is complete, the radiographer compares the resulting DLP with its equivalent LDRL. If the 75th percentile is exceeded, the performing radiographer must provide an explanation. Common justified explanations include increasing of scan range due to patient pathology or size.
If the 90th percentile is exceeded, the medical physics team and the CT clinical specialist radiographer are also informed for monitoring and audit purposes. This process ensures early identification of any potential technical issues which may results in a higher than intended ionising radiation exposure.
Once the checklist has been completed, it is recorded against the patient’s examination on RIS. This facilitates the audit process.
Audits are carried out regularly to evaluate compliance with checklist recording and the use of the LDRL check.
Previous audits identified issues with checklist recording compliance. The two biggest contributory factors identified for this were a lack of scanning facilities in the CT console room and time pressures experienced by radiographers. A paper scanner was sourced for the CT console room in 2018 and in 2019 a Radiography Assistant took responsibility to ensure all checklists were recorded on RIS. In Figure 3, improved compliance with checklist recording is demonstrated for the first half of 2019 following the introduction of the paper scanner. A further increase is demonstrated in the second half of 2019, following the introduction of support from the Radiography Assistant. In order to improve compliance further, staff are regularly reminded of the role of the CT safety checklist and actively encouraged to complete the checklist.
The checklists also facilitate easy audit of the LDRL process. Figure 4 demonstrates audit results regarding exceeded LDRLs. In all cases where a LDRL was exceeded, the performing radiographer provided a justified explanation.
However, in the 2019 (Q1 & Q2) audit the LDRL check was not completed for 4% of checklists. This potentially results from a lack of understanding of the role and significance of LDRLs. A brief educational session was held with the CT radiography team to explain the role of LDRLs and their significance in the CT department. In the most recent audit, the LDRL check was completed for all checklists recorded.