The majority of the Cerebral Embolisation procedures carried out at our hospital are performed on a bi-plane Azurion Clarity IQ (Philips) system, also used for our phantom study. Three elliptic cylinder shaped polymethyl methacrylate (PMMA) phantoms of increasing size were used to simulate the patient body and standard 20 cm PMMA plates were positioned alongside to represent the hips and top of the thighs. The radiation protection drape used in this study was the RADPAD® Femoral Entry Angiography Shield, which is used during cerebral embolisation in the department.
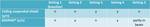
Scattered air kerma was measured using a Raysafe X2 survey meter (Unfors RaySafe AB, Billdal, Sweeden), approximately at the operator position in five different settings listed in Table 1.
Our baseline measurements, against which most others were compared, were performed under setting 1 without any protective equipment. Separate measurements were performed with the RADPAD® only (setting 2), the ceiling suspended shield only (setting 3), and with both RADPAD® and ceiling suspended shield (setting 4). Finally, measurements were performed with the RADPAD® partly in the beam without the suspended shield (setting 5).
Two phantom geometries were used to represent the working projections used during the majority of the procedures (geometry 1a and 1b, Figure 1 and Figure 2 respectively) as well as the initial catheter insertion into the femoral artery (geometry 2, Figure 3). Geometry 1a and 1b represent different patient scatter conditions where geometry 1b is mimicking a higher scatter air kerma rate situation with a larger part of the PMMA in the beam.
The examination protocol used clinically for Cerebral Embolisation procedures was also used to expose the phantoms. Both C-arms were positioned at a 90° angle to each other (frontal C-arm at RAO 0°, CRA 0°) and the most clinically used field sizes of 42 cm for the frontal and 22 cm for the lateral tube were chosen. The phantoms were exposed in both fluoroscopy and acquisition modes, repeating measurements three times for each setting.
Measurements were then analysed and statistical significance was evaluated with two-sample t-test (p-value<0.01 considered statistically significant).
The results from scatter air kerma rate reduction measurements are summarised in Table 2.
All percentage changes for fluoroscopy and acquisition modes were the same for the particular geometries and settings considered, so only one result is presented in Table 2 for each situation.
The presence of the RADPAD® only (setting 2) led to a scatter air kerma rate reduction between 5% (p<0.001) and 13% (p<0.0002) in geometry 1a and geometry 1b respectively.
The presence of the ceiling suspended shield only led to an 88% of air kerma rate reduction (p<0.00001), while both RADPAD® and ceiling suspended shield led to an 89% dose saving (p<0.00003) in geometry 1a.
The percentage change between cases using the ceiling shield only versus ceiling shield and RADPAD® was also analysed and resulted in another statistically significant reduction of 6% (p<0.0005).
Finally, the presence of the RADPAD® in the primary beam (setting 5, geometry 2) led to a non-statistically significant scatter air kerma rate increase of 3% (p<0.06), due to the increased air kerma rate after positioning the highly attenuating shield in the beam. Clinically, this condition is used during the initial catheter insertion which takes a few seconds and is therefore not expected to make a significant contribution to staff doses.