Results
8.16% (59/723) of the total number of images met all qualitative diagnostic requirements, without MinFS truncations or exposure beyond tolerance.
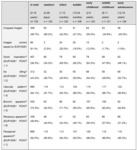
Quantitative analysis showed mean overexposure of 43±17%, and mean tissue overexposure of 38±16% in relation to the MinFS (Table 2). Observed mean distances from respective MinFS edges to their AEA borders were 20±12mm for cervical, 10±8mm for lateral and 9±22mm for abdominal respectively. The mean abdominal distance in relation to MinFS turned out to be negative with -1.2±8.6mm in the newborns sub group. Regression analysis was performed to evaluate the impact of patient age on the relative overexposure. For lateral tissue overexposure % (F(1, 362) = 59.935, p = .00) each year in age resulted in an increase of the relative lateral tissue overexposure by 1% (R2 = 0,14, f = .41). 49.7% (359/723) of all images showed field size truncations disabling field size computations. All images with truncated MinFS had diagnostic field sizes. Sinuses were cropped in 4.14% of all images. Sinuses were increasingly cropped with age, ranging from 0% in newborns, and 2.5% in infants up to 9.3% for patients in their early adolescence.
Qualitative analysis showed that criteria were met in 9.1% (66/723) of all examinations (Table 3). Good inspiration was found in 56.3% (407/723) of cases. 43.2% (312/723) didn’t show signs of tilting and/or rotation. The vascular pattern in the central halves of the lungs was visible in 94.1% (680/723) of all images. The upper airways were apparent in 73.3% (530/723) of the cases. Sharp diaphragms and costophrenic angles could be observed in 46.9% (339//723) of all images. 92.5% (660/723) showed a good representation of the spine and paraspinal structures, as well as the retro cardiac mediastinum.
Agreement: An inter-rater reliability (k = 0.72) , and intra-observer agreement (k = 0.85) were observed. Poor inter-rater agreement was found for points 1.1 “inspiration” (k = 0.41), 1.2 “rotation and tilting” (k = 0.38) and 1.6 “diaphragm” (k = 0.40). Absolute agreement was found for the diagnostic value of cropped images. Overall ICC between observers was .99 at a 95% confidence interval from 0.99 to 0.99 (F(719,719) = 1.158, p < 0.0001). ICC for the intra-observer rating was also .99 at a 95% confidence interval from 0.99 to 0.99 (F(704,704) = 1.159, p < 0.0001).
Conclusion
The study strengthens the proposition to use the provided semi-automatic tool for time efficient audits, offering excellent validity for quantitative parameters and good informative value for qualitative parameters derived from the diagnostic requirements for chest radiographs according to the EC guidelines. The observed results lead to the conclusion that the diagnostic requirements defined by the EC guidelines for AP/PA chest radiography in paediatrics were only partially met. While inadequate field sizes and inspiration depths were discovered they remained within tolerance in general.
Debateable issues whether the qualitative criteria can be met due to subjective intepretation, and whether the EC guidelines are feasible for mobile unit examinations of PIC patients were observed. Quality criteria on “inspiration”, “rotation and tilting”, and “sharp diaphragm” revealed the lowest rates of satisfaction. While no diagnostic image should be rejected due to unsatisfactory image quality no directions are given on how the presence of clinical support devices and installations, or extensive pathologies affecting image quality should be interpreted (e.g.: poor visualisation of the diaphragm due to pleural effusion).
Low inter-rater agreement was found for the qualitative parameter “performed at peak inspiration”. It has been suggested to amend this point. Optimal inspiration depths according to three age groups were introduced: visibility of at least 10 posterior ribs above the diaphragm for patients older than six, 9 in children aged two to five, and 8 in children aged zero to two years was recommended. [5, 9-12] This suggestion gains stronger validity as similar results were re-produced for PICU patients in this study.
Redundancies had previously been reported for the points “vasculature” and “spine”, and were reproducible in this study strengthening the proposition to merge them. [5] Homogenous terminology for studies in paediatrics is needed, and in the narrower sense this includes radiographic terminology. [6, 13, 14] To a certain extent the EC guidelines fail to offer definitions for quality criteria that are not susceptible to subjective interpretation. In conclusion a review of the EC guidelines might be warranted.